Global Journal of Obesity, Diabetes and Metabolic Syndrome
Shaping Immune Responses by Dysregulated Adipokines in Obesity
The Hormel Institute, University of Minnesota, Austin, MN, USA
Author and article information
Cite this as
Zhang Y, Rao E, Li B (2015) Shaping Immune Responses by Dysregulated Adipokines in Obesity. Glob J Obes Diabetes Metab Syndr. 2014; 2(1): 35-37. Available from: 10.17352/2455-8583.000006
Copyright License
© 2014 Zhang Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Obesity is a major epidemic worldwide. According to the Centers for Disease Control and Prevention (CDC), about 34.9% of adults and 17% of children and adolescents are obese in the United States. The increasing prevalence of obesity poses a major threat to public health. Clinical and epidemiological data have established that obesity not only links to the development of diabetes, atherosclerosis and cardiovascular diseases, but also increases the risk of many types of cancer [1]. Although tremendous effort has been taken to investigate the pathogenesis of obesity and its associated diseases, the molecular mechanisms by which obesity negatively impacts on metabolic and immunologic homeostasisand increases the morbidity and mortality of many maladies remain largely unknown.
Obesity is a major epidemic worldwide. According to the Centers for Disease Control and Prevention (CDC), about 34.9% of adults and 17% of children and adolescents are obese in the United States. The increasing prevalence of obesity poses a major threat to public health. Clinical and epidemiological data have established that obesity not only links to the development of diabetes, atherosclerosis and cardiovascular diseases, but also increases the risk of many types of cancer [1]. Although tremendous effort has been taken to investigate the pathogenesis of obesity and its associated diseases, the molecular mechanisms by which obesity negatively impacts on metabolic and immunologic homeostasisand increases the morbidity and mortality of many maladies remain largely unknown.
Although obesity is attributed to the combination of both genetic and environmental factors, it commonly occurs due to the imbalance of excessive caloric intake and low energy expenditure [2]. Obesity is associated with accumulation of excess lipids in white adipose tissue and with a state of chronic low-grade systemic inflammation in the host. Once considered simply as sites of lipid storage, adipocytes in the adipose tissue are now recognized as important endocrine cells through their secretion of various types of soluble mediators named “adipokines”, such as leptin, adiponectin and resistin, etc. It is now believed that adipokines serve as “messengers” of adipose tissue, regulating energetic balance and coordinating innate and adaptive immune responses in vivo.
In the community of adipose tissue, residents are classically divided into lipid containing adipocytes and other stromal cells including endothelial cells and various types of innate and immune cell populations. In normal weight subjects, macrophages in adipose tissue are implicated in maintaining adipose homeostasis through phagocytosis of necrotic adipocytes and facilitation of adipocyte differentiation and proliferation. Through coordinating with other innate and adaptive cells, such as eosinophils and regulatory T cells (Tregs), in adipose tissue, macrophages exhibit an anti-inflammatory M2 phenotype by production of IL-10 and arginase, thereby sustaining insulin sensitivity and normal functions of adipocytes. In contrast, in obese patients, immune populations, macrophages in particular are remarkably increased in adipose tissues. Phenotypically, macrophages in obese adipose tissue express CD11c and produce large amounts of cytokines, such as TNFα, IL-1β, IL-6 and iNOS, displaying a pro-inflammatory M1 phenotype. Many studies further demonstrate that increased numbers of CD8+ T cells and Th1 cells in obese tissue contribute to the recruitment and M1-polarization of macrophages. Due to the overwhelming levels of lipids and proinflammatry cytokines, including TNFα and IFNγ, in obesity, the homeostatic balance of immunity and metabolism is disrupted, leading to dysregulated functions of adipocytes characterized by insulin resistance and unbalanced production of adipokines.
Among the dysregulated adipokines in obesity, adiponectin and leptin receive the most attention due to their implications in regulating insulin signaling, inflammation, and immune responses [3]. Numerous lines of experimental and clinical evidence have supported the notion that adiponectin mainly functions as a “good” adipokine by inhibiting inflammatory responses and improving insulin sensitivity in obesity. For instance, treatment with adiponectin has been shown to suppress NFκB signaling in endothelial cells and macrophages. Instead, deficiency of adiponectin in mice significantly increases TNFα levels in adipose tissue and in circulation [4-6]. In addition, obesity is always associated with reduced levels of circulating adiponectin, which increases the risk of many inflammatory metabolic diseases [7,8]. Conversely, leptin is considered as a “bad” adipokine due to its pro-inflammatory characteristic during obesity development. In obese adipose tissue, macrophages can be activated by increased levels of leptin, which binds leptin-receptor on macrophages, promoting production of TNFα and IL-1β. Leptin also enhances the production of IFNγ and IL-2 while suppressing the production of IL-4 by CD4+ T cells [9]. Given the opposing roles in inflammation and immune responses, adiponectin and leptin are proposed to function oppositely in many diseases, including metabolic diseases and multiple types of cancer [10].
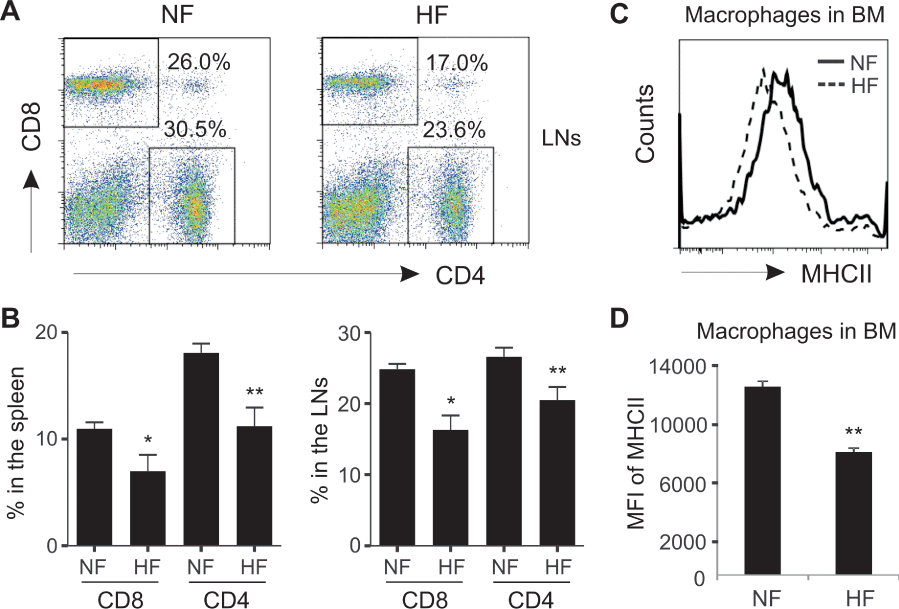
Recently, the links between obesity and cancer development have begun to be appreciated. Approximately 85,000 new cancer cases per year are related to obesity and 14%-20% of cancer mortality is due to obesity in the United States [11,12]. Although increased secretion of leptin and inflammatory cytokines and decreased secretion of adiponection in obesity are generally considered to contribute to the increased cancer risk, studies have shown inconsistent results [13-16], suggesting that other factors may also be involved. In our studies investigating obesity/cancer associations using high-fatdiet-induced mouse obese models, we put mice on a high-fat diet for at least half a year to closely mirror the chronic development of obesity in humans. We have demonstrated that obesity greatly reduces the expression of MHC II molecules on bone marrow macrophages in vivo. Moreover, obese mice exhibit significantly lower percentages of both CD4+ and CD8+ T cell in spleen, peripheral blood and lymph nodes as compared to lean mice (Figure 1). These new observations suggest that obesity greatly impairs both innate and adaptive immune responses, which may contribute to the unfavorable effects of obesity on cancer development. In exploring the possible molecular mechanisms in mediating these effects, we notice that obesity can greatly promote the circulating levels of adipose fatty acid binding protein (A-FABP). We speculate that A-FABP may serve as a new adipokine regulating immunologic and metabolic responses in obesity based on the following observations. 1) A-FABP is abundantly expressed in macrophages and adipocytes [17-19]. 2) In macrophages A-FABP modulates inflammatory responses through activation of nuclear factor κB (NF-κB) and c-Jun N-terminal kinase (JNK) pathways [18,20]. 3) In adipocytes A-FABP regulates lipid metabolism through interactions with proteins, such as hormone-sensitive lipase (HSL) and Janus kinase 2 (JAK2) [21-23]. 4) Circulating levels of A-FABP are positively associated with breast cancer progression [24]. Thus, studies from animal models and humans suggest that A-FABP, as a central regulator of both inflammatory and metabolic pathways, represents a new link underlying obesity/cancer associations.
It is worth noting that the FABP family consists of 9 different members, all of which exhibit tightly regulated patterns of tissue distribution. For example, intestinal FABP (I-FABP) is primarily expressed in intestine while epidermal FABP (E-FABP) exhibits a more ubiquitous expression pattern beyond just the epidermal skin cells [25-27]. Thus, each individual FABP member may display unique functions in different tissues depending upon where they are located and how they are regulated. Our previous studies showing that E-FABP plays distinct roles in different immune cells also support this new notion [28,29]. It will be of great interest to know how A-FABP, as a new adipokine, shapes host immune responses in obesity-related diseases, including cancer and other diseases.
Acknowledgements
This publication was made possible by funding from the Minnesota obesity grant (5P30DK50456) and NIH R01 grants (CA18098601A1, CA17767901A1).
- Johnson AR, JJ Milner, L Makowski (2012) The inflammation highway: metabolism accelerates inflammatory traffic in obesity. Immunol Rev 249: 218-238 .
- Pi-Sunyer F X (2002 ) The obesity epidemic: pathophysiology and consequences of obesity. Obes Res 10 2: 97S-104S .
- Tilg H, AR Moschen (2006) Adipocytokines: mediators linking adipose tissue, inflammation and immunity. Nat Rev Immunol 6: 772-783.
- Maeda N, I Shimomura, K Kishida, H Nishizawa, M Matsuda, et al. (2002) Diet-induced insulin resistance in mice lacking adiponectin/ACRP30. Nat Med 8: 731-737.
- Ouchi N, S Kihara, Y Arita, Y Okamoto, K Maeda, et al. (2000) Adiponectin, an adipocyte-derived plasma protein, inhibits endothelial NF-kappaB signaling through a cAMP-dependent pathway. Circulation 102: 1296-1301 .
- Ouchi N, S Kihara, Y Arita, M Nishida, A Matsuyama, et al. (2001) Adipocyte-derived plasma protein, adiponectin, suppresses lipid accumulation and class A scavenger receptor expression in human monocyte-derived macrophages. Circulation 103: 1057-1063.
- Maahs D M, L G Ogden, G L Kinney, P Wadwa, J K Snell-Bergeon, et al. (2005) Low plasma adiponectin levels predict progression of coronary artery calcification. Circulation 111: 747-753 .
- Mandel MA, AA Mahmoud (1978) Impairment of cell-mediated immunity in mutation diabetic mice (db/db). J Immunol 120: 1375-1377.
- Lord GM, G Matarese, JK Howard, RJ Baker, SR Bloom, et al. (1998) Leptin modulates the T-cell immune response and reverses starvation-induced immunosuppression. Nature 394: 897-901.
- Khandekar MJ, P Cohen, BM Spiegelman (2011) Molecular mechanisms of cancer development in obesity. Nat Rev Cancer 11: 886-895.
- Basen-Engquist K, M Chang (2011) Obesity and cancer risk: recent review and evidence. Curr Oncol Rep 13: 71-76.
- Calle EE, C Rodriguez, K Walker-Thurmond, MJ Thun (2003) Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med 348: 1625-1638 .
- Lukanova A, S Soderberg, R Kaaks, E Jellum, P Stattin (2006) Serum adiponectin is not associated with risk of colorectal cancer. Cancer Epidemiol. Biomarkers Prev 15: 401-402 .
- Stattin P, A Lukanova, C Biessy, S Soderberg, R Palmqvist, et al. (2004) Obesity and colon cancer: does leptin provide a link? Int J Cancer 109: 149-152 .
- Aparicio T, S Guilmeau, H Goiot, A Tsocas, JP Laigneau, et al. (2004) Leptin reduces the development of the initial precancerous lesions induced by azoxymethane in the rat colonic mucosa. Gastroenterology 126: 499-510.
- Soliman PT, X Cui, Q Zhang, SE Hankinson, KH Lu (2011) Circulating adiponectin levels and risk of endometrial cancer: the prospective Nurses' Health Study. Am J Obstet Gynecol 204: 167.
- Hunt CR, JH Ro, DE Dobson, HY Min, BM Spiegelman (1986) Adipocyte P2 gene: developmental expression and homology of 5'-flanking sequences among fat cell-specific genes. Proc Natl Acad Sci U S A 83: 3786-3790 .
- Makowski L, KC Brittingham, JM Reynolds, J Suttles, GS Hotamisligil (2005) The fatty acid-binding protein, aP2, coordinates macrophage cholesterol trafficking and inflammatory activity. Macrophage expression of aP2 impacts peroxisome proliferator-activated receptor gamma and IkappaB kinase activities. J Biol Chem 280: 12888-12895 .
- Reynolds JM, Q Liu, KC Brittingham, Y Liu, M Gruenthal, et al. (2007) Deficiency of fatty acid-binding proteins in mice confers protection from development of experimental autoimmune encephalomyelitis. J Immunol 179: 313-321 .
- Hui X, H Li, Z Zhou, KS Lam, Y Xiao, et al. (2010) Adipocyte fatty acid-binding protein modulates inflammatory responses in macrophages through a positive feedback loop involving c-Jun NH2-terminal kinases and activator protein-1. J Biol Chem 285: 10273-10280.
- Coe NR, MA Simpson, DA Bernlohr (1999) Targeted disruption of the adipocyte lipid-binding protein (aP2 protein) gene impairs fat cell lipolysis and increases cellular fatty acid levels. J Lipid Res 40: 967-972 .
- Thompson BR, AM Mazurkiewicz-Munoz, J Suttles, C Carter-Su, DA Bernlohr (2009) Interaction of adipocyte fatty acid-binding protein (AFABP) and JAK2: AFABP/aP2 as a regulator of JAK2 signaling. J Biol Chem 284: 13473-13480.
- Gorbenko O, G Panayotou, A Zhyvoloup, D Volkova, I Gout, et al. (2010) Identification of novel PTEN-binding partners: PTEN interaction with fatty acid binding protein FABP4. Mol Cell Biochem 337: 299-305.
- Hancke K, D Grubeck, N Hauser, R Kreienberg, JM Weiss (2010) Adipocyte fatty acid-binding protein as a novel prognostic factor in obese breast cancer patients. Breast Cancer Res Treat 119: 367-377.
- Furuhashi M, GS Hotamisligil (2008) Fatty acid-binding proteins: role in metabolic diseases and potential as drug targets. Nat Rev Drug Discov 7: 489-503 .
- Storch J, B Corsico (2008) The emerging functions and mechanisms of mammalian fatty acid-binding proteins. Annu Rev Nutr 28: 73-95.
- Davidson NO, CA Ifkovits, SF Skarosi, AM Hausman, X Llor, et al. (1993) Tissue and cell-specific patterns of expression of rat liver and intestinal fatty acid binding protein during development and in experimental colonic and small intestinal adenocarcinomas. Lab Invest 68: 663-675 .
- Zhang Y, Y Sun, E Rao, F Yan, Q Li, et al. (2014) Fatty acid-binding protein E-FABP restricts tumor growth by promoting IFN-beta responses in tumor-associated macrophages. Cancer Res 74: 2986-2998 .
- Li B, JM Reynolds, RD Stout, DA Bernlohr, J Suttles (2009) Regulation of Th17 differentiation by epidermal fatty acid-binding protein. J Immunol 182: 7625-7633.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
