Journal of Surgery and Surgical Research
Complications of Hydatid Cysts in the Lung
1Department of thoracic surgery, Medical Faculty, Doctor of medicine, Associate Professor, University of Yuzuncu Yil, Van, Turkey
2Department of pulmonology, Medical Faculty, Doctor of medicine, Assistant Professor, University of Yuzuncu Yil, Van, Turkey
Author and article information
Cite this as
Cobanoglu U, Asker S (2015) Complications of Hydatid Cysts in the Lung. J Surg Surgical Res. 2015; 1(2): 23-28. Available from: 10.17352/2455-2968.000006
Copyright License
© 2015 Cobanoglu U, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.A hydatid cyst, or echinococcus, is a zoonosis frequently formed by the larvas of Echinococcus granulosus. The disease appears as a slowly growing cystic mass and is asymptomatic. The disease is common in the Eastern, Southeastern, and Central Anatolia regions of Turkey. The rate of incidence of the disease in Turkey is reported as 5.7 out of 100,000 individuals. The complications of hydatic cysts appear as different clinical entities depending on the cyst’s being intact or ruptured. The complications of intact cysts are usually compression symptoms, while the infection in the clinical progress of the ruptured cysts and secondary complications to the infecion are frequently seen. In this section, hydatid cyst complications in the lung, extrapulmonary thoracic findings, and respiratory system complications of hydatid cyst cases of the liver will be discussed.
Echinococcus is one of the common infections around the world caused by adult parasites of the Echinococcus species in the final hosts and the larva with metacestode form in the interval hosts. Infections in the final hosts are called echinococcus while the infection caused by the larva in interval host is called echinococcus, hydatid cyst disease, hydatidosis, cystic echinococcus, alveolar echinococcus, and polycystic echinococcus [1].
Hydatid cyst disease, which is common throughout the world, remains a serious health problem in developing countries and in the countries where stock-breeding is common [2].
It adheres to the intestinal wall with the embryo caranoids from the eggs taken orally and reaches the liver, first entering the blood vessels there. Therefore, the organ where the disease is seen at the most frequent rate is the liver, at a rate of 60-70%. 20 to 25% of the patients have lung involvement and 10% have any organ involvement. When the parasite settles on an organ, hydatid cysts occurs [3].
There are 4 means through which the parasite can reach the lung: 1–The parasite dies, there is a loss of liquid, and the cuticula get fibrosis; 2-The cysts is expectored through bronchial drainage; 3. The infection between the cyst and cuticula leads to cystic death and infection appears in the space; and 4. The cysts continue growing depending on the resistance of lung surrounding [4].
Cysts hydatic can present with many different clinical findings since it may have various organ involvements and also due to the complications that may develop. The objective of this paper is to review the complications that may occur during the progress of the hydatid cysts in the lung and the clinical findings that develop in line with these complications.
Additionally, extrapulmonary intrathoracic hydatid cyst cases and the respiratory system complications developed based on the hydatid cysts in the liver will be discussed in this section.
The complications of hydatid cysts in the lung can be generally discussed under nine headings.
Complications of Intact Cysts
The early period of the formation of a cyst is generally asymptomatic and they do not exhibit any symptoms until they reach nearly 5 cm in diameter [3]. The cysts without symptoms are generally detected during regular treatments [3].
The symptoms appear with pressure on the adjacent organs and the development of complications. Hydatid cysts can reach to large dimensions (≥10cm) without symptoms in the pediatric age groups since their immune response has not yet fully developed; furthermore, the parenchyma elasticity of the lung and the respiratory capacity is greater compared to adults [5]. Such cysts generally lead to chest pain and coughing, depending on bronchial and/or pleural irritation and to dyspnea, depending on the pressure on the parenchyma [5].
Larger cysts may lead to the symptoms due to pressure on the adjacent vital organs, such as the esophagus, heart, trachea, and large veins and may cause mediastinal shift, cardiac malposition and arrhythmia, pressure on the main vascular structures, and Vena Cava Superior Syndrome [6].
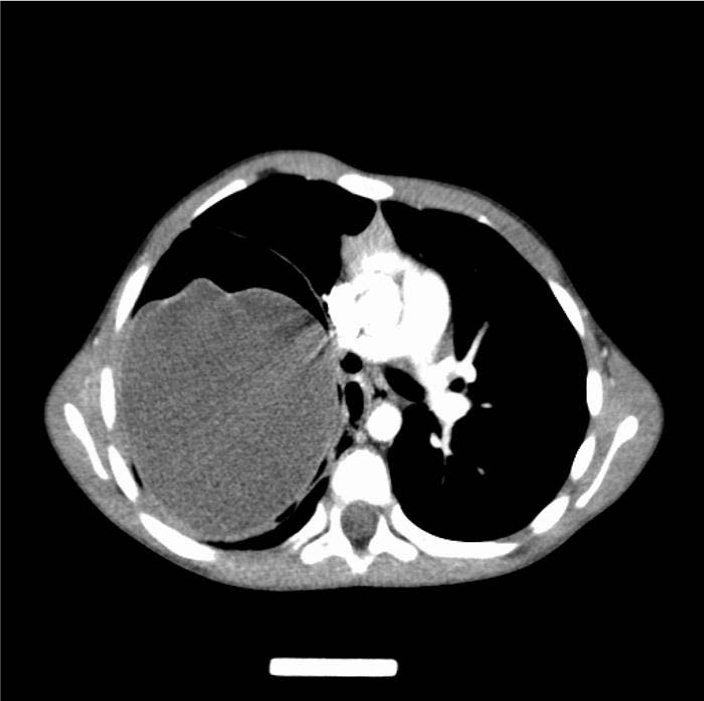
In our multi-centered study in which we examined hydatid cyst cases with 412 cases between 2003 and 2011, giant hydatid cyst was detected in 46 cases (11.1%) and mediastinal shift and the clinical findings depending on this were detected in 9.75% of the cases [7].
After the diognosis, the patients were scheduled for urgent surgery (Figure 1).
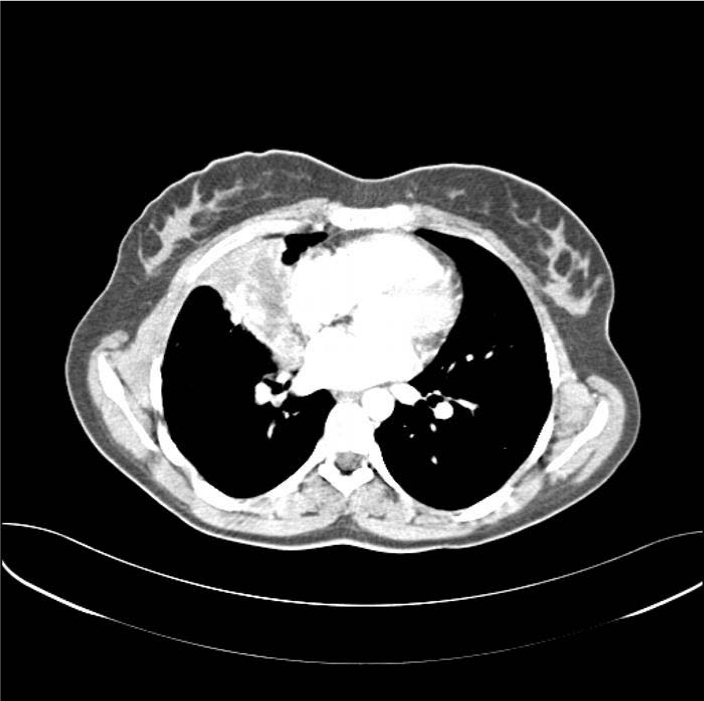
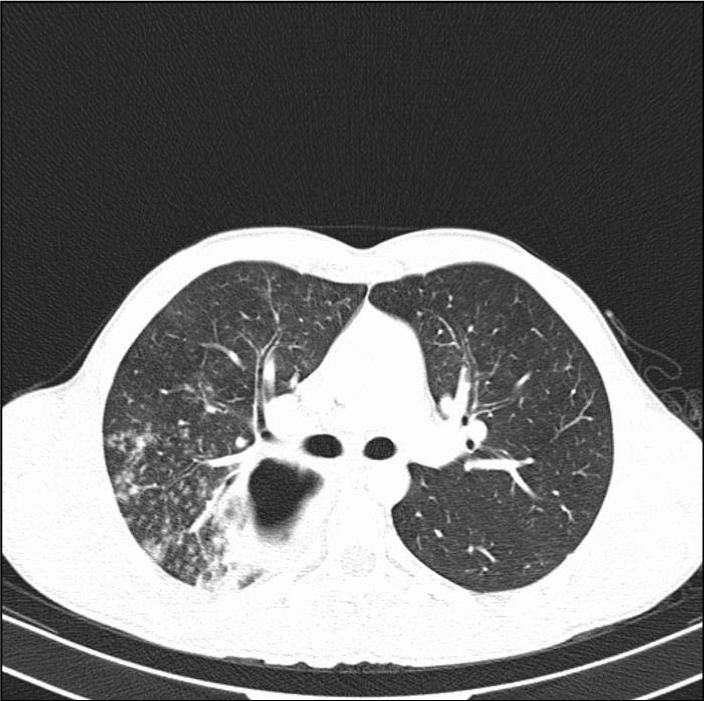
Atelectasis caused by compression of the cyst and pneumonia as a result of atelectasis are the common complications in cases of intact cysts [6,8]. In intact cysts, pneumonia developing from atelectasis is formed as a result of the erosion of the bronchus by the cysts, cyst rupture, or more rarely, erosion occurring in the vascular structure [6,8]. The cysts in the lungs were reported to cause massive hemoptysis and subsequent mortality when they are closely adjacent to large vascular structures and the vascular wall is eroded [8]. In our multi-centered study it was detected that atelectasis depending on hydatid cyst pressure developed in 16.26% of the cases (11.6% of these cases are with giant hydatid cyst) and the respiratory problems increased [7]. In the same study [7], the presence of pneumonia was detected during the diagnosis in 3.39% of the cases. However, in another of our studies where diagnosis dilemma in cystic hydatic cases was examined [9], it was determined that 27.27% of the cases were tracked with lobar pneumonia and following the treatments, the presence of a hydatic cyst was detected (Figure 2).
Since the fibrosed lung parenchyma forms the pericyste tissue around the growing hydatid cyst, parenchymal loss is in direct proportion to the size of the cyst [6]. Bronchiectasis in the distal parenchyma as a result of bronchial obstruction and a destroyed lung are the other frequently seen complications. If the parenchymal destruction is considered to be irrevocable in such cases, resection must be preferred [6,10]. In the current study, the destruction areas of which the borders exist and do not exist in the anatomic localization, in the peripheral parenchymal tissue in many cases with hydatid cyst were detected while destroyed lung covering the entire lung was not detected in any case. In three cases related to hydatid cyst (0.72%), it was detected that the bronchiectasis developed and anatomic resections were conducted on these cases [7].
Complications Related to Hydatid Cyst Rupture
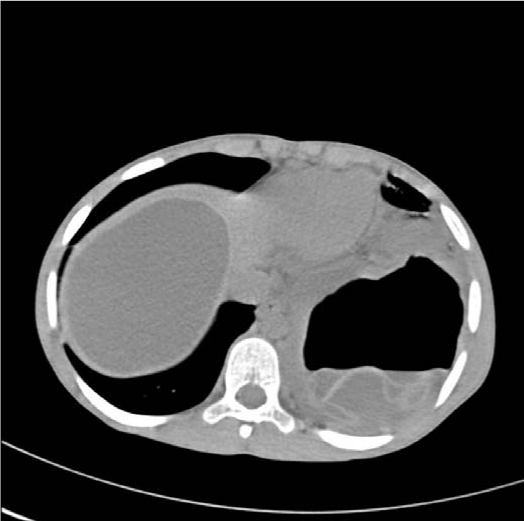
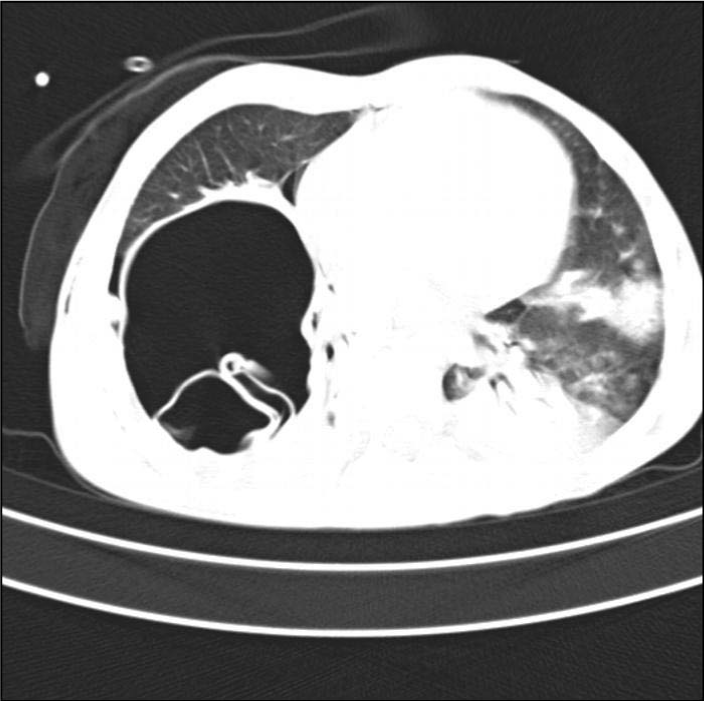
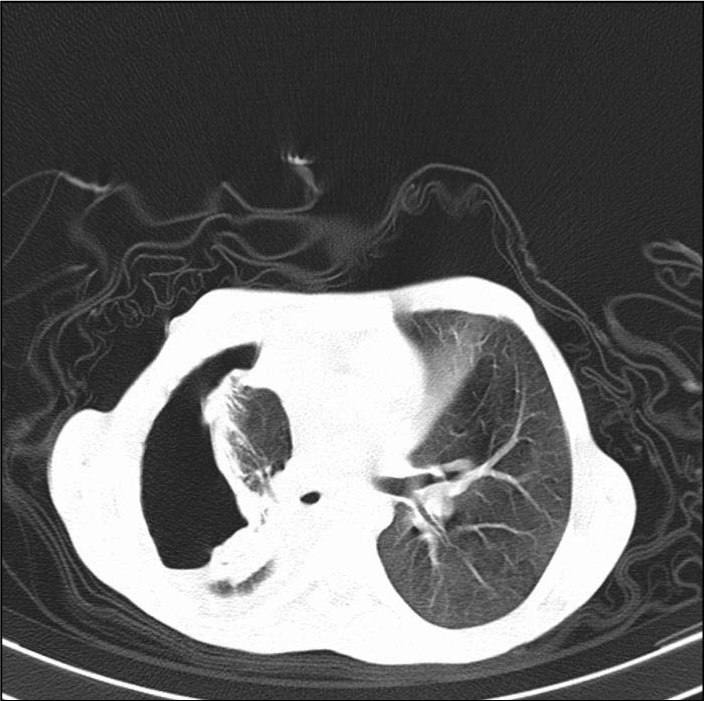
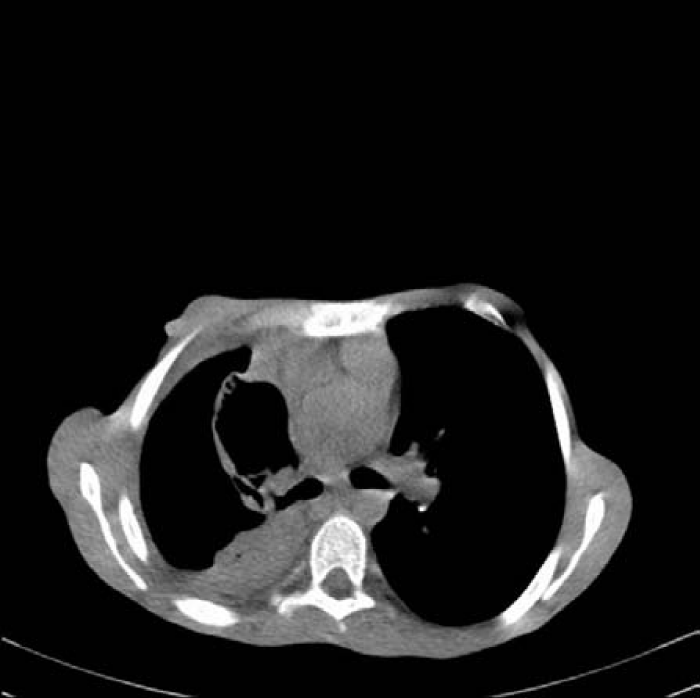
Hydatid cysts may be ruptured to the bronchial system at any period of the life cycle, whether spontaneous iatrogenic, or traumatic [11]. Perforation rates in lung hydatid cysts may vary between 26.7-49% in different series [6,11]. In our studies, the perforation rate was high (42.7%) because of late consultation with a doctor due to the socio-economic and cultural structure of the region [7,12] (Figures 3, 4).
Since the pericyste in the lung does not develops well as in the liver, it is more likely to rupture. An increase in the size of the cyst, which causes an increase in intrathoracic pressure, due to factors such as trauma and cough, can cause the cyst rupture [11]. The pressure inside the cyst is proportional to the cube of the diameter of the cyst. Therefore, even the smallest increase in diameter of the cyst increases cyst pressure to a serious degree and causes a large rupture risk.
The complications in ruptured hydatid cysts are seen more frequently compared to intact cycts hydatics [8]. Complications of a ruptured cyst of can be ordered as: asphyxia (membrane and cyst fluid expectoration), hemoptysis, anaphylactic shock, respiratory failure, pneumonia, destroyed liver, bronchiectasis, pulmonary abscesses, empyema, pneumothorax, and aspergilloma in the cyst cavity (Figure 5). Additionally, a perforated hydatid cyst can cause extrapulmonary destruction in the sternum and ribs.
In particular, large ruptured cysts can result in asphyxia of cyst fluid or membrane fragments that fill the tracheobronchial system and result in sudden death [8].
In the current study, although 10.79% of the 176 cases of perforated hydatid cysts had cyst membrane expectoration,but none of them had asphyxia clinical course [12].
Hemoptysis is a complication frequently observed as a result of the rupture of intraparenchymal cysts. It is reported at a rate of 1.8-8% in different series [8]. In our two different studies, hemoptysis was detected in 42.7% cases and only 6 of them (1.45%) had massive hemoptysis [7,12].
Rupture is a predisposing factor for infection, which is the most serious complication. The frequency of this complication is reported between 30-90%. Infected hydatid cysts can show a thick and opacifying wall structure, similar to lung abscesses, and include air-liquid level and a pneumonic consolidation area can surround them [13]. When the cyst cavity is involved in the bronchial system, this prepares the environment for bacterial and fungal infections. The pneumonia in the peripheral parenchyma after an infection of the cyst cavity, bronchiectasis in the delayed cases and a destroyed lung are the pathologies encountered [8,10],[11]. In the case that the cyct is infected, immune complex disease, glomerulonephritis, nephrotic syndrome, and secondary amyloidosis can develop [13].
In the current study, which included cases with perforated hydatid cyst, an infection clinical course consisting of lung abscesses, empyema, and pneumonia were detected in 40.9% of the cases [12].
Respiratory failure is a rare complication of hydatid cysts. The large cysts that depend on invasive parenchymal involvement caused by Echinococcus multilocularis or Echinococcus granulosus and may lead to respiratory failure [14] (Figure 6).
If the cyst leaks without a serious rupture, recurrent urticaria or bronchospasm may develop as a symptom of hypersensitivity [14]. If the cyst ruptures and antigenic material spreads, this may lead to sudden and delayed reactions, and provoke allergies, eosinophilic pneumonia, and even anaphylaxis.
Pleural complications
Pleural involvement in hydatid disease is formed primarily with the hematogen or lymphatic route and direct larval infestation of the pleura or secondarily with the spread of cyst content throughout the pleura as a result of a rupture of an adjacent pulmonary or hepatic cyst [15].
Parenchymal hydatid cysts, ruptured or intact, can progress particularly with pleural effusion and with complications such as empyema, pneumothorax. On average 5-13% of the hydatid cyst patients may develop complications such as pleural effusion, pneumothorax, hydropneumothorax, tension pneumothorax, empyema, bronchopleural fistula, pleural thickening, trapped lung, and secondary pleural hydatic disease [6,8],[15].
Pleural effusion formed in intact cysts frequently develops as parapneumonic effusion and liquid exudate [6] (Figure 7).
If there is no pleural adhesion in the rupture to pleura, the rupture will result in pneumothorax or a hydropneumothorax and in such cases, generally there are small bronchial fistula that are not large enough to discharge the content of the cyst.
If there is pleural adhesion, following to pachypleuritis, pleural thickening will occur and the pleura will be cultured [16]. As a result that the live scolex that is released from the ruptured pulmonary hidatic cyst is cultivated to the cavity, secondary pleural hydatic disease occurs [16].
In our series of 412 cases where surgical procedures were examined and in our series of 176 cases where the complications related to perforated hydatid cysts, the rate of pleural complication was 26.94% [7,12]. 22.77% of 176 cases with perforated hydatid cyst were detected to have pneumothorax. Two of these (1.13%) were tension pneumothorax. Pleural effusion in 36 (20.45%) cases, empyema in 35 (19.88%) cases, and pleural thickening in 17 (9.65%) cases were detected [12].
Cardiac complications
The cysts in the cardiac area are seen at a rate of 0.02-2% [15,17]. Since the vascular ground is richer, it is seen in the left ventricular wall most frequently, and may be seen in the right ventricule and other locations around the heart. The accession of Echinococcus embryo to the left chamber of the heart occurs through coronary circulation and to the right chamber through venous return [16]. There are two potential mechanisms through which the embryo can access the coronary circulation.
Transmission is realized through patent foramen ovale or pulmonary circulation, with the skolexes passing from hepatic system to the right atrium or to the pulmonary veins through tears in the lung cyst [18].
The embryo reaches full maturity within one to five years after it reaches the heart. In the cyst, adventitial perycyst layer occurs as myocardial reaction [18]. The cysts in the right chamber of the heart tend to grow as intracavitary and subendocardial, the left heart cysts tend to grow subepicardial.
The complications are reported to be associated with the cardiac cysts: rupture, pulmonary and systemic embolism, heart block, cardiac valve obstruction, congestive heart failure, pericarditis, cardiac tamponade, acute myocardial infarction, anaphylaxis, and pulmonary hypertension [6,18].
In cardiac hydatid cysts with an interventricular septum location, atrioventricular block, syncope attacks, and apnea may develop depending on compression in the cardiac nerve conduction paths [19]. The cysts in the right ventricule are ruptured more frequently and they may lead to pulmonary embolism, anaphylaxis, and sudden death. As a result of rupture to the pericardial cavity, effusion, and cardiac tamponade may develop. The heart can be affected secondarily with direct contact with hepatic and pulmonary cysts.
Although it is rare, the complications such as pulmonary artery stenosis and compression have been reported for the cysts with central location [20]. The cysts that create pressure on coronary arteries may lead to myocardial infarction [15,17].
Mediastinal complications
Mediastinal hydatid cyst is seen at a rate of 0.1% as primer [21]. This parasite may reach the mediastinal region through a branch of the thoracic aorta or lymph nodes [21]. Many mediastinal cysts settle on the paravertebral sulcus. It is rare that cysts with a paravertebral location may expand to the spinal duct. These cysts, which are called pince-nez cysts in the literature, form when the cyst with a paravertebral location reaches the opposite paravertebral area through the front of the vertebra from the back of the aorta and esophagus [21]. The visceral mediastinum is a rare localization for hydatid cysts.
Mediastinal hydatid cysts may be solitary or multiple. Symptoms and the complications depend on the size, localization of the cyst, and involvement of the peripheral structures [13]. Furthermore, they erode some main vascular structures, and pressure and associated complications may be seen. Mediastinal cysts frequently lead to the compression of mediastinal shift, cardiac and main vascular structures and also rarely lead to Horner’s syndrome, thoracic outlet syndrome, diaphragmatic eventrations as a result of phrenic nerve failure, respiratory disorder after tracheal compression, and failure to thrive due to esophagus pressure [21].
In the current study, there were six (1.45%) hydatid cyst cases that were all intact, consisting of two (0.48%) visceral, and four (0.97%) settled in the posterior mediastium. The cysts located in the visceral mediastinum had small diameters and in the two cases with posterior mediastinum locations, there was esophagus pressure [7].
Thorax wall complications
Hydatid cyst cases with chest wall locations are very rarely observed. The focus may be soft tissue, sternum or rib in the involvement of chest wall. Bone involvement in all hydatid cysts are seen between 0.9% and 2% [22].
Hydatic disease in the chest wall muscular structure occurs at a rate of 0.5-1% of all Echinococcus infections and generally occurs with propagation during surgery of the lesion in the liver and lungs [22].
Infection is generally removed during childhood; however, since the incubation time is longer than ten years, clinical appearance may be delayed until adulthood [22]. Direct implementation of the embryo through an infected dog bite and spread to the systemic circulation from the bowels and then passing through two important strainers (the liver and lung) and reaching to the muscle are the thoughts set forth in the related pathogenesis regarding primer skeleton muscle of hydatid cyst localization [22]. Hydatid cysts located in the thoracic wall may lead to muscle and bone destruction [6]. Pathological changes caused by the hydatid cyst made to the thoracic wall radiologically imitate tumors of the thoracic wall [6].
In our clinic, a 31-year-old female patient was diagnosed with hydatid cyst with the size of 15x23 cm in the left posterolateral hemithorax, latissimus dorsi muscle [23]. In a case without infected dog bite story and hydatid cyst in the lung and liver, it was concluded that the cyst settled in the skeletal muscles, accessing the circulatory system through the bowels.
Settlement in the thoracic aperture and complications
The most frequent complications of the cysts that settle in the thoracic aperture are Vena Cava Superior syndrome and Horner’s Syndrome, hoarseness after the Laryngeal nerve is invaded, Thoracic Outlet Syndrome, Subclavian artery pressure [6,24].
Respiratory system complications of the hydatid cysts in the liver
Hydatid cysts frequently settle in the right lobe of the liver and are generally solitary. They can lead to hydatid cysts in the lung or bronchobiliary fistula by accessing the bronchial tree through transdiaphragmatic transmission. Dome cysts in the liver that have become excessively large erode the diaphragm muscles and perforate the thorax.
The complications with diaphragmatic involvement of the liver cysts and intrathoracic propagation are reported at a rate of 0.6-16% [25]. These complications, many of which are seen in the cysts located in the liver dome can generally originate from factors including spontaneous, traumatic, and intraabdominal pressure increases. The pressure gradient between the thorax and abdomen cavity, diaphragmatic ischemia secondary to compression, inflammation in the cyst membrane, and the chemical effect of the gallbladder on the diaphragm are the other predisposing factors [25].
If the liver dome cysts become a perforated thorax, they may lead to pleural effusion, empyema, or parenchymal destruction. The opening of the liver hydatid cyst to the pleural cavity or bronchus is the cause of high mortality (9-43%) and morbidity [26]. In our series of 27 cases in which we examined liver dome cysts together with the lung, it was determined that 11 (40.74%) cysts in the lung were perforated and all the cysts in the liver were intact. All of these cases were operated on with thoracophrenotomy [27].
When the cyst crosses the diaphragm, it may rupture in the pleural cavity, intrathoracic large veins, pericardium, and the pulmonary parenchyma if there is adhesion between the diaphragm and lungs [25,26]. The gallbladder has a corrosive effect on the lungs and pleural area. An indication of the presence of gallbladder in the pleural liquid and with the analysis of biloptysis and bilirubin levels is pathognomonic for the fistula [25,26]. In the bronchobiliary fistula where the mortality is already high, the surgical treatment must be considered only when no response is given with conservative approaches [26].
Systemic complications
In the hydatid cyst cases, anaphylaxis and shock are life threatening complications that can be seen after cyst perforation [28].
When the cyst leaks without serious rupture, recurrent urticarial or bronchospasm may appear as a symptom of hypersensitivity. This situation that the allergic proteins caused in the cyst may create a simple allergic reaction in a short time during which the symptoms such as chest pain, itching, urticarial, flushing appear and also may lead to shock status [28].
In our series in which we examined perforated hydatid cysts, allergic complications were detected in 14 cases (7.95%), urticaria and erythema in six (3.40%) cases, and asthma and bronchial provocation in three (1.70%) cases were identified [12].
When the cyst ruptures, results ranging from anaphylactic shock to death may appear [28]. After the intraoperative cyst is drained into the bronchial system or pour into the blood circulation for a patient with stable progress under general anesthesia, if low blood pressure or shock are observed, within minutes the reaction must be suspected [28].
Anaphylaxis is an unwanted hypersensitivity reaction of which the clinic status may be very serious. This may result in death due to vascular collapse and obstruction of the airway [29].
It should be kept in mind that allergic reactions may be observed, depending on the cyst rupture after anthelmintic hydatid cyst treatment or percutaneous aspiration [28]. In the liver hydatid cyst, allergic reactions depending on spontaneous cyst rupture are reported but the case of lung hydatid cyst that appears with anaphylaxis is very rare [28].
Conclusion
Under the conditions in Turkey, not only the doctors of general surgery or thoracic surgery, but also the doctors from almost all branches encounter hydatid cysts once in their careers. Hydatid cysts present with many different clinical findings because of the potential of the involvement of various organs and the complications that may develop. Complicated hydatid cysts may clinically imitate many diseases and radio logically, the problems may occur in the diagnosis, long hospitalization time, and high hospital costs may appear. Therefore, the complications that may develop during the progression of hydatid cyst and the clinical findings depending on these complications must be known.
- Mallon DH, Summers DM, Bradley JA, Pettigrew GJ (2013) Defining delayed graft function after renal transplantation: simplest is best. Transplantation 96: 885-889 .
- Kayler L, Zendejas I, Molmenti E, Chordia P, Schain D, et al. (2012) Kidney transplant ureteroneocystostomy: comparison of full-thickness vs. Lich-Gregoir techniques. Clinical transplantation 26: E372-380 .
- Pascual J, Zamora J, Pirsch JD (2008) A systematic review of kidney transplantation from expanded criteria donors. American journal of kidney diseases : the official journal of the National Kidney Foundation 52: 553-586 .
- Johnson LB, Kno PC, Dafoe DC, Schweitzer EJ, Alfrey EJ, et al. (1996) Double adult renal allografts: a technique for expansion of the cadaveric kidney donor pool. Surgery 120: 580-583 .
- Moore PS, Farney AC, Sundberg AK, Rohr MS, Hartmann EL, et al. (2006)Experience with dual kidney transplants from donors at the extremes of age. Surgery 140: 597-605 .
- Laftavi MR, Stephan R, Feng L, Said M, Kohli R, et al. (2011) Dual kidney transplants from very old or very young donors: long-term outcomes and complications. Transplantation proceedings 43: 507-511 .
- Lu AD, Carter JT, Weinstein RJ, Prapong W, Salvatierra O, et al. (1999) Excellent outcome in recipients of dual kidney transplants: a report of the first 50 dual kidney transplants at Stanford University. Archives of surgery.134: 971-975 .
- Medina-Polo J, Pamplona-Casamayor M, Miranda-Utrera N, Gonzalez-Monte E, Passas-Martinez JB, et al. (2014) Dual kidney transplantation involving organs from expanded criteria donors: a review of our series and an update on current indications. Transplantation proceedings 46: 3412-3415 .
- Remuzzi G, Cravedi P, Perna A, Dimitrov BD, Turturro M, et al. (2006) Long-term outcome of renal transplantation from older donors. The New Eng J Med 354: 343-352 .
- Hobart MG, Modlin CS, Kapoor A, Boparai N, Mastroianni B, et al. (1998) Transplantation of pediatric en bloc cadaver kidneys into adult recipients. Transplantation 66: 1689-1694 .
- Dalgic A, Boyvat F, Karakayali H, Moray G, Emiroglu R, et al. (2006) Urologic complications in 1523 renal transplantations: The Baskent University experience. Transplantation proceedings 38: 543-547 .
- Faenza A, Nardo B, Catena F, Scolari MP, d'Arcangelo GL, et al. (1999) Ureteral stenosis after kidney transplantation. A study on 869 consecutive transplants. Transpl Int 12: 334-340 .
- Faenza A, Nardo B, Fuga G, Liviano-D'Arcangelo G, Grammatico F, et al. (2005) Urological complications in kidney transplantation: ureterocystostomy versus uretero-ureterostomy. Transplantation proceedings 37: 2518-2520 .
- Gill J, Cho YW, Danovitch GM, Wilkinson A, Lipshutz G, et al. (2008) Outcomes of dual adult kidney transplants in the United States: an analysis of the OPTN/UNOS database. Transplantation 85: 62-68 .
- Lucarelli G, Bettocchi C, Battaglia M, Impedovo SV, Vavallo A, et al. (2010) Extended criteria donor kidney transplantation: comparative outcome analysis between single versus double kidney transplantation at 5 years. Transplantation proceedings 42: 1104-1107.
- Rigotti P, Capovilla G, Di Bella C, Silvestre C, Donato P, et al. (2014) A single-center experience with 200 dual kidney transplantations. Clinical transplantation 28: 1433-1440 .
- Kayler LK, Srinivas TR, Schold JD (2011) Influence of CIT-induced DGF on kidney transplant outcomes. Am J Transplant 11: 2657-2664.
- Quiroga I, McShane P, Koo DD, Gray D, Friend PJ, et al. (2006) Major effects of delayed graft function and cold ischaemia time on renal allograft survival. Nephrol Dial Transplant 21: 1689-1696 .
- Ekser B, Furian L, Broggiato A, Silvestre C, Pierobon ES, et al. (2010) Technical aspects of unilateral dual kidney transplantation from expanded criteria donors: experience of 100 patients. Am J Transplant 10: 2000-2007 .
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
