Journal of Surgery and Surgical Research
A rare case of massive adult mesenteric lymphangiomatosis presenting as acute abdominal obstruction – A Case report
Ashish Vora, Department of Surgery, Dr RML Hospital & PGI, New Delhi 110001, India,
Author and article information
Cite this as
Vora A (2020) A rare case of massive adult mesenteric lymphangiomatosis presenting as acute abdominal obstruction – A Case report. J Surg Surgical Res. 2020; 6(1): 33-34. Available from: 10.17352/2455-2968.000093
Copyright License
© 2020 Vora A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.A lymphangioma usually appears as a partially septated, cystic mass on imaging studies including ultrasound, Computed Tomography (CT) and Magnetic Resonance Imaging (MRI).Lymphangioma is a rare benign tumor that develops in the lymphatic system.“Generalized lymphangiomatosis” is term given to diffuse occurance of the disease [4].This disease usually occurs in children and involves the skin.
A 45 Year old female presented to ER with complaints of pain abdomen since 8 days associated with fever, vomiting and absolute constipation since 7 days.On per abdominal examination abdomen was grossly distended with board like rigidity and rebound tenderness with absent bowel sounds.Note on percussion was tympanic.Pain started in the right lower abdomen, progressed to entire abdomen over the period of 8 days.Blood investigations showed raised TLC of 32,000 cumm and acidosis with pH of 7.0.X-ray erect abdomen standing showed multiple air-fluid levels with ground glass appearance and an USG showed multiseptated organized collection filling the peritoneal cavity with dilated bowel loops showing sluggish peristalsis.Patient was immediately admitted and after initial resuscitation with a pre-operative diagnosis of peritonitis secondary to perforation was taken to the OR.Approximately 500ml of whitish foul smelling fluid was present in the peritoneal cavity.
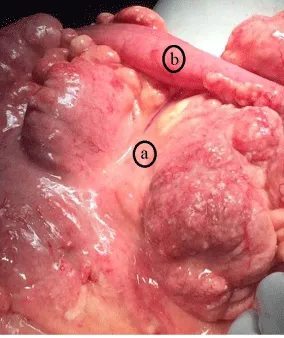
Approximately three and a half feet away from the duodeno-jejunal junction, grossly thickened lobulated mesentery encasing one feet of ileum within it was seen. It caused extra luminal obstruction (Figures 1a,b).
Grossly thickened lobulated mesentery containing multiple cysts within it which were filled with whitish fluid (Figure 2). Exploratory laparotomy was performed with resection of the encased bowel and mesentery. The resected bowel was anastomosed with through peritoneal toileting.
Histopathology report was a surprise “Cavernous lymphangioma of the mesentery and involving bowel” (Figure 3).
Post operatively patient was in ICU for one day and thereafter was shifted and discharged from ward after 8 days without any significant post-op period.
Discussion
Lymphangioma or lymphangiomatosis mostly involve the skin, the covering of various organs except brain.
More than 90% are diagnosed below age of 2 years [1,2].
In adults, gastrointestinal tract involvement of lymphangioma is very rare and the distal ileal mesentery is commonly affected [3].
They are considered to be a congenital dysplasia of lymphatic tissue and abnormal development of the lymphatic vessels during fetal life [5,6].
The macroscopic appearance of lymphangioma is a cystic mass with partial septations and its histological characteristics are endothelial-lined, dilated, communicating lymphatic channels containing a variable amount of connective tissue
Lymphangiomas can be simple capillary, cavernous, or cystic according to its anatomy [8,9].
Cavernous lymphangioma is composed of dilated lymphatic vessels and lymphoid stroma and is connected with the adjacent normal lymphatics.
Whereas cystic variety comprises of various-sized lymphatic spaces without connection with the adjacent normal lymphatics.
However, as cystic lymphangiomas may have a cavernous area, clear differentiation between cystic and cavernous lymphangioma is not always possible [9,10].
These are classified into four categories [11]: cavernous lymphangioma,capillary lymphangioma, cystic lymphangioma (hygroma) and hemolymphangioma (a combination of hemangioma and lymphangioma).
It can be limited to a particular organ or structure (e.g., spleen, liver, or thoracic cavity) or involve a more generalized process [12].
Due to absence of lymphatics in brain its spared from lymphangiomatosis.
- Vargas-Serrano B, Alegre-Bernal N, Cortina-Moreno B, Rodriguez-Romero R, Sanchez-Ortega F (1995) Abdominal cystic lymphangiomas: US and CT findings. Eur J Radiol 19: 183-187. Link: https://bit.ly/3dAkols
- Chung JH, Suh YL, Park IA, Jang JJ, Chi JG, et al. (1999) A pathologic study of abdominal lymphangiomas. J Korean Med Sci 14: 257–262. Link: https://bit.ly/2Thnaof
- Yoshida Y, Okamura T, Ezaki T, Yano K, Kodate M, et al. (1994) Lymphangioma of the oesophagus: a case report and review of the literature. Thorax 49: 1267-1268. Link: https://bit.ly/3dEaBuL
- Marom EM, Moran CA, Munden RF (2004) Generalized lymphangiomatosis. AJR Am J Roentgenol 182: 1068. Link: https://bit.ly/2WucMeF
- Paal E, Thompson LD, Heffess CS (1998) A clinicopathologic and immunohistochemical study of ten pancreatic lymphangiomas and a review of the literature. Cancer 82: 2150-2158. Link: https://bit.ly/2T1Hqd6
- Abe H, Kubota K, Noie T, Bandai Y, Makuuchi M (1997) Cystic lymphangioma of the pancreas: a case report with special reference to embryological development. Am J Gastroenterol 92: 1566-1567. Link: https://bit.ly/2yTnqT5
- Beham A (2002) Lymphangioma. In: Fletcher Ch DM, Unni KK, Merten F, editors. World Health Organization, classification of tumors. Pathology and genetics of tumors of soft tissue and bone. Lyon (France): IARC Press 162-163.
- Chen CW, Hsu SD, Lin CH, Cheng MF, Yu JC (2005) Cystic lymphangioma of the jejunal mesentery in an adult: a case report. World J Gastroenterol 11: 5084-5086. Link: https://bit.ly/35XDIX7
- Rieker RJ, Quentmeier A, Weiss C, Kretzschmar U, Amann K, et al. (2000) Cystic lymphangioma of the small-bowel mesentery: case report and a review of the literature. PatholOncol Res 6: 146-148. Link: https://bit.ly/361LiAb
- Seki H, Ueda T, Kasuya T, Kotanagi H, Tamura T (1998) Lymphangioma of the jejunum and mesentery presenting with acute abdomen in an adult. J Gastroenterol 33: 107-111. Link: https://bit.ly/3btxvDE
- Kosmidis I, Vlachou M, Koutroufinis A, Filiopoulos K (2010) Hemolymphangioma of the lower extremities in children: two case reports. J OrthopSurg Res 5: 56. Link: https://bit.ly/2zvtots
- Blei F (2011) Lymphangiomatosis: clinical overview. Lymphat Res Biol 9: 185-190. Link: https://bit.ly/2ApnbzK
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
