Superior Patellar Sleeve Fracture: A case report and review of the published evidence
Wrightington Hospital, Hall Ln, Appley Bridge, Wigan, WN6, 9EP, UK
Author and article information
Cite this as
Yassa R, Oputa TJ, McNair M, Michaud R (2019) Superior Patellar Sleeve Fracture: A case report and review of the published evidence. Open J Trauma. 2019; 3(1): 3-5. Available from: 10.17352/ojt.000018
Copyright License
© 2019 Yassa R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Patellar fractures are uncommon, accounting for only 2% of all fractures [1]. Sleeve fractures were first reported in 1978 by Houghton and Ackroyd and occur predominantly in children. This fracture results in the inferior sleeve of articular cartilage being avulsed along with the periosteum and retinaculum from the patella. Inconsistently the avulsed fragment can contain a small bony component. [2,3].
Patellar fractures are uncommon, accounting for only 2% of all fractures [1]. Sleeve fractures were first reported in 1978 by Houghton and Ackroyd and occur predominantly in children. This fracture results in the inferior sleeve of articular cartilage being avulsed along with the periosteum and retinaculum from the patella. Inconsistently the avulsed fragment can contain a small bony component. [2,3].
Sleeve fractures have been described from the superior boarder of the patella although this injury is classically from the inferior pole [4,5]. These fractures occur almost exclusively in children and adolescents with a peak incidence at 12.7 years [6]. They are rare, accounting for only 1-6.5% of all paediatric fractures [6]. A study examining patellar fractures in children found that sleeve fracture was the most common type of patellar fracture observed, and accounting for 57% of paediatric patellar fractures [7]. The incidence in the younger age group is thought to be due to the osteochondral change and growth pattern of the patella as well as an increased involvement in sporting activity [8]. It is typically a non-contact injury [4].
Superior sleeve fractures are very uncommon in comparison to inferior fractures. A literature search yielded only eight papers documenting cases of superior fracture were found in English literature and two in German and Belgian papers since 1991 [5,8-16]. These cases include adults as well as children due to various aetiology.
The diagnosis of a sleeve fracture can be easily missed. A combination of history, examination and radiological studies has proven to be the most effective way of managing theses cases. On examination, the patient presented with local pain, tenderness, swelling and an inability to fully extend the knee actively. Haemarthrosis is a common finding [5,17].
Plain x-ray film is important in the diagnosis however with small fragments or avulsions with a large cartilaginous component, the injury can be difficult to visualise [4,5,18]. Soft tissue swelling may be visible indicating a haemarthrosis and significant trauma which should be investigated further [4]. Several papers have examined other imaging methods and concluded that magnetic resonance imaging (MRI), and ultrasonography (USS) are of benefit [19,20].
Case Report
The patient involved is fit and healthy eight-year-old boy on holiday who fell whilst playing on a push scooter on a paved area. He did not have any past medical history of note and he was not taking any medication. He had accelerated quickly and then braked causing the scooter to skid and turn. He described sliding down the scooter, twisting awkwardly, and then hitting the ground with his right knee. There was no open wound recorded. On examination, his knee was tender to palpation with soft tissue swelling. There was a definite effusion present and a palpable gap was noted over the quadriceps tendon. He had a reduced range of movement in the joint and could not perform a straight leg raise.
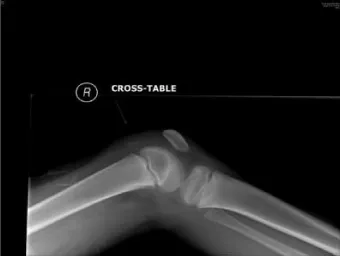
Plain X ray films revealed an anteriorly angulated low lying patella with a small bony fragment seen adjacent to the right distal femoral physis visible on the lateral view. There was an associated soft tissue swelling also noted in the affected area (Figure 1).
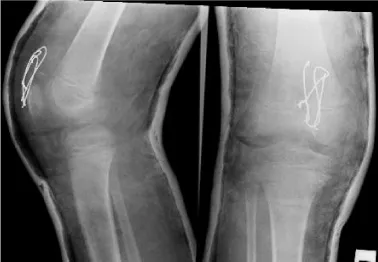
The patient was treated for the superior sleeve fracture surgically. This was accomplished through a midline incision. The fracture of the superior pole of the patella was identified with some fragmentation. The fracture was stabilised with two 1.0mm K wires and tension band wiring. Postoperatively, a plaster cylinder was applied for 6 weeks (Figure 2). The patient was allowed to bear weight.
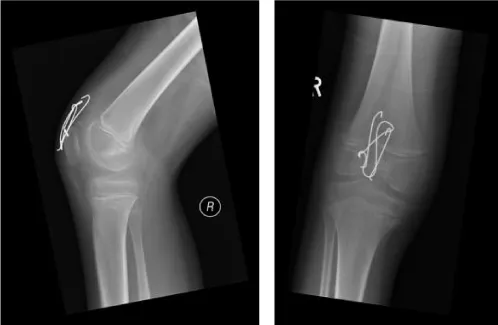
Latest follow up has shown full recovery with return of full knee range of movement and function at 5 months postoperatively following an intense physiotherapy program (Figure 3).
Discussion
The patella in children is particularly cartilaginous with ossification beginning only between 3-6 years of age (6). Ossification occurs in small islands that expand to the periphery. The immature patella can withstand trauma impact and tactile force due to a protective surface cartilage layer and and increased mobility compared to the developed patella [5]. Sleeve fractures occur in the paediatric population due to the cartilaginous composition of the patella. The sleeve is avulsed more frequently than tendon rupture as this is felt to be the weaker component, with the tendon collagen fibres at insertion being indistinct from the cartilaginous sleeve [21].Although sleeve fractures typically occur as the result of a non-contact injury, it can also occur as the result of falls and trauma as seen in this case [9,16]. The classical mechanism of injury for inferior fractures is thought to be due to forceful quadriceps contraction with flexion of the knee, resulting in separation of the sleeve from the patella. However, in superior sleeve fractures Klerx-Melis et al postulated that certain knee flexion causing more force to be transmitted through the superior pole compared to the inferior pole [13]. Jumping sports such at hurdles, high jump and basketball are all associated with sleeve fractures affecting the take off leg [3,4].
Sleeve fractures can be easily missed on plain x-rays film due to the bony component being either very small or not present. Further imaging is recommended especially in uncertain cases with high clinical suspicion. MRI and USS have both been demonstrated to be of use in diagnosis. In MRI, T2 weighted images can be used to evaluate the extent of the injury to the cartilaginous sleeve and assist in planning further management. Bates et al demonstrated the sleeve avulsion successfully and were able to define inter-articular involvement of the injury using MR imaging [19].
Other than sporting injuries some studies have suggested association of sleeve fractures with post surgical recovery from certain procedures as well as with certain chronic medical conditions. Brennan et al postulated that there was a link between patellar stabilization surgery and compromised vascularisation to the proximal pole of the patella resulting in an increased risk of this injury in the post operative period. This has not been formally researched and Brennan et al state that this is unlikely due to these fractures being so rare compared to the instability treatment group and may be more likely linked to post surgical immobilization instead [10]. Kumar and Knight similarly presented a case of superior sleeve fracture which occurred following a fall soon after removal of cylinder cast for patellar dislocation [5].
Some adult cases have been presented in patients with osteogenesis imperfecta and in patient following cast immobilisation, however it is controversial as to whether this is a true sleeve fracture due to the patella having fully ossified in the mature skeleton [22].
Surgical management of sleeve fractures constitutes open reduction and internal fixation. Several successful methods have been documented including suturing and bone anchors, tension banding, and figure eight suturing [5,9,10]. Hunt and Somashekar noted that fixation was less certain when no osseous component was present [2]. Nevertheless, there is no randomised controlled trial to give us guidance on the best modality of fixation in this particular kind of injury. It is mainly based on the surgeon’s preference.
Conclusion
In summary, superior sleeve fractures are a very rare injury but should be considered in children and adolescents who present with pain, effusion and extensor weakness in both non-contact and contact trauma. In cases with inconclusive plain film imaging, due to the small bony fragment and larger cartilaginous component associated with this type of injury, MRI and USS have been demonstrated to be of clinical use in managing these cases and determining the extent of the injury. Following a review of previous literature, operative management with internal fixation is recommended to prevent complications associated with conservative management, such as quadriceps weakness, patella elongation or duplication and long term mobility issues.
- Bostrom A (1972) Fracture of the Patella: A Study of 422 Patellar Fractures. Journal Acta Orthopaedica Scandinavica 43: 1-80. Link: https://tinyurl.com/yyymn9d4
- Hunt DM, Somashekar N (2005) A review of sleeve fractures of the patella in children. Knee 12: 3-7. Link: https://tinyurl.com/y3qsjky8
- Houghton GR, Ackroyd CE (1979) Sleeve fractures of the patella in children: a report of three cases. J Bone Join Surg 61-B: 165-168. Link: https://tinyurl.com/y6z4oqrw
- Strahan R (2009) Non-contact paediatric knee injuries, including patellar sleeve fractures. J Med Imaging Radiat Oncol 52: 544-549. Link: https://tinyurl.com/y49kcnv6
- Kumar K, Knight DJ (2005) Sleeve fracture of the superior pole of the patella: a case report. Knee Surg Sports Traumatol Arthrosc 13: 299-301. Link: https://tinyurl.com/yyrpzt5x
- Ray JM, Hendrix T (1992) Incidence, mechanism of injury and treatment of fractures of the patella in children. J Trauma 32: 464-467. Link: https://tinyurl.com/y375cncb
- Dai LY, Zhang WM (1999) Fractures of the patella in children. Knee Surg, Sport Traumatol, Arthrosc 7: 243-245. Link: https://tinyurl.com/yy3rwpzv
- Khanna G, El-Khoury GY (2007) Sleeve fracture at the superior pole of the patella. Pediatr Radiol 37: 720-723. Link: https://tinyurl.com/y2w2qg4n
- Bishay M (1991) Sleeve fracture of upper pole of patella. J Bone Joint Surg Br 73: 339. Link: https://tinyurl.com/y3vd4c28
- Brennan S, Walls R, Jackson M, Moran R (2009) Superior pole sleeve fracture following patellar stabilisation. The Knee 16: 235-237. Link: https://tinyurl.com/y3qqutl2
- Bimmel R, Reddy K (2008) Quadriceps tendon rupture and periosteal sleeve avulsion fracture of the proximal patella pole in and active adolescent. Orthopaedics 31: 716. Link: https://tinyurl.com/yxp2zefv
- Maripuri SN, Mehta H, Mohanty K (2008) Sleeve fracture of the superior pole of the patella with an intra-articular dislocation. A case report. J Bone Joint Surg Am 90: 385-389. Link: https://tinyurl.com/y5yfdlms
- Kelerx-Melis F, Watt I (2006) The mechanism and diagnosis of a sleeve fracture of the upper pole of the patella in children. Eur J Radiol Extra 59: 67-70. Link: https://tinyurl.com/y4vv9uxx
- Gettys FK, Morgan RJ, Fleischli JE (2010) Superior pole sleeve fracture of the patella. A Case Report and Review of the Literature. Am J Sports 38: 2331-2336. Link: https://tinyurl.com/y6d9ty5a
- Van Isacker T, De Boeck H (2007) Sleeve fracture of the upper pole of the patella: a case report. Acta Orthop Belg 73: 114-117. Link: https://tinyurl.com/y3zcqhq3
- Kaivers P, Busch T, Lies A (2003) An avulsion (sleeve) fracture of the proximal patella pole in a child. Diagnosis, treatment and results in a patient after a fall onto the knee. German Unfallchirurg 106: 676-679. Link: https://tinyurl.com/y3v47p3x
- Wu CD, Huang SC, Liu TK (1991) Sleeve fracture of the patella in children: A report of five cases. Am J Sports Med 19; 525-528. Link: https://tinyurl.com/y378ex9x
- Nath PI, Lattin GE (2010) Patellar sleeve fracture. Pediatr Radiol 40: s53. Link: https://tinyurl.com/y62khhjo
- Bates DG, Hresko MT, Jaramillo D (1994) Patellar sleeve fracture: demonstration with MR imaging. Radiology 193: 825-827. Link: https://tinyurl.com/yxg5pwn4
- Ditchfield A, Sampson MA, Taylor GR (2000) Case Report: Ultrasound diagnosis of sleeve fracture of the patella. Clin Radiol 55: 721-722. Link: https://tinyurl.com/y29d5muo
- Peterson L, Stener B (1976) Distal disinsertion of the patellar ligament combined with avulsion fractures at the medial and lateral margins of the patella. Acta Orthop Scand 47: 680-685. Link: https://tinyurl.com/y49xzyav
- Kakazu T, Tatemoto H, Kawamura M, Sugita T (2003) Sleeve fracture of the upper pole of the patella in an adult with osteogenesis imperfecta. Injury 34: 793-794. Link: https://tinyurl.com/y3jcs2ds
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
