Journal of Clinical Research and Ophthalmology
Penetrating keratoplasty for the management of a severe idiopathic lipid keratopathy
1Department of Ophthalmology, University of Lausanne, Jules-Gonin Eye Hospital, Fondation Asile des aveugles, Lausanne, Switzerland
2Department of Ophthalmology, National and Kapodistrian University of Athens, General Hospital “G. Gennimatas”, Athens, Greece
Author and article information
Cite this as
Kaisari E, Blavakis E, Kymionis G (2021) Penetrating keratoplasty for the management of a severe idiopathic lipid keratopathy. J Clin Res Ophthalmol. 2021; 8(2): 043-043. Available from: 10.17352/2455-1414.000092
Copyright License
© 2021 Kaisari E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.An 83-year-old female presented with progressive bilateral lipid keratopathy (LK) during the last 12 years. There was no history of previous ocular disease or trauma. Slit lamp examination of the left eye revealed a diffuse LK obscuring the visual axis and a temporal epithelial papillomatous lesion with superficial neovascularization (Figure A), while Best Corrected Visual Acuity (BCVA) was 20/200 with eccentric fixation. An uneventful Penetrating Keratoplasty (PKP) combined with excision of the temporal lesion was performed.
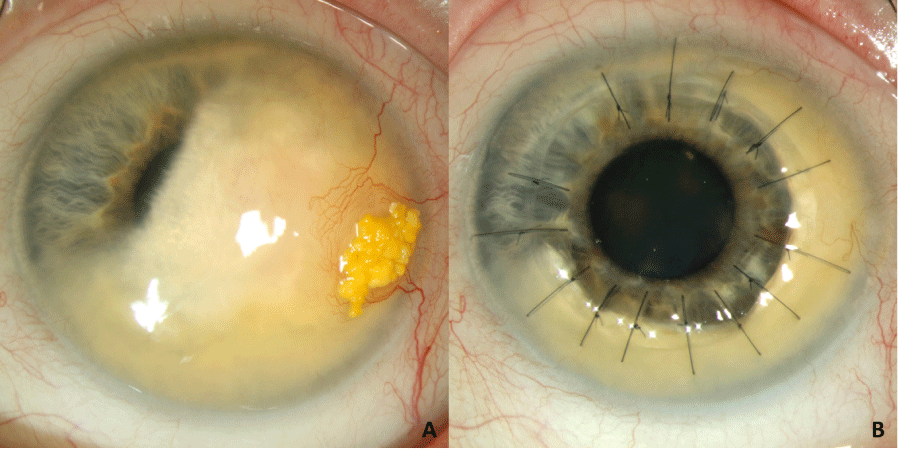
An 83-year-old female presented with progressive bilateral lipid keratopathy (LK) during the last 12 years. There was no history of previous ocular disease or trauma. Slit lamp examination of the left eye revealed a diffuse LK obscuring the visual axis and a temporal epithelial papillomatous lesion with superficial neovascularization (Figure A), while Best Corrected Visual Acuity (BCVA) was 20/200 with eccentric fixation. An uneventful Penetrating Keratoplasty (PKP) combined with excision of the temporal lesion was performed. Pathologic examination was indicative of LK, revealing chronic stromal inflammation including lymphocytes and histiocytes, partially xanthomized and the presence of cholesterol crystals. Two years post-operatively, the corneal graft was clear and BCVA was 20/20 following cataract surgery (Figure B). LK is either idiopathic, typically bilateral, or unilateral secondary to corneal neovascularization due to ocular disease or trauma [1]. Our case illustrates a severe form of idiopathic LK, treated successfully with PKP.
- Hall MN, Moshirfar M, Amin-Javaheri A, Ouano DP, Ronquillo Y, et al. (2020) Lipid Keratopathy: A Review of Pathophysiology, Differential Diagnosis, and Management. Ophthalmol Ther 9: 833–852. Link: https://bit.ly/3tk9d9D
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
