Journal of Surgery and Surgical Research
Thyroidectomy under local anaesthesia in a poor resource health facility in Northeastern Nigeria
1Department of Surgery, University of Maiduguri Teaching Hospital, Borno, Nigeria
2Department of Surgery, Abubakar Tafawa Balewa University Teaching Hospital, Bauchi, Nigeria
3Department of Surgery and Anaesthesia, Abubakar Tafawa –Balewa University, Bauchi, Nigeria
Author and article information
Cite this as
Aliyu S, Ningi AB, Rabi’u MB (2020) Thyroidectomy under local anaesthesia in a poor resource health facility in Northeastern Nigeria. J Surg Surgical Res. 2020; 6(1): 1-5. Available from: 10.17352/2455-2968.000084
Copyright License
© 2020 Aliyu S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: The provision of quality health care is one of the priorities of every government. The quality of such care is however, limited by the human and technical resources available. The varying types of thyroidectomy for Goitres are often done under general anaesthesia, unless, there is a contraindication such as, cardiopulmonary instability. Recently, there is increasing evidence that thyroidectomy could be done under local anaesthesia with or without anxiolytics or opioid analgesia augmentation. This study reports on our experience of performing thyroidectomy under infiltrative local anaesthesia.
Objectives: To evaluate the safety of performing thyroidectomy under infiltrative local anaesthesia and compare the post-operative outcome with that done under general anaesthesia.
Patients and methods: This is a descriptive case series of 59 patients that underwent thyroidectomy under field block with 1% Lignocaine with Adrenaline 1:200,0000 dilutions. Dose was standardised for all patients at 4mg/kg under monitored anaesthesia. The period under study covered from October 2017-October 2019. The patients’ characteristics analysed were Biodata, clinical diagnosis, patients’ weight, type of surgery, duration of surgery and complications.
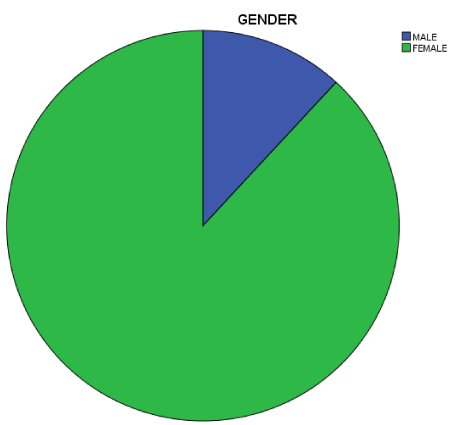
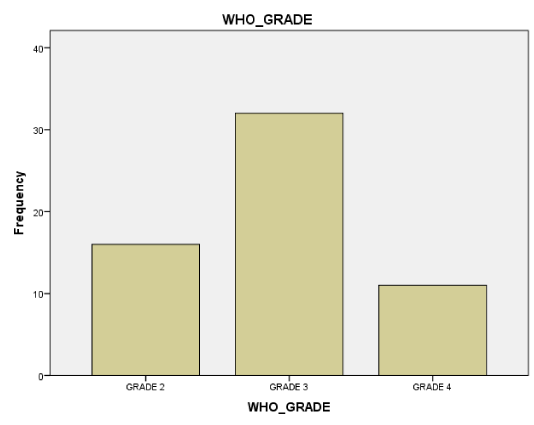
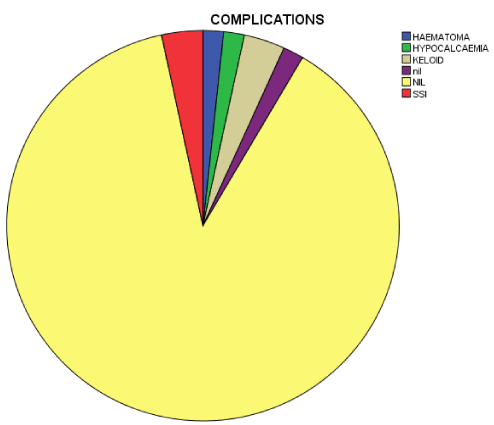
Results: The study population were 59 patients, 88.1% were females, 11.9% were males with female –male ratio of 8:1. The mean age was 42.03(+_3.5), simple multinodular goitre was the most common subtype 47.5%, toxic multinodular goitre 39%, diffuse simple goitre and diffuse toxic goitre 5.1% each. Malignant goitre 3.4% and all are papillary carcinomas. 54,2% off all the goitres are WHO grade 3. The mean duration of surgery is 40minutes and the average duration of hospital stay is 24-48hours. There were 6 complications. 1(1.7%) sub-cutaneous haematoma, 1(1.7%) post-operative hypocalcaemia, 2(3.4%) keloidal scar and 2(3.4%) surgical site infections.
Conclusion: Thyroidectomy under infiltrative local anaesthesia is safe if done by a trained surgeon, in a poor resource health facility.
Limitation: Patient’s preference for general anaesthesia and short-necked, obese patients.
The pioneers in thyroid surgeries, particularly, surgery for thyrotoxicosis, performed their surgeries under local anaesthesia [1]. The improvement in the knowledge of the pathophysiologic basis of thyroid disorders and the development of medical strategy for achieving euthyroid state allowed surgeons to perform surgery on patients with toxic goitres under general anaesthesia with adequate relaxation and minimised the incidence of thyrotoxicosis related intra-operative complications [1].
The improvement in the safety profile of general anaesthesia allowed surgeons to perform numerous procedures including thyroid surgeries almost exclusively on general anaesthesia [2]. The presence of contraindication to general anaesthesia in some patients forced surgeons to look for alternatives to general anaesthesia. In developing countries like Nigeria, most rural hospitals lack facilities for general anaesthesia and where the facilities are available, maintaining the system is usually cost inhibitive [3]. Patients with various types of thyroid pathologies stand the risk of not having their surgeries or have to travel to cities with more advanced health care system to have such operations. With out of pocket system of payment for services, inadequate NHIS coverage, payment for such care for peasant citizens is quite difficult [3].
There is therefore, a need for assessing the possibility of doing such thyroid surgeries under the relatively cheaper and more readily available infiltrative local anaesthesia. This should however be done cautiously. Patients should be meticulously assessed for medical suitability for such procedure to reduce avoidably high surgically related morbidities and mortalities.
Local anaesthesia has the added advantage of lack of general complications associated with general anaesthesia, such as nausea, vomiting and altered consciousness. The use of adrenaline containing lignocaine minimises bleeding and the need for transfusion and improves surgical field visibility. The analgesic effect continues postoperatively. This is thought to reduce the intensity of the systemic inflammatory response to the stress of surgery and ensures early post-operative recovery and probably, shorter hospital stay [4]. It will also enhance hospital economy, as thyroidectomy and other surgical procedures may be done as Day Case surgeries [4].
We, therefore, designed this study to assess the safety of thyroidectomy under local infiltrative anaesthesia and to compare its morbidity profile with thyroidectomy under general anaesthesia in carefully selected patients. We attempt to analyse patients’ characteristics and evaluate outcome measures such as hospital stay and post-operative complications and compare these with those seen in thyroidectomy under general anaesthesia. We hope to elucidate the safety of performing thyroid surgeries under infiltrative local anaesthesia and possibly allow hospitals consider doing thyroid surgeries as Day Case procures.
Patients and methods
Patients
This prospective descriptive case series was done on 59 patients between October 2017- October 2019 at the surgery department of general hospital potiskum, Yobe state, Nigeria. The hospital has a 3 operating theatre tables but, no single functional anaesthetic machine or oxygen cylinder for intra-nasal oxygenation. All the patients that were recruited were clinically assessed for symptoms of toxicity, recurrence and malignancy. All toxic goitres were chemically rendered euthyroid and all malignant goitres were clinically and radiologically assessed for loco-regional advancement. All locally advanced malignant goitres, those with failed medical control of toxicity, those with poor glycaemic control and those who declined consent were excluded. Basic preoperative haematological and biochemical parameters were ensured to be within normal range. Pre-operative indirect laryngoscopy, neck and thoracic inlet radiographs were taken to assess vocal cords integrity and to rule out tracheal abnormalities.
Detailed counselling on the procedure was done, covering the need for patients to keep communication with the operating room, swallow any accumulated saliva and to alert the team if there is undue pain or respiratory problems. Previously successfully operated patients were often involved in the counselling to demonstrate safety and allay anxiety.
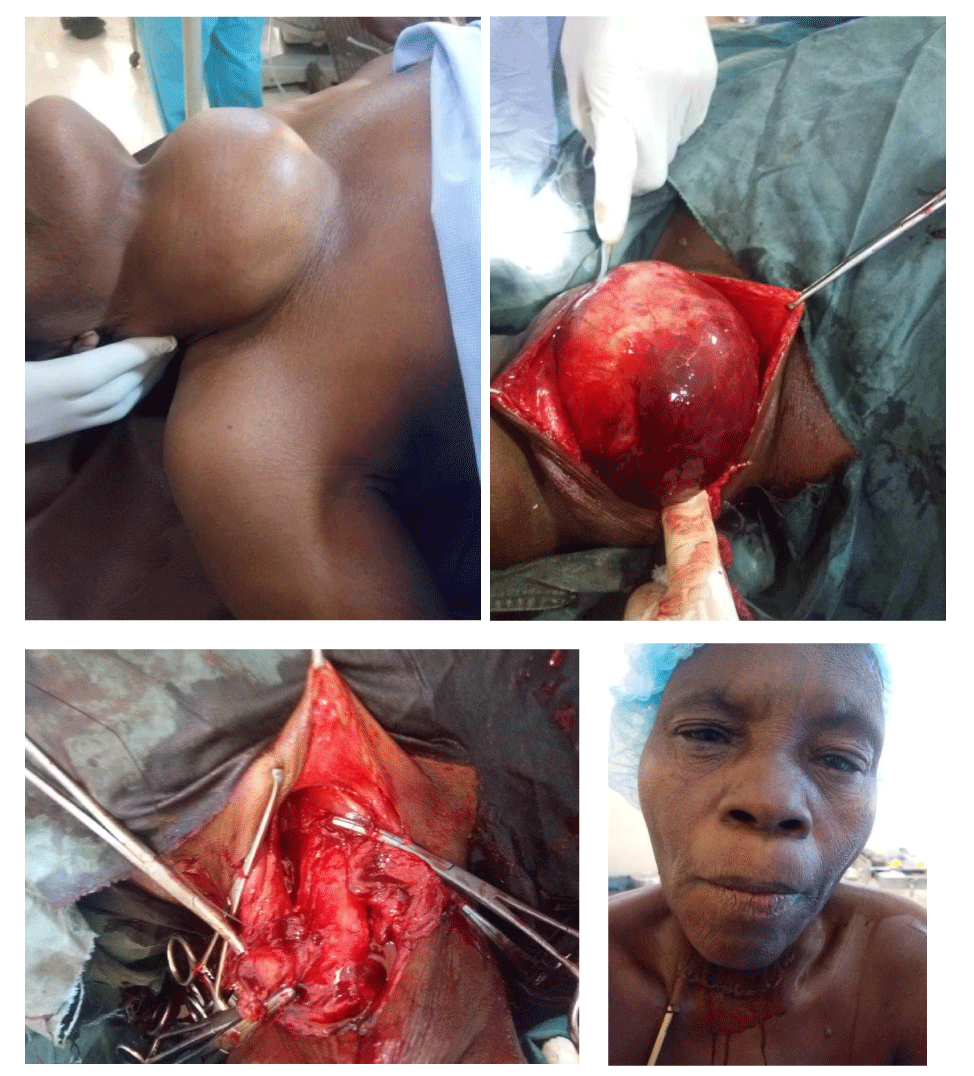
All the participants gave informed consent and additional consent was sought from few to take their pictures with the faces showing to demonstrate the state of wakefulness.
Methods
Infiltrative local anaesthesia was with 1% lignocaine with adrenaline at 1:200,000 dilutions and a standardised dose of 4mg/kg. The calculated dose was made up to 60 ml with 0.9% saline. A 10ml syringe with 27G needle was used for infiltration and the field block. 20ml of the reconstituted lignocaine was used for field block, extending from the supra-sternal notch below to the cricoid cartilage above and the lateral borders of sternomastoid muscles laterally. 10ml was given along the incision line. 10ml of lignocaine was injected under the investing layer of the pretracheal fascia after raising sub-platysma flaps. The remaining 20ml is given at 5cc at each of the thyroid poles to minimise discomfort during mobilisation.
Patients’ position and operative field preparation is as in surgery under general anaesthesia, but, draping is done in such a way to expose patient’s mouth and nose to allow continued communication and spontaneous breathing. The communication assures the surgeon of the safety of the recurrent laryngeal nerves as no effort is made to search for it. The remaining operative steps are as outlined in standard operative texts for thyroidectomy under general anaesthesia and all had a passive drain left in situ.
Only one of the patients required a salvage dose of opioid analgesia and anxiolytic due to agitation. Non was given intra-operative antibiotic as the surgery is considered to be a clean procedure. All operated patients were kept under close observation at the recovery room for 30minutes, monitored by manual assessment of their vital signs. Patients were then transferred to the surgical wards and drains were removed within 24-48hours. All were discharged home to see the team at the surgical out-patient department for wound inspection, assessment for early post-operative complications and review of results of post- operative investigations and histopathology.
Results
A total of 59 patients were recruited for the study. 52 were females and 7 were males, giving a female to male ratio of 8:1. The mean age of the study population is 42. 03, mostly between 31-40 years of age.
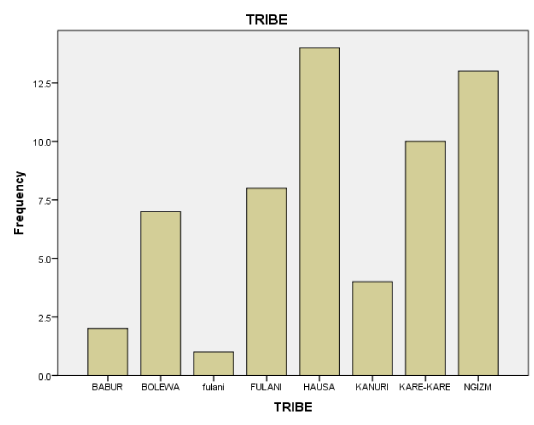
Although Potiskum is a multi-ethnic society, most thyroid pathologies are seen within Hausa (27.1%) and Ngizm (22%) population.
Most patients presented with clinically and biochemically non-toxic multinodular goitre 47.5%, toxic multinodular goitres 39%, diffuse simple goitres 5.1%, diffuse toxic goitres 5.1% and malignant goitres 3.4%. All the malignant goitres were of the papillary subtype. Majority of the patients had WHO grade 3 goitres (54.2%). 49.2% of the patients had sub-total thyroidectomy, 47.5% underwent near total thyroidectomy. Only those with malignant goitres (3.4%) were offered total thyroidectomy.
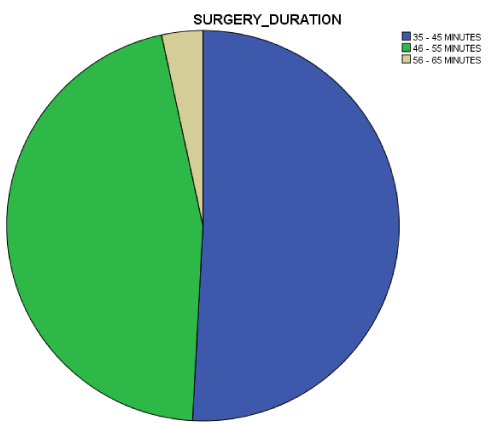
The mean operative time was 40minutes, with most surgeries finished within 35-45 minutes (50.8%). Only one of the patients required salvage dose of 30mg of pentazocine and 10mg of diazepam because of agitation. None had undue primary haemorrhage that will require volume replacement or post-operative transfusion. One patient (1.7%) had reactionary haemorrhage with subcutaneous haematoma that was drained on releasing subcuticular sutures. One patient (1.7%) developed hypocalcaemic tetany which resolved on administration of 10% calcium gluconate and maintenance dose of oral calcium preparation. Two patients (3.4%) developed superficial incisional surgical site infection and 2 others (3.4%) developed keloidal scars within 6 months of follow up visits.
None of the patients had respiratory problems post-operatively and all had their passive drains removed within 24-48 hours. None has reported delayed onset of voice changes, recurrent toxic symptoms or clinical symptoms of hypothyroidism.
Majority of the patients were discharge 24 hours after surgery. 24 hours (49.2%), 24-48hours (37.3%) and 13.6% remained beyond 48hours (Figures 1-6) (Tables 1-3).
Discussion
Undertaking thyroidectomy under regional anaesthesia is not novel in the Nigeria or other African countries. Alufohai E, reported his experience with thyroidectomy for various thyroid pathologies and reported the use of augmented local anaesthesia for thyroidectomy in poor resource rural hospital [3]. The augmentation was mainly with sedatives/ anxiolytics and the Wilson sedation score is often 1-2 [5].
Many Authors have reported performing thyroidectomy under local anaesthesia without any augmentation and they didn’t find any statistically significant difference in safety when compared with those done under general anaesthesia [6].
There were initial concerns on the safety and challenges associated with use of local anaesthesia for thyroidectomy. The possibility of failure and the need for conversion to general anaesthesia appear cogent and the consequence could be fatal if the needed requirements for the general anaesthesia are unavailable. Careful selection of patients is therefore paramount. The potential risk of intravascular injection and subsequent cardiac or neurological complications like seizure were raised [7]. The untoward systemic effect however, will be dependent on the total administered dose, rate of vascular absorption, plasma concentration, bioavailability, pharmacokinetics and the efficacy of the body’s metabolic and excretory functions [8].
Local anaesthesia obviates the risks that are inherent in general anaesthetic agents, risk of laryngeal spasm or oedema on endotracheal intubation and the increased need for post-operative continued monitoring or even ICU admission [9].
The preponderance of female patients in our study, with a male-female ratio of 1:8 is in keeping with reports from other workers [1]. Although, almost half of our patients presented with large goitres, this didn’t pose any challenge. Previous works have alluded to this observation also [3].
Majority of the benign goitres were treated with sub-total thyroidectomy except for those in the males and the elderly. We preferred near total thyroidectomy for the males because of the documented increased risk of malignant transformation in their goitres. Elderly patients with benign multinodular goitre were also treated by near total thyroidectomy. This is because of the reported risk of malignant transformation in the remaining thyroid tissue. Although, there is a shift towards total thyroidectomy for even multinodular goitres because of the above noted reason [10], we preferred conserving some thyroid tissues in our patient. L-thyroxine replacement therapy following total thyroidectomy is often difficult in rural patients, as availability and affordability of the drug is often problematic.
No statistically significant difference has been noted in the complication rates for thyroidectomy under local anaesthesia when compared with those done under general anaesthesia [10]. None of our patients suffered recurrent laryngeal nerve injury. The continuous communication intraoperatively and the avoidance of search for the nerve have been attributed to such [10].
One patient each, developed hypocalcaemia and subcutaneous haematoma. This was from the total thyroidectomy group. Bhattacharya reported similar complication rate [11]. Two patients developed superficial incisional surgical site infection. This is similar to the infection rate reported for thyroidectomy under general anaesthesia [12,13].
87% of our patients were discharged home within 2 days of surgery. The decreased stay is related to decreased physiological changes associated with local anaesthesia, early recovery and the absence of life threatening complications in our patients.
It is evident from this study that thyroidectomy under local anaesthesia can be safely done by a trained surgeon in a carefully selected cohort of patients. Surgeons practicing in the secondary tier health facilities can safely offer surgery to the retinue of their patients with thyroid disorders and those in tertiary health facilities can convert thyroidectomy to a day care procedure.
- Crile G (1989) Regional anaesthesia for certain patients undergoing thyroid and parathyroid surgery. Surgery 105: 455. Link: http://bit.ly/2RktgDA
- Lo Gerfo P, Ditkoff BA, Chabor J, Feind C (1994) Thyroid surgery using monitored anaesthesia care: an alternative to general anaesthesia. Thyroid 4: 437-439. Link: http://bit.ly/2RnaFXG
- Misauno MA, Yilkudi MG, Akwaras AL, Embu HY, Ojo EO, et al. (2008) Thyroidectomy under local anaesthesia: how safe? N J of Clinical Practice 11: 37-40. Link: http://bit.ly/2uw3jbm
- Hochman MD, Willard FE (1991) Thyroidectomy under local anaesthesia. Arch Otolaryngol Head Neck Surg 117: 405-407.
- Prasad KC, Shanmugam VU (1998) Major neck surgeries under regional anaesthesia. Am J Otolaryngology 19:163-169. Link: http://bit.ly/2NWcgRV
- Fernandez FH (1984) Cervical block anaesthesia in thyroidectomy. Int Surg 69: 309-311. Link: http://bit.ly/30Mhsgw
- Lo Gerfo P (1998) Local/regional anaesthesia for thyroidectomy: Evaluation as an outpatient procedure. Surgery 124: 975-979. Link: http://bit.ly/36ik9aB
- Lo Gerfo P (1998) Outpatient thyroid surgery. J Clin Endocrinol Metab 83: 1097-1100. Link: http://bit.ly/2NWSyFH
- Michelle CS, Miriam R, Catherine BB, Esposito C, Fahey TJ (2001) Characteristics of Patients Having Thyroid Surgery under Regional Anaesthesia. J Am CollSurg 193: 367-372. Link: http://bit.ly/2usANam
- Ignjatović M, Cuk V, Ozegović A, Cerović S, Kostić Z (2003) Early complications in surgical treatment of thyroid diseases: analysis of 2100 paticnts. Acta Chir lugosI 50: 155-175. Link: http://bit.ly/2kpatJB
- Bhattacharyya N, Fried MP (2002) Assessment of the morbidity and complications of total thyroidectomy. Arch Otolaryngol Head Neck Surg 128: 389-392. Link: http://bit.ly/2NVhP2Y
- Hisham AN, Aina EN (2002) A reappraisal of thyroid surgery under local anaesthesia: back to thefuture? ANZ J Surg 72: 287-289. Link: http://bit.ly/36o7mDN
- Saxe AW, Brown E, Hamburger SW (1988) Thyroid and parathyroid surgery performed with patient under regional anaesthesia. Surgery 103: 415-420. Link: http://bit.ly/30PwMZD
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
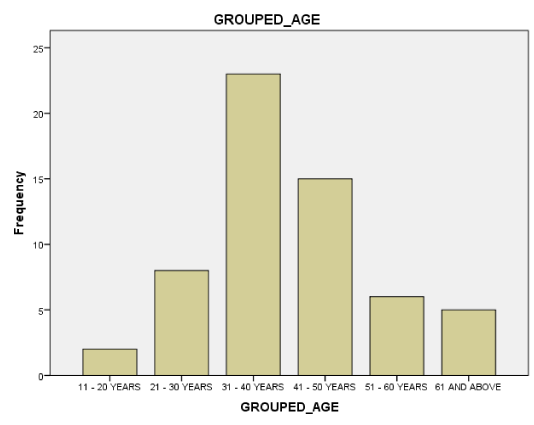


 Save to Mendeley
Save to Mendeley
