Journal of Clinical Research and Ophthalmology
Needle Revision with Antimetabolites in Bleb Failure
Ehab Ghoneim, MD, Professor of Ophthalmology, Suez Canal University, Ismailia, 6532, Egypt
Author and article information
Cite this as
Ghoneim E (2015) Needle Revision with Antimetabolites in Bleb Failure. J Clin Res Ophthalmol. 2015; 2(1): 7-9. Available from: 10.17352/2455-1414.000008
Copyright License
© 2015 Ghoneim E. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Glaucoma filtering surgery is unusual in that its goal is the creation and maintenance of a non healing fistula between two anatomic spaces that are normally not connected [1].
Fibroblasts, connective tissue elements, cytokines, aqueous humor and the surrounding vascular supply all influence what happens to a bleb over a long period of time.
The enemy of drainage procedure is excessive scarring [2].
Long-term studies showed a loss of intraocular pressure (IOP) control in a significant proportion of eyes with an initially successful trabeculectomy [2,3]. So follow up of glaucoma patients after surgery is mandatory as significant proportion develop bleb failure.
Revision of guarded filtration procedures was reported as early as 1941 by Ferrer [4]. Needling as currently performed was described by Pederson and Smith [5]. The combination of needling with antimetabolites (mitomycin C and 5FU) greatly improve the outcome of needling and enhance bleb survival.
Glaucoma filtering surgery is unusual in that its goal is the creation and maintenance of a non healing fistula between two anatomic spaces that are normally not connected [1].
Fibroblasts, connective tissue elements, cytokines, aqueous humor and the surrounding vascular supply all influence what happens to a bleb over a long period of time.
The enemy of drainage procedure is excessive scarring [2].
Long-term studies showed a loss of intraocular pressure (IOP) control in a significant proportion of eyes with an initially successful trabeculectomy [2,3]. So follow up of glaucoma patients after surgery is mandatory as significant proportion develop bleb failure.
Revision of guarded filtration procedures was reported as early as 1941 by Ferrer [4]. Needling as currently performed was described by Pederson and Smith [5]. The combination of needling with anti metabolites (mitomycin C and 5FU) greatly improve the outcome of needling and enhance bleb survival.
Bleb morphology
Most filtering blebs contain loculations that are delimited by internal fibrous walls. In bleb development, the walls are formed from conjunctival adherence to the underlying sclera and episclera. The main loculation is formed at the sclerostomy site and may be surrounded by other, usually smaller, loculations [6].
Phases in life of the bleb
Formation phase.Comprise roughly the first two week, successful blebs showed common characteristics (elevation and avascularity). They may be diffuse or localized, thin walled or spongy and they differ in height, pallor and extent of conjunctival micro cystic edema.
Establishment phase: The bleb wall is elevated and the wall appears tense and cystic.
Mature phase: May be functional blebs which usually multi loculated bleb. While failed blebs are often totally flat and vascularized.
Encapsulated blebs: Defined as highly elevated, tense, thickened, dome-shaped or sausage shaped blebs occurring within 3 months after trabeculectomy. A significant proportion of these blebs resolve without surgical intervention [6].
Bleb failure
The signs of bleb failure include sub conjunctival cyst disappearance, increased vascularity, decreasing area of bleb and elevated intraocular pressure (IOP) [6]. Those patients at high risk of bleb failure are Africans, with previous ocular inflammation, prolonged topical medication (miotics and sympathomimetics) and aphakia. As there were a great tendency to subconjunctival, episcleral and scleral fibrosis [7]. The clinical appearance of a bleb is not always an accurate predictor of functional status as a small proportion of flat blebs are functioning well, also blebs are dynamic structure and remodeling takesover time [6].
Bleb management
For successful glaucoma surgery, close follow up and early intervention is recommended to manage complications and to maintain the delicate balance between maintaining the integrity of the eye and prevention of excessive scarring [2,6].
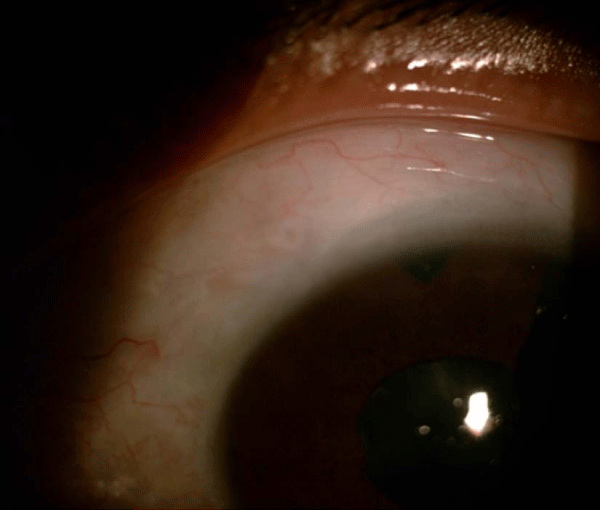
Needling is indicated when there is inadequate IOP control with an elevated bleb with microcysts, flat bleb with visible scleral flap without micro cyst (Figure 1), postoperative need of topical ocular hypotensive medication and some eyes with encapsulated bleb [8].
Needling is performed by lysing or puncturing bands of fibrous tissue that define the margins of areas with good filtration from areas with little or no filtration. These bands may be in the bleb itself or may be episcleral and tightly adherent to the scleral flap [8].
Early intervention in case of bleb failure was supported by several studies. They recommend performingMMC needling when signs of failure are detected during the cellular phase, which starts several weeks after surgery [1,7,8].
Intra operative signs of good needling include softening of the eyeball, release of aqueous humor into the sub conjunctival space, which created a raised conjunctival bleb, and occasionally a small reflux of blood into the anterior chamber (AC) [8].
Poor needling response is anticipated with the need for multiple needle revision procedures.Flat bleb that tightly adherent to episclera, higher pre needling IOP and immediate post-needling IOP over 19mm Hg [9].
Bleb failure (Needling or ocular hypotensive drugs)
The use of ocular hypotensive medications reduces aqueous flow into a filtering bleb. This decreases the volume of the bleb, thereby increasing the degree of contact between the conjunctiva and the underlying sclera and potentiating fibrosis [8].
This is the rationale for early needle revision in eyes with functional trabeculectomies but inadequately controlled IOP.
Antimetabolites and needling
Chen [10] was the first to use MMC intra-operativly for refractory glaucoma. Ewing and Stamper [11], first reported the use of 5-fluorouracil (5-FU) with needling and Mardelli et al. [12] first described needling with MMC in 1996.
As the main cause of bleb failure is excessive fibrosis so the need of anti fibrotic agents is essential to obtain successful needling [1].
The dose of subconjunctival MMC used in different needling's studies varied significantly. Chen et al. [10] reported that a concentration of 0.1 mg/ml MMC inhibits fibroblast replication while concentrations of 0.3 mg/ml cause fibroblast cell death [10].
Titration of the optimal dose of MMC remains an art rather than a science, too little MMC may make fistula to close soon after surgery and too much MMC may lead to avascular bleb and delayed leaks with their problems.
Most studies of needling used MMC concentration ranged from 0.4mg/ml to 0.2 mg/ml as subconjuctival injection. The severity of glaucoma, racial factor and experience of the surgeon with MMC, all such factors play a rule in the selection of MMC dose. The usual dose of subconjunctival injection of 5-FU is 5 mg [1].
Mitomycin C has some advantages over 5-FU, it has less corneal epithelial toxicity, higher potency, and the need for only a single intra operative application [11,13].
However MMC is contraindicated in glaucoma surgery in patients with ocular rosacea, sjogren's syndrome, anterior uveitis, scleritis, immune disorder sand old age above 70 years. In such patients the possibility of scleritis, scleral perforations, cataract formation and corneal perforations is high [14].
The possible complications of mitomycin C is cataract, prolonged hypotony, maculopathy, blebitis and epitheliopathy [8].
Topical MMC in trabeculectomy
Velpandian et al. [15] estimate transconjunctival penetration of MMC (0.4 mg/mL) to Tenon tissue after application overthe intact conjunctiva before routine trabeculectomy.Tenon capsule directly beneath the site of application was excised during trabeculectomy and MMC concentrations were analyzed. They found that MMC concentration reached above the tissue concentration required to inhibit human conjunctival fibroblasts.
Topical MMC with needling
The advantages of topical application of MMC instead of subconjunctival injection is to avoid conjunctival elevation so needling manipulations can be seen easily, less chance of subconjunctival hemorrhage and avoid escape of mitomycin C in to AC during manipulations.
The use of topical application of MMC before bleb revision is a recent technique by Ghoneim et al. [16], as most studies use subconjunctival injection of MMC before needling; only Iwach et al. [17] used topical application of MMC over conjunctiva after needling procedure.
It is difficult to compare needling studies because of differences in surgical techniques, success criteria, antimetabolite type and dose, timing of the needling procedure, and follow-up period.
Gauge needles 30 or 25
Thirty gauge needles usually result in self-sealing entry sites; sometimes, the needle is flexible to adequately penetrate and cut dense subconjunctival fibrotic tissue.Twenty-five–gauge needles penetrate well, occasionally self-seal, but usually need to be closed with bipolar cautery or suture, 27 and 28-gauge needles fall in between.
Slit lamp versus operating room
Operating room advantages: In the operating room there is an increased patient comfort, two handed procedure, wide field of view and presumed lower risk for infection [16].
Slit Lamp Advantages: It is outpatient procedure with less time consuming, less patients stressand the main advantage is precise identification of Tenon'scapsule [18].
Slit lamp needling
The slit lamp is set at the lowest magnification. This facilitates visualization of the bleb.
A tuberculin syringe with a 30 or 27-gauge needle was introduced as far superiorly as possible away from the bleb.The needle is advanced carefully beneath the Tenon's space till the scleral flap is reached.If possible, the needle is placed under the scleral flap and used to lift the flap [18].
The future
Three - dimensional anterior segment optical coherence tomography (OCT)not only is useful for bleb revision but also provides important information regard the internal morphology of the blebs, the precise identification of filtration openings from margins of the scleral flap which may affect the plan for needling [19].
Conclusions
Needling has the potential to be as effective as a trabeculectomy, with lower cost and less surgical trauma. Needling alone without anti proliferative drugs does not overcome the major problem, which is episcleral fibrosis due to fibroblast activity.Needling without antimetabolites like photorefractive keratectomy without mitomycin C, both techniques needs antimetabolites to avoid fibroblastic activity.
- Broadway DC, Bloom PA, Bunce C (2004) Needle revision of failing and failed trabeculectomy blebs with adjunctive 5-fluorouracil : survival analysis. Ophthalmology 111: 665-673 .
- Wilensky JT, Chen TC (1996) Long-term results of trabeculectomy ineyes that was initially successful, Trans Am Ophthalmol Soc 94: 147-159 .
- Suzuki R, Dickens CJ, Iwach AG (2002) Long-term follow-up of initially successful trabeculectomy with 5-fluorouracil injections, Ophthalmology 109: 1921-1924 .
- Ferrer H (1941) Conjunctival dialysis in the treatment of glaucoma recurrent after sclerectomy. Am J Ophthalmol 24: 788-790.
- Pederson JE, Smith SG (1985) Surgical management of encapsulated filtering blebs. Ophthalmology 92: 955-958 .
- Skuta GL, Parrish RK (1987) Wound healing in glaucoma filtering surgery. Surv Ophthalmol 32: 149-170 .
- Broadway DC, Chang LP (2001)Trabeculectomy, risk factors for failure and the preoperative state of the conjunctiva. J Glaucoma 10: 237-249 .
- Feldman R, Tabet R (2008) Needle revision of filtering blebs. J Glaucoma 17: 594-600.
- Ben-Simon GJ, Glovinsky Y (2003) Needle revision of failed filtering blebs augmented with subconjunctival injection of mitomycin C. Ophthalmic Surg Lasers Imaging 34: 94-99 .
- Chen CW, Huang HT, Bair JS, Lee CC (1990) Trabeculectomywith simultaneous topical application of mitomycin-C inrefractory glaucoma. J Ocul Pharmacol 6: 175-182 .
- Ewing RH, Stamper RL (1990) Needle revision with and without 5-fluorouracil for the treatment of failed filtering blebs. Am J Ophthalmol 110: 254-259 .
- Mardelli PG, Lederer CM Jr, Murray PL (1996) Slit-lamp needle revision of failed filtering blebs using mitomycin C . Ophthalmology 103: 1946-1955 .
- Anand N, Khan A (2009) Long-term outcomes of needle revision of trabeculectomy blebs with mitomycin C and 5-fluorouracil: a comparative safety and efficacy report. J Glaucoma 18: 513-520 .
- Rubinfeld RS, Pfister RR, Stein RM, Foster CS, Martin NF, et al. (1992) Serious complications of topical mitomycin-C after pterygium surgery. Ophthalmology 99: 1647-1654 .
- Velpandian T, Sihota R, Sinha A, Gupta V (2008) Transconjunctival penetration of mitomycin C. Indian J Ophthalmol 56: 197-201 .
- Ghoneim EM, Abd El Hameed M (2011) Needling augmented with topical application of mitomycin C for management of bleb failure. J Glaucoma 20: 528-532 .
- Iwach AG, Delgado MF, Novack GD (2003) Transconjunctival mitomycin-C in needle revisions of failing filtering blebs. Ophthalmology 110: 734-742 .
- Shetty R, Wartluft L, Moster M (2005) Slit-lamp needle revision of failed filtering blebs using high-dose mitomycin , J Glaucoma 14: 52-56 .
- Inoue T, Matsumura R, Kuroda U, Nakashima K, Kawaji T, et al. (2012) Precise identification of filtration openings on the scleral flap by three-dimensional anterior segment optical coherence tomography. Invest Ophthalmol Vis Sci 53: 8288-8294 .
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
