Journal of Clinical Research and Ophthalmology
Bilateral Retrobulbar HIV Optic Neuritis
Department of Ophthalmology, University Clinic Hospital of Valladolid, Spain
Author and article information
Cite this as
Asensio-Sanchez VM, Labrador-Velandia S (2015) Bilateral Retrobulbar HIV Optic Neuritis. J Clin Res Ophthalmol. 2015; 2(2): 026-027. Available from: 10.17352/2455-1414.000013
Copyright License
© 2015 Asensio-Sanchez VM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The human immunodeficiency virus (HIV) manifests in various ways in the eye. Several optic nerve disorders have been described, most commonly resulting from neoplasms, opportunistic infections, and inflammatory causes [1-4]. HIV itself may be a direct cause of optic neuropathy. It is an uncommon presentation and a diagnosis of exclusion, with only a few cases described in the literature [5-7].
Purpose
The purpose of this report is to present a case of bilateral retrobulbar optic neuropathy in an HIV-positive patient without treatment.
Case Report
The authors obtained written consent from the patient for the publication of her anonymised clinical data.
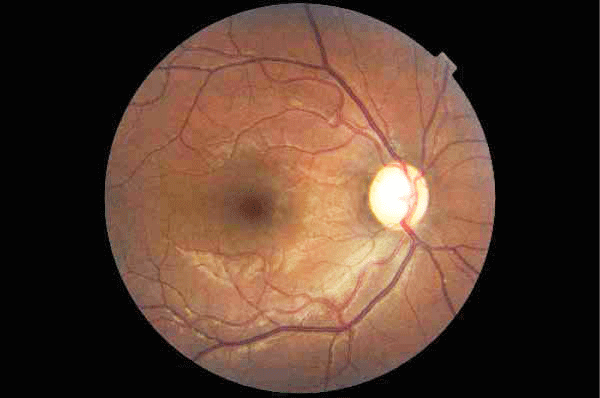
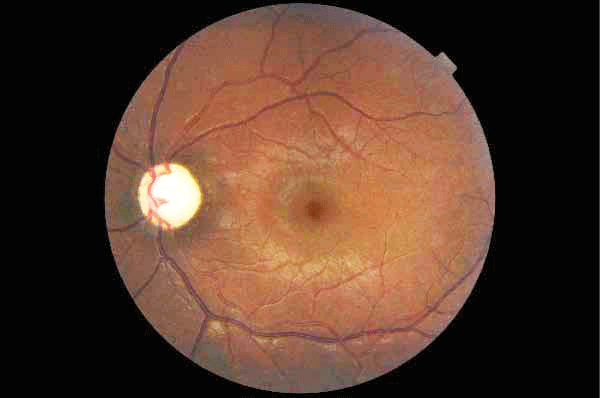
A 25-year-old woman presented bilateral visual loss. Past medical history was significant for HIV test in 2008 but no AIDS-defining illness. She declined antiretroviral therapy. Past ocular history was non-contributory, and results from previous eye exams were normal. She developed painful bilateral simultaneous progressive visual loss for the previous 3 months. Her best-corrected visual acuity was 20/200 OD and amaurosis OS. She saw 2/13 Ishihara plates OD and none OS. Visual field was constricted in the OD. The pupils were sluggishly reactive OU. Motility, slit lamp, and retinal exam results were normal. The optic nerves showing bilateral optic disc pallor and atrophic, with more pallor OS than OD (Figures 1, 2). An extensive evaluation for other infectious causes of her visual loss were negative. CD4+ cell count was 20/μL and serum HIV RNA level was 190,000 copies/mL. The full blood count showed leukocytosis (white cell count 13×10˄9 /L) with neutrocytosis (78%).
The human immunodeficiency virus (HIV) manifests in various ways in the eye. Several optic nerve disorders have been described, most commonly resulting from neoplasms, opportunistic infections, and inflammatory causes [1-4]. HIV itself may be a direct cause of optic neuropathy. It is an uncommon presentation and a diagnosis of exclusion, with only a few cases described in the literature [5-7].
Purpose
The purpose of this report is to present a case of bilateral retrobulbar optic neuropathy in an HIV-positive patient without treatment.
Case Report
The authors obtained written consent from the patient for the publication of her anonymised clinical data.
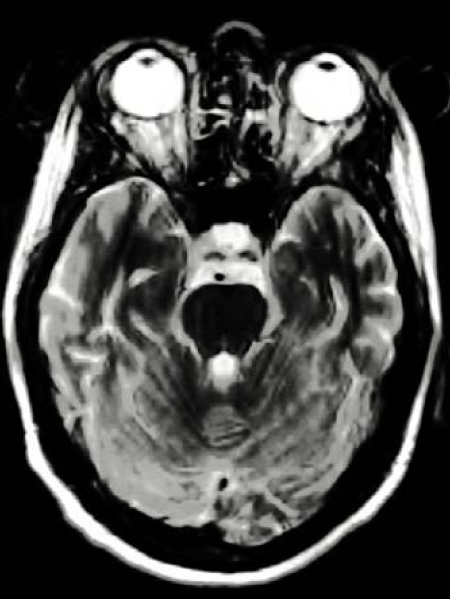
A 25-year-old woman presented bilateral visual loss. Past medical history was significant for HIV test in 2008 but no AIDS-defining illness. She declined antiretroviral therapy. Past ocular history was non-contributory, and results from previous eye exams were normal. She developed painful bilateral simultaneous progressive visual loss for the previous 3 months. Her best-corrected visual acuity was 20/200 OD and amaurosis OS. She saw 2/13 Ishihara plates OD and none OS. Visual field was constricted in the OD. The pupils were sluggishly reactive OU. Motility, slit lamp, and retinal exam results were normal. The optic nerves showing bilateral optic disc pallor and atrophic, with more pallor OS than OD (Figures 1, 2). An extensive evaluation for other infectious causes of her visual loss were negative. CD4+ cell count was 20/μL and serum HIV RNA level was 190,000 copies/mL. The full blood count showed leukocytosis (white cell count 13×10˄9 /L) with neutrocytosis (78%). The erythrocyte sedimentation rate was increased at 65 mm/h, with the C-reactive protein level at 7.2 mg/l. Additional laboratory tests including ANA, p/c ANCA, anti-ds DNA-Ab, antiphospholipid Ab, vitamin B12, folic acid were performed without any pathological findings. The chest radiograph was normal. A CT scan of the brain with contrast showed mild atrophy, but a magnetic resonance imaging scan (MRI) showed diffuse enhancement of the bilateral optic nerves post-contrast (Figure 3). There were no periventricular plaques. Lumbar puncture disclosed an opening pressure of 20 cm H2O and cerebrospinal fluid (CSF) chemistry and cytology were normal, including normal protein, glucose levels, and cell count. CSF cytology was negative for malignancy. Oligoclonal bands were negative. Results of a VDRL test, a Cryptococcus antigen test, an acid-fast stain, a Mycobacterium tuberculosis polymerase chain reaction (PCR) assay, and all cultures (bacteria, fungi, viruses, and mycobacteria) were negative.
Discussion
Optic neuritis is an inflammation of the optic nerve accompanied by impaired central or paracentral vision [8]. In a few cases, a primary demyelinating process in the optic nerve is not the cause of retrobulbar optic neuritis. The differential diagnosis of a bilateral optic neuritis includes papilledema, infiltrative optic neuropathy, toxic/nutritional optic neuropathy and, hereditary optic neuropathy [8]. In papilledema, the vision is initially normal, and the visual field may be normal or with an enlargement of the blind spot. Orbital lesions compressing the optic nerve and infiltrative disease of the optic nerve may cause disc edema and visual loss. Toxic or nutritional optic neuropathies are notable for a normal optic disc or mild temporal pallor. Leber´s hereditary optic neuropathy typically affects males between 10 and 30 years of age, and Kjer dominant optic atrophy affects males and females between 4 to 8 years of age. Most cases of optic neuropathy in patients with HIV infection are associated with opportunistic infections as systemic viral diseases such as hepatitis B virus infection, herpesviridae family or bacterial diseases, as Lyme disease, tuberculosis and syphilis. Evaluation of visual loss in patients with AIDS is complex, requiring investigation of infectious causes. The proposed mechanisms for the clinical findings of the HIV-mediated optic neuropathy include direct or indirect neurotoxic effects of the HIV-1 infection on the optic nerve similar to that seen in the CNS [5-7]. Some patients with AIDS develop patchy and scattered degeneration of ganglion cell axons throughout the optic nerve by HIV itself suggest that AIDS-associated optic neuropathy is a distinct primary optic nerve degeneration that is unrelated to secondary retinal or optic nerve infections [9-11].
Conclusion
We describe a woman with advanced HIV infection with profound immunosuppression in whom bilateral retrobulbar optic neuritis developed as a result of HIV virus itself. We can exclude the possibility that our patients´s optic neuropathies were caused by another infection. The diagnosis of HIV retrobulbar optic neuritis was based on a normal anterior segment, pupillary defects, ocular pain progressing over days, appearance of optic nerve pallor late in the disease course, compatible MRI findings, and lack of evidence of alternative causes on the basis of comprehensive serum and CSF test results, and radiological findings.
Summary Statement
We report on an infrequent case of bilateral retrobulbar optic neuropathy as symptom of in an HIV-positive patient.
- Vrabec TR (2004) Posterior segment manifestations of HIV/AIDS. SurvOphthalmol 49:131-157 .
- Goldsmith P, Jones RE, Ozuzu GE, Richardson J, Ong EL (2000) Optic neuropathy as the presenting feature of HIV infection: Recovery of vision with highly active antiretroviral therapy. Br J Ophthalmol 84:551-553 .
- Mwanza JC, Nyamabo LK, Tylleskär T, Plant GT (2004) Neuro-phthalmological disorders in HIV infected subjects with neurological manifestations. Br J Ophthalmol 88:1455-1459.
- Gordon LK(2005) Retroviruses and retroviral diseases. In: Miller NR,Newman NJ, eds. Walsh and Hoyt's Clinical Neuro-Ophthalmology 6thedition. Lippincott Willliamsand Wilkins 3323-3368.
- Newman NJ, Lessel S (1992) Bilateral optic neuropathies with remission in two HIV-positive men. J ClinNeruoOphthalmol 12:1-5.
- Sweeney BJ,Manji H, Gilson RJC, Harrison MJG (1993) Optic neuritis and HIV-1 infection. J NeurolNeurosurg Psychiatry 56:705-707 .
- Larsen M, Toft PB, Bernhard P, Herning M (1998) Bilateral optic neuritis in acute human immunodeficiency virus infection. ActaOphthalmolScand76:737-738 .
- Voss E, Raab P, Trebst C, Stangel M (2011) Clinical approach to optic neuritis: pitfalls, red flags and differential diagnosis. TherAdvNeurolDisord 4: 123-134 .
- Tenhula WN, Shizao X, Madigan MC, Heller K, Freeman WR, et al. (1992) Morphometric Comparison of Optic Nerve Axon Loss in AcquiredImmunodeficiency Syndrome. Am J Ophthalmol 113:14-20 .
- Sadun AA, Pepose JS, Madigan MC, Laycock KA, Tenula WN, et al.(1995) AIDS-related optic neuropathy: a histological, virological and ultrastructural study. Graefes Arch ClinExpOphthalmol 233:387-398 .
- Mahadevan A, Satishchandra P, Prachet KK, Sidappa NB, Ranga U, et al. (2006) Optic nerve axonal pathology is related to abnormal visual evoked responses in AIDS. ActaNeuropathol 112:461-469 .
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
