Archives of Clinical Gastroenterology
Isolated Distal Pancreatic Transection Secondary to an Abdominal Blunt Trauma - A Case Report
Hepato-Pancreato-Biliary Surgical Unit, Department of Surgery, Hospital Universitario de Guadalajara, Guadalajara, Spain
Author and article information
Cite this as
Medina Velasco AA, Ramia JM, Peralta VA, Valenzuela J, López Marcano AJ (2016) Isolated Distal Pancreatic Transection Secondary to an Abdominal Blunt Trauma - A Case Report. Arch Clin Gastroenterol. 2016; 2(2): 53-55. Available from: 10.17352/2455-2283.000021
Copyright License
© 2016 Medina Velasco AA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Isolated pancreatic trauma (IPT) secondary to an abdominal blunt trauma, is an uncommon condition- IPT diagnosis usually is insidious, requiring the integration of multiple parameters, regarding anamnesis, physical examination, blood analysis and radiologic tests. Nowadays, exists controversy in the literature about management of the IPT. We report a case of a young male with a body-tail pancreatic transection, secondary to an abdominal blunt trauma. Distal pancreatectomy with spleen preservation was performed with successful postoperative course. We discuss diagnostic and therapeutical options in IPT.
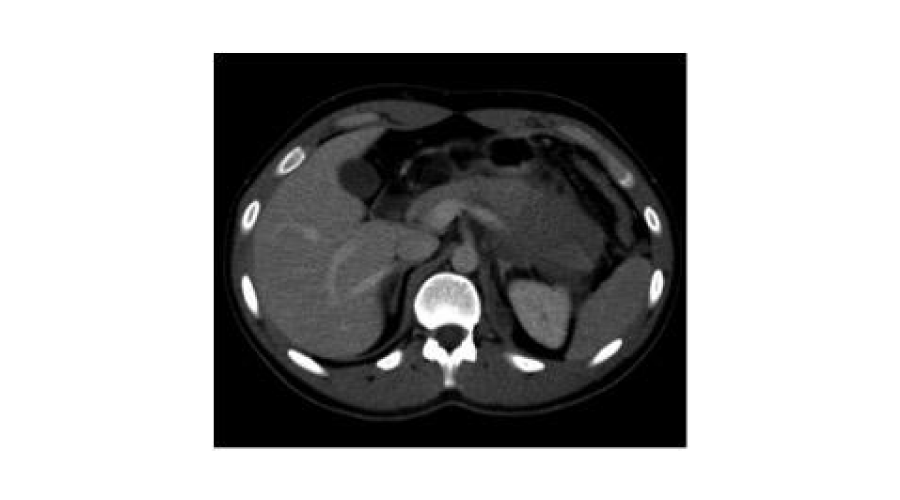
A 21 years old young male presented to the emergency room (ER) after a motorcycle accident. He had no remarkable past medical history. He suffered a thoracic inferior and abdominal blunt trauma with the handle. Glasgow coma scale: 15 points, HR: 78 B.P.S., Arterial Pressure: 110/70 mmHg, SpO2: 98%. At the examination, his abdomen was soft with pain in left hypochondrium and left lumbar region, with a haematoma in the left lumbar region. No signs of peritonism were present. Laboratory studies were significant for leukocytes 22,600 μL-1 and elevated amylase of 216 U/L. Computed tomography (CT) of abdomen and pelvis demonstrated the complete transection of the body of the pancreas with peripancreatic fluid of 6 x 5.5 cm, leading extension to all the bursa omentalis, perisplenic and left perirenal región, towards to left psoas major muscle (Figure 1).
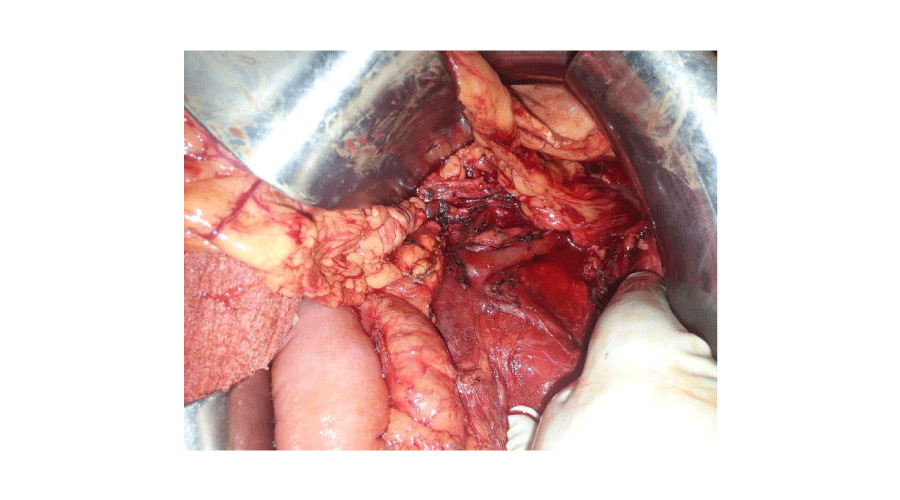
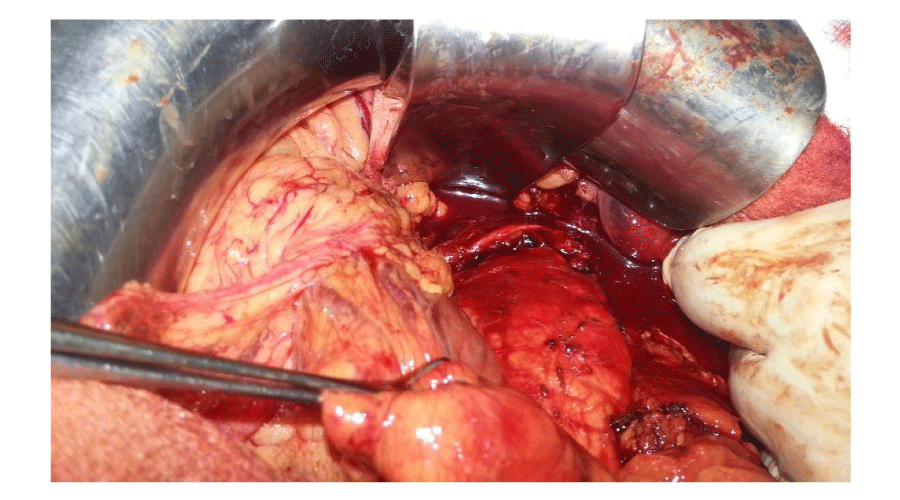
In the operation room was confirmed the complete section of the pancreas body-tail with a 2 cm laceration proximal to the section (Grade III and Grade I AAST) (Figure 2), requiring a distal pancreatectomy, performing a preservation of the splenic vessels. The proximal part of the pancreas was closed with an EndoGia™ (60mm) and reinforced with a running suture, also an omentoplasty was performed (Figure 3). Microbiological tests of samples were negative. He left the hospital 12 days after admission. Pathology evidenced normal parenchyma with necrosis in small scattered areas. During a 12-month follow-up, the patient did not show any complications.
Discussion
Travers, was the first who described a rupture of the pancreas ought to an abdominal blunt trauma [1]. It is necessary for a high velocity impact to occur, and the mechanism appears to be related to the compression of the organ to the vertebral column during the impact [2-4]. Pancreatic trauma shows up in the 1-5% of the abdominal blunt trauma (developed as an IPT in less of 1%), this prevalence turns higher (12%) in the penetrating abdominal trauma. Morbidity and mortality are high in the pancreatic trauma (30-60% and 10-30% respectively) [1-6].
Approximately the 65% of pancreatic lesions occurs in the neck and body the remaining ones, take place at the head and tail [3]. Around the 90% of the patients with pancreatic trauma shows up concomitant small bowel lesions, and because of the anatomic proximity and irrigation sharing, duodenal lesions are the most common, as well as vascular structures [1,3,5,7]. Exist a 5-grade classification (AAST) of the pancreatic trauma describing the presence of hematoma, laceration, site of lesion and the integrity of the pancreatic duct and its complications [8]. In most of the cases, late deaths are from infection and sepsis, generally from pancreatic or hollow viscus injury [5].
The diagnosis of the pancreatic trauma, specially IPT, used to be difficult: non-specific symptoms due to retroperitoneal location of the pancreas, elevations in serum amylase and lipase are not reliable to determine pancreatic injuries, radiological tests lacks of specificity [2,5,9,10], that is why sometimes diagnosis occurs as an incidental finding at the time of a laparotomy, ought to repair other associated lesions [1-3]. There is a great increment of the morbid-mortality when the delay is more than 24 hours, appearing in almost one-third of the cases complications as: 1) Pseudocysts, 2) Abscesses, 3) Hemorrhage, 4) Fistulae or 5) Sepsis and multi system organ failure [1,3].
Elevations in serum amylase and lipase are not reliable to determine pancreatic injuries, but may serve as an indicator of the probable pancreatic injury [1,2,7]. Elevated levels of amylase occurs around the 66-90% of the pancreatic trauma secondary to a blunt abdominal trauma, but could be normal at the early stage. There is no correlation between levels of amylase and grade of pancreatic injury [1].
Ultrasound scan (US) is considered to be useful for the detection of free intraperitoneal fluid or a large hematoma, but its ability to show a specific injury of the pancreatic duct is limited because of its retroperitoneal localization. It is a low cost noninvasive test, submitting findings in real time [2,7]. In children the utility of the US appears to be higher [11]. Sato et al. demonstrate that the 80% of the ductal lesions are diagnosticated by abdominal US in experts’ hands [12].
Computed tomography (CT) is the best diagnostic modality for pancreatic trauma in stable conditions patients [1-3]. Sensibility is between 60-85%, being lower (43%) to demonstrate the integrity of the pancreatic duct [1,3,4]. On CT, direct signs of pancreatic injury include: (1) glandular contusion, (2) laceration, and (3) transection (lacerations that involves 50% of the thickness of the pancreas have a risk of involving the main duct). Indirect signs are: (1) peripancreatic fluid in the lesser sac, (2) pancreatic hematoma or partial laceration, (3) diffuse gland enlargement with pancreatitis or focal edema at the site of injury, and (4) thickening of the left anterior renal fascia [1-3].
If the diagnosis is unclear, the magnetic resonance cholangiopancreatography (MRCP) is an alternative diagnosis method to the CT and superior than endoscopic retrograde cholangiopancreatography (ERCP) evaluating the integrity of the pancreatic duct, being less invasive, faster, reachable, and more sensitive (by stimulation with secretin). In addition, MRCP pancreatography may demonstrate abnormalities not visible at ERCP, such as fluid collections upstream of the site of duct transection, and is helpful in assessing parenchymal injury [3,7,13]. ERCP is recommended as a therapeutic skill, not for the diagnosis, having a great sensitivity and specificity [1,3].
The integrity of the pancreatic duct is the principal factor principal factor that needs to be consider to decide the treatment, being an important morbidly determinant as well [1-3,7]. If a disruption of the duct is detected, therapeutics must take place as fast as possible (Surgery or endoscopy). Under these conditions, a treatment delay of more than 24 hours, duplicates or triplicates morbidity. If the indemnity of the duct is proved, expectant actitud can be used [1,3,6]. Intraoperatory Indicators suggestive of ductal injury are: Complete transection of the pancreas, direct visualization of ductal injury, central perforation, or severe maceration [5].
Surgical treatment depends of the localization of trauma, grade of pancreatic duct disruption and AAST level. Injury to the pancreatic head is best manageable by drainage and, in some cases, by staged Kausch-Whipple procedure. For rupture at the level of the pancreatic body and tail (most frequently seen following blunt abdominal trauma), most surgeons choose to perform a distal pancreatectomy (PD), which may be combined with Roux-en-Y pancreaticojejunostomy to reduce the risk of postoperative pancreatic fistula [6,14]. Because of the intimal anatomic relation with the spleen, PD frequently is accompanied by a splenectomy [15]. We want to highlight that our PD was with preservation of splenic vessels, decreasing the immunological compromise that splenectomy causes.
Other type of surgical treatments has been reported with good results. Kris et al. [6], reported a case of a Head-neck pancreatic transection secondary to an abdominal blunt trauma, with the ductal section ventral to the Mesenteric superior vein. A central pancreatectomy with a distal pancreatoyeyunostomy was performed, good results were obtained at the postoperative course. The benefit of this surgical technique is the preservation of the distal pancreatic tissue, avoiding the drastically decrease of endocrin/exocrin function.
To conclude, isolated pancreatic transection secondary to an abdominal blunt trauma is an infrequent condition, it used to be associated to other intraabdominal organ lesions. Diagnosis usually is insidious, requiring the integration of multiple parameters, regarding anamnesis, physical examination, blood analysis and radiologic tests. Early diagnosis and treatment are the best way to get a successful outcome and decrease of the mobility and mortality.
- Oteiza F, Diaz de Liaño A, Ciga MA, Ortiz H (2003) Rotura pancreática aislada diagnosticada por TC en un traumatismo cerrado. Cir Esp 74: 296-298 .
- Tsai MT, Sun JT, Tsai KC, Lien WC (2010) Isolated traumatic pancreatic rupture. Am J Emerg Med 28: 745-746 .
- Holalkere NS, Soto J (2012) Imaging of miscellanous pancreatic pathology (trauma, transplant, infections and deposition). Radiol Clin N Am 50: 515-528 .
- Fisher M, Brasel K (2011) Evolving management of pancreatic injury. Curr Opin Crit Care 17: 613-617.
- Peitzman AB, Richardson JD (2010) Surgical treatment of injuries to the solid abdominal organs: a 50-year perspective from the Journal of Trauma. J Trauma 69: 1011-1021 .
- Kreis ME, Albertsmeier M, Graser A, Krenz D, Jauch KW, et al. (2011) Novel surgical technique for complete traumatic rupture of the pancreas: A case report. J Med Case Rep 5: 456 .
- Govaert MJ, Ponsen KJ, de Jonge L, de Wit LT, Obertop H (2001) Fracture of the pancreas in two patients after a go-kart accident. HPB Oxford 3: 3-6 .
- Moore EE, Moore FA (2010) American Association for the Surgery of Trauma Organ Injury Scaling: 50th anniversary review article of the Journal of Trauma. J Trauma 69: 1600-1601 .
- Bradley EL 3rd, Young PR Jr, Chang MC, Allen JE, Baker CC, et al. (1998) Diagnosis and initial management of blunt pancreatic trauma. Ann Surg 227: 861-869 .
- Stawicki SP, Schwab CW (2008) Pancreatic trauma: demographics, diagnosis, and management. Am Surg 74: 1133-1145 .
- Healey AJ, Dimarikis I, Pai M, Jiao LR (2008) Delayed presentation of isolated complete pancreatic transection as a result of sport-related blunt trauma to the abdomen. Case Rep Gastroenterol 2: 22-26 .
- Sato M, Yoshii H (2004) Reevaluation of ultrasonography for solid-organ injury in blunt abdominal trauma. J Ultrasound Med 23: 1583-1596 .
- Gillams AR, Kurzawinski T, Lees WR (2006) Diagnosis of duct disruption and assessment of pancreatic leak with dynamic secretin-stimulated MR cholangiopancreatography. AJR Am J Roentgenol 186: 499–506 .
- Wagner M, Gloor B, Ambühl M, Worni M, Lutz JA, et al. (2007) Roux-en-Y drainage of the pancreatic stump decreases pancreatic fistula after distal pancreatic resection. J Gastrointest Surg 11: 303-308 .
- Shi N, Liu SL, Li YT, You L, Dai MH, et al. (2015) Splenic Preservation Versus Splenectomy During Distal Pancreatectomy: A Systematic Review and Meta-analysis. Ann Surg Oncol 23: 365-374 .
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
