Psychological and attitudinal assessment of patients with Fibromyalgia undergoing antalgic management: a short report
1Department of Medicine and Surgery, University of Turin, Torino, Italy
2Anesthesia and Pain Medicine Unit, Department of Emergency and Urgency, Policlinico S. Orsola-Malpighi Hospital, Bologna, Italy
3Department of Medical and Surgical Science, Psychiatry Unit, Alma Mater Studiorum Università di Bologna, Bologna, Italy
4Department of Mental Health and Pathological Addiction, Local Health Authority, Bologna, Italy
5Department of Medicine and Surgery Sciences, University of Bologna, Bologna, Italy
Author and article information
Cite this as
Balzani E, Fanelli A, Tarricone I, Muratori R, Campesato M, et al. (2022) Psychological and attitudinal assessment of patients with Fibromyalgia undergoing antalgic management: a short report. Open J Pain Med. 2022; 6(1): 24-29. Available from: 10.17352/ojpm.000031
Copyright License
© 2022 Balzani E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Objectives: Fibromyalgia (FM) is a widespread condition that is difficult to manage medically. Often algologists are faced with patients who are poorly compliant with pharmacological treatment or with concomitant mood problems. There are treatments tailored to temperament and character patterns. In this study using the division into pain persistence and pain avoidance patterns, a stratification was hypothesized to facilitate its medical management using self-administered questionnaires.
Methods: We screened the population consisting of FM patients to four different questionnaires, namely the Temperament and Character Inventory (TCI), Hospital Anxiety and Depression Scale, Short form 36 and the INTERMED- Self Assessment.
Results: A total of thirty-two patients were enrolled. The analyzed population showed preponderant pain avoidance characteristics (90.7%). The persistence pattern proved to be present in only 9.3% of the population. The FM patients examined also reported an incidence of anxiety disorder of 71.9% and depressive disorder of 75%.
Conclusion: Dividing the population with FM into patterns yielded uniform results. This justifies a multidisciplinary approach in these FM patients. The high incidence of anxiety and depression from the test results is an outcome that suggests the adoption of the HADS tool in the antalgic evaluation of FM patients.
Fibromyalgia (FM) is a broad-spectrum syndrome characterized by a wide range of symptoms (Table 1) [1]. FM has a prevalence between 2%-3% and 8% [2]. Between 10% and 30% of FM, patients declare themselves impaired in work, which is a higher proportion compared to chronic pain patients [3].
Because FM’s underlying pathophysiology is not yet well understood, there are currently no effective treatments for the complete remission of FM symptoms [4]. Due to its symptoms variability, a purely clinical diagnosis, and the lack of agreement on treatment, a specific care pathway was not yet defined leading to a discontinuity in FM patients’ treatment [5]. A multidisciplinary therapeutic approach is therefore suggested, based on an individualized program including pharmacological and non-pharmacological interventions, involving general practitioners, algologists, psychiatrists, and physiatrists, coordinated by rheumatologists [6].
Furthermore, depression affects 28%-70% of FM patients, while anxiety disorders have a prevalence approximately of 32.3% [7]. Psychic disorders affect physical activity, work, and quality of life by favoring disadaptive psychological mechanisms, such as catastrophizing [8]. Besides, they can affect the quality of life, conditioning social and work activity, and hinder therapeutic success. Personalized treatment may benefit from the characterization of patients in specific cognitive-behavioral patterns, contributing to the maintenance and exacerbation of painful symptoms and related disabilities [9,10]. Van Koulil, et al. provided a cognitive-behavioral characterization for FM patients: Pain Persistence Pattern (PPP) with poor acceptance of the limits imposed by chronic pain, associated with a worsening of symptoms, and Pattern Pain Avoidance (PAP) with damage avoidance, fear of pain, hypervigilance, and catastrophism. These cognitive-behavioral traits seem to be associated with the maintenance and exacerbation of pain and their early detection could influence algological management [11].
Our study aimed to describe the incidence of depression, anxiety, PPP, and PAP in patients with FM, to evaluate whether particular patterns prevailed over others, establishing a viable tool to facilitate patients’ pain management and evaluation within a multidisciplinary pathway.
Materials and methods
Study design and participants
This exploratory retrospective cohort study was drawn up following the Strengthening the Reporting of Observational Studies in Epidemiology checklist [12]. The study was approved by the Ethics Committee of the Sant’Orsola-Malpighi Hospital of Bologna (169/2019/Oss/AOUBo) and by clinicaltrials.gov (NCT04623827).
This is a retrospective, monocentric, non-pharmacological study evaluating the incidence of depression, anxiety, and PPP and PAP through the use of self-administered questionnaires in FM patients referring to the Pain Therapy unit of Policlinico Sant’Orsola-Malpighi of Bologna and aged from 18y in the period from January 2018 to January 2019.
All subjects provided informed consent. Anonymized data were used to fill in a standardized template. Participation in the study did not interfere with the normal treatment for each patient, as the therapeutic plan represented normal daily clinical practice and was carried out regardless of patient enrollment.
Psychometric instruments and statistical methods
Participants were asked to complete the following instruments:
- Temperament and Character Inventory (TCI) [13]
- Hospital Anxiety and Depression Scale (HADS) [14]
- Short form 36 (SF-36) [15]
- INTERMED- Self Assessment (IMSA) [16]a
A total average time of 40 minutes was required to complete the tests. Being completely self-administered, after receiving the appropriate instructions, the patient was invited to compile tests autonomously or, if requested, was helped by a healthcare professional or family members.
Being completely self-administered, after receiving the appropriate instructions, the patient was invited to compile tests autonomously or, if requested, was helped by a healthcare professional or family members.
The temperament and Character Inventory (TCI) is a self-administrable questionnaire developed to quantify individual differences within temperament and character domains. Each of the main components consists of various subdimensions, which are probed by specific items. This test is validated and has also been used in cohorts of patients with FM [17].
The Hospital Anxiety and Depression scale (HADS) is a questionnaire used in clinical practice to identify mood disorders, namely anxiety, and depression. Its use has been validated in a population with FM [18].
Short Form 36 (SF-36) is a tool used to detect a patient’s health-related quality of life (HRQoL). This test is validated in the Italian language for FM [19].
The INTERMED-Self Assessment questionnaire (IM-SA) is the self-administrable version of INTERMED. This type of test has also been shown to be valid in patients with chronic painful conditions, and psychiatric settings [20].
The sociodemographic characteristics of our population such as gender have been synthesized using mean and standard deviation for continuous variables.
Due to the descriptive nature of the study, scores were reported for each test using mean, median, interquartile range, and standard deviation.
Statistical analysis
The sociodemographic characteristics of our population such as age and gender have been synthesized using mean and standard deviation for continuous variables (mean or median, standard deviation or interquartile range according to the Shapiro-Wilk normality test).
Due to the descriptive nature of the study, we reported the mean and the respective score for each test.
Results
In the cohort of the population studied (n = 32), 5 were males and 27 were females.
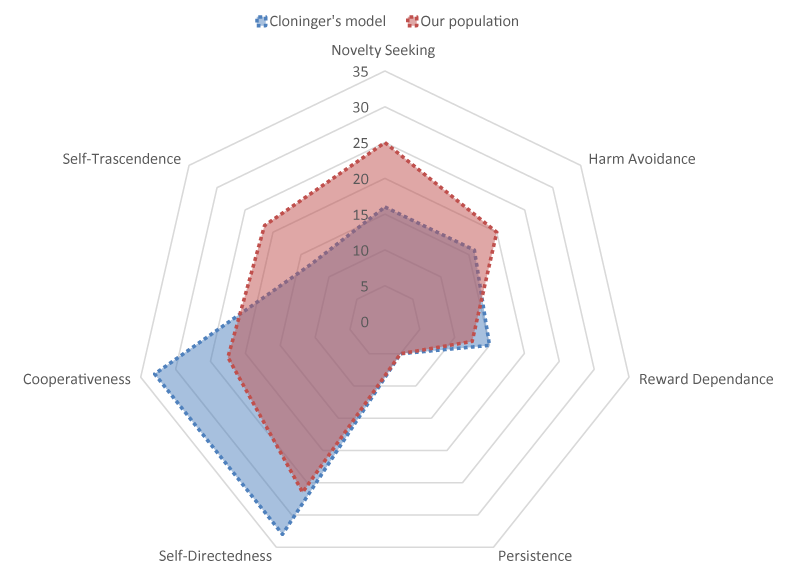
All the patients completed the TCI questionnaire, which scores were examined and compared with the median of the healthy population given by Cloninger [21]. The distribution of our population was examined by dividing it into quartiles for each domain.
Based on the results of the median of the general population 9.3% (n = 3) had values below the baseline for the Harm Avoidance (HA) domain. On the other hand, considering the Persistence (P) domain 59.4% (n = 19) patients had values below the general median (Figure 1).
Thus, compared to the general population 100% of our population had results above the median in the Novelty Seeking (NS) domain, 91% in the HA domain, 28% in the Reward Dependence domain, 41% in the P domain, 3% in the Self-Directedness domain, 0% in the Cooperativeness domain, and 94% in the Self Transcendence domain.
Regarding the HADS questionnaire, according to the results of the HADS questionnaire, 71.9% (n = 23) of our population would have anxiety disorders, while 75% (n = 24) would have depressive disorders (Table 2).
Considering the IMSA questionnaire, 65.6% (n = 21) had a total score ≥18 indicative of high complexity and need for integrated biopsychosocial care. However, when evaluating the various domains divided over time, only 6.3% (n = 2) scored ≥ 18 in the past and present, and 0% in the future. According to the SF-36 questionnaire, the mean for our population was always below that of the overall mean [22] (Table 2).
Discussion
This study reported a high prevalence of PAP among patients with FM, detected through four questionnaires.
The clear preponderance of the PAP could predispose patients to poor collaboration with healthcare providers and low compliance in the long term.
Overall, the questionnaires proved to be user-friendly, inexpensive, and well-accepted tools by patients (99% of patients completed them).
TCI questionnaire’s findings pointed out a tendency to avoid stressors, anticipatory anxiety, and a negative thought propensity in response to chronic pain, emphasized by an impulsive and unregulated attitude [23].
Regarding the Character results, we highlighted a fragile character, characterized by aimlessness, ineptitude, and lack of self-control [22] associated with traits of hostility and poor empathy [24]. High scores in the Self-Transcendence domain were associated with borderline, narcissistic, and paranoid personality disorders [25]. Based on our results, the persistence (P) domain represents an exception. In the context of a chronic disease such as FM, P is a fundamental trait for adequate compliance and patient management.
Specific approaches based on psycho-attitudinal characteristics and cognitive-behavioral therapy are tailored to improve pain symptoms, treatment compliance, and anxiety-depressive disorder in PAPs [11].
HADS questionnaire evaluation revealed a high percentage of patients with scores compatible with an anxiety-depressive disorder. This finding confirms the high prevalence reported in the literature and imposes the need for specialized psychiatric evaluation of FM patients within multidisciplinary management [8].
SF-36 test results showed that the patients had a lower quality of life than the average of the healthy population, both from the physical and mental points of view [23]. Lastly, the IMSA test remarked the need for integrated biopsychosocial care: most of the patients in our sample had scores indicative of high management complexity.
These findings suggest a polarization in the character, temperament, and mood of our population. As chronic conditions such as chronic pain were often associated with mood disorders [26], we question whether these alterations are characteristic of our population or the general chronic pain population.
Moreover, these comorbidities are associated with greater disability one year after the onset of chronic pain, making early detection critical for the algologist [27].
A potential limitation of the study we conducted is the small sample size examined, which could influence this result.
In conclusion, this study confirms the usefulness of using these self-administered questionnaires. Our results showed a consistent trend toward the PAP for which cognitive-behavioral therapy proved usefulness, improving poor cooperativeness behaviors, and enhancing patients’ compliance.
The high association between FM and anxiety-depressive disorders is confirmed by using the HADS questionnaire, which has proven to be a useful tool to identify pathological traits of mood that, however, require a specific diagnosis. Consequently, our results confirm the need for a multidisciplinary approach tailored to the patient.
Further studies may consider this type of assessment in patients with chronic pain. If the results were like those in our FM population, early detection of mood disorders and behavioral characteristics would lead to the identification of those most susceptible to poor compliance with antalgic therapy and those who should be started on an early psychiatric evaluation. The role of PPP in the FM and chronic pain population should also be clarified.
- Mease PJ, Seymour K. Treatment options for fibromyalgia. Pain Pract 18: 26-35.
- Goldenberg DL. Clinical manifestations and diagnosis of fibromyalgia in adults. In: UpToDate , Post TW (Ed), UpToDate, Waltham, MA. 2022.
- Goldenberg DL. Initial treatment of fibromyalgia in adults. In: UpToDate , Post TW (Ed), UpToDate, Waltham, MA. 2022.
- Fitzcharles MA, Ste-Marie PA, Goldenberg DL, Pereira JX, Abbey S, Choinière M, Ko G, Moulin DE, Panopalis P, Proulx J, Shir Y. Canadian Pain Society and Canadian Rheumatology Association recommendations for rational care of persons with fibromyalgia: a summary report. J Rheumatol. 2013 Aug;40(8):1388-93. doi: 10.3899/jrheum.130127. Epub 2013 Jul 1. PMID: 23818709.
- Baraniuk JN. Cerebrospinal fluid levels of opioid peptides in fibromyalgia and chronic low back pain. BMC Musculoskelet Disord. 2004; 5: 1–7.
- Di Franco M, Iannuccelli C, Alessandri C, Paradiso M, Riccieri V, Libri F, Valesini G. Autonomic dysfunction and neuropeptide Y in fibromyalgia. Clin Exp Rheumatol. 2009 Sep-Oct;27(5 Suppl 56):S75-8. PMID: 20074444.
- Thieme K, Turk DC, Flor H. Comorbid depression and anxiety in fibromyalgia syndrome: relationship to somatic and psychosocial variables. Psychosom Med.2004Nov-Dec;66(6):837-44. doi: 10.1097/01.psy.0000146329.63158.40. PMID: 15564347.
- Borchers AT, Gershwin ME. Fibromyalgia: A Critical and Comprehensive Review. Clin Rev Allergy Immunol. 2015 Oct;49(2):100-51. doi: 10.1007/s12016-015-8509-4. PMID: 26445775.
- van Koulil S, van Lankveld W, Kraaimaat FW, van Helmond T, Vedder A, van Hoorn H, Donders R, de Jong AJ, Haverman JF, Korff KJ, van Riel PL, Cats HA, Evers AW. Tailored cognitive-behavioral therapy and exercise training for high-risk patients with fibromyalgia. Arthritis Care Res (Hoboken). 2010 Oct;62(10):1377-85. doi: 10.1002/acr.20268. PMID: 20521308.
- Lami MJ, Martínez MP, Sánchez AI. Systematic review of psychological treatment in fibromyalgia. Curr Pain Headache Rep. 2013 Jul;17(7):345. doi: 10.1007/s11916-013-0345-8. PMID: 23715945.
- van Koulil S, Kraaimaat FW, van Lankveld W, van Helmond T, Vedder A, van Hoorn H, Cats H, van Riel PL, Evers AW. Screening for pain-persistence and pain-avoidance patterns in fibromyalgia. Int J Behav Med. 2008;15(3):211-20. doi: 10.1080/10705500802222964. PMID: 18696315.
- von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP; STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008 Apr;61(4):344-9. doi: 10.1016/j.jclinepi.2007.11.008. PMID: 18313558.
- Garcia D, Lester N, Cloninger KM, Robert Cloninger C. Temperament and Character Inventory (TCI). In: Zeigler-Hill V., Shackelford T. (eds) Encyclopedia of Personality and Individual Differences. Springer, Cham. 2017.https://doi.org/10.1007/978-3-319-28099-8_91-1
- Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983 Jun;67(6):361-70. doi: 10.1111/j.1600-0447.1983.tb09716.x. PMID: 6880820.
- Rand Corporation. 36-Item Short Form Survey (SF-36). https://www.rand.org/health-care/surveys_tools/mos/36-item-short-form.html
- Ferrari S. he Intermed Self-Assessment questionnaire (IM-SA). https://iris.unimore.it/retrieve/handle/11380/1142963/160058/2017_IMSA_Ferrari.pdf
- Santos DM, Lage LV, Jabur EK, Kaziyama HHS, Iosifescu DV, De Lucia MCS, Fráguas R. The influence of depression on personality traits in patients with fibromyalgia: a case-control study. Clin Exp Rheumatol. 2017 May-Jun;35 Suppl 105(3):13-19. Epub 2016 Oct 20. PMID: 27782872.
- Işık-Ulusoy S. Evaluation of affective temperament and anxiety-depression levels in fibromyalgia patients: a pilot study. Braz J Psychiatry. 2019 Apr 15;41(5):428-432. doi: 10.1590/1516-4446-2018-0057. PMID: 30994852; PMCID: PMC6796816.
- Johnson P, Golden H,Katz R,Ruderman E.Convergent Validity of the SF-36 and Fibromyalgia Impact Questionnaire (FIQ) in the Measurement of Health Status in FMS Patients Arthritis & Rheumatism. 1998; 41(9):S257
- Stiefel FC, de Jonge P, Huyse FJ, Guex P, Slaets JP, Lyons JS, Spagnoli J, Vannotti M. 'INTERMED': a method to assess health service needs. II. Results on its validity and clinical use. Gen Hosp Psychiatry. 1999 Jan-Feb;21(1):49-56. doi: 10.1016/s0163-8343(98)00061-9. PMID: 10068920.
- Cloninger CR, Przybeck TR, Svrakic DM, Wetzel RD. The temperament and character inventory (TCI): A guide to its development and use. St-Louis, MO: Washington University. 1994.
- Garcia-Fontanals A, García-Blanco S, Portell M, Pujol J, Poca-Dias V, García-Fructuoso F, López-Ruiz M, Gutiérrez-Rosado T, Gomà-I-Freixanet M, Deus J. Cloninger's psychobiological model of personality and psychological distress in fibromyalgia. Int J Rheum Dis. 2016 Sep;19(9):852-63. doi: 10.1111/1756-185X.12473. Epub 2014 Dec 5. PMID: 25483854.
- Burholt V, Nash P. Short Form 36 (SF-36) Health Survey Questionnaire: normative data for Wales. J Public Health (Oxf). 2011 Dec;33(4):587-603. doi: 10.1093/pubmed/fdr006. Epub 2011 Feb 9. PMID: 21307049.
- Svrakic DM, Draganic S, Hill K, Bayon C, Przybeck TR, Cloninger CR. Temperament, character, and personality disorders: etiologic, diagnostic, treatment issues. Acta Psychiatr Scand. 2002 Sep;106(3):189-95. doi: 10.1034/j.1600-0447.2002.02196.x. PMID: 12197856.
- Gencay-Can A, Can SS. Temperament and character profile of patients with fibromyalgia. Rheumatol Int. 2012 Dec;32(12):3957-61. doi: 10.1007/s00296-011-2324-x. Epub 2011 Dec 27. PMID: 22200811.
- Arango-Dávila CA, Rincón-Hoyos HG. Depressive Disorder, Anxiety Disorder and Chronic Pain: Multiple Manifestations of a Common Clinical and Pathophysiological Core. Rev Colomb Psiquiatr (Engl Ed). 2018 Jan-Mar;47(1):46-55. English, Spanish. doi: 10.1016/j.rcp.2016.10.007. Epub 2016 Dec 14. PMID: 29428122.
- Oliveira DS, Vélia Ferreira Mendonça L, Sofia Monteiro Sampaio R, Manuel Pereira Dias de Castro-Lopes J, Ribeiro de Azevedo LF. The Impact of Anxiety and Depression on the Outcomes of Chronic Low Back Pain Multidisciplinary Pain Management-A Multicenter Prospective Cohort Study in Pain Clinics with One-Year Follow-up. Pain Med. 2019 Apr 1;20(4):736-746. doi: 10.1093/pm/pny128. PMID: 30010966.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
