Imaging Journal of Clinical and Medical Sciences
Cone cavernoma with a twice secondary intramedullary hemorrhage
1Neurosurgery Department, Salamanca University Hospital, Spain
2Primary Care Department, Salamanca University Hospital, Spain
Author and article information
Cite this as
Garrido Ruiz PA, Garrido MR (2023) Cone cavernoma with a twice secondary intramedullary hemorrhage. Imaging J Clin Medical Sci. 2023; 10(1): 1-3. Available from: 10.17352/2455-8702.000139
Copyright License
© 2023 Garrido Ruiz PA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Possible complications that may occur and how to solve them before surgery are essential. This case is of special interest for being a low-incidence pathology in a rare location. The case is of high interest because of the importance of evacuating the hemorrhage to prevent sequels and the complexity of its management and highlights the importance of considering the diagnosis of this event.
We present a type II cavernoma in the medullary cone with two episodes of sudden deficit due to hemorrhage. This report describes a type II cavernoma located at the conus medullaris, which is rare as there are few reported cases of cavernomas occurring at this location in the literature. The case is of great interest because the conus medullaris is a rare location of cavernoma [1-4] with few cases reported in the literature and because of the importance of keeping in mind its diagnostic possibility.
Materials & methods
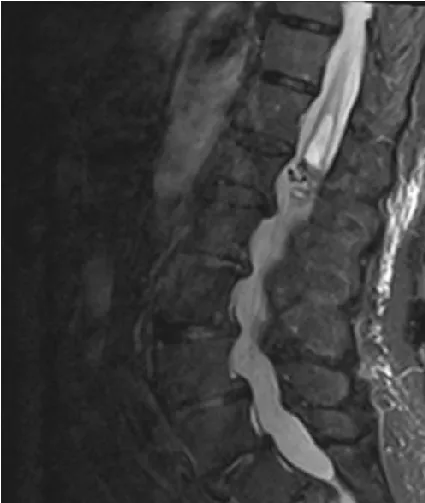
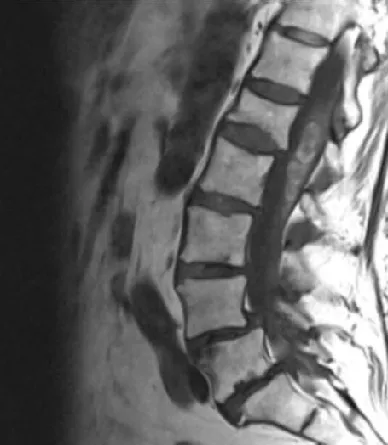
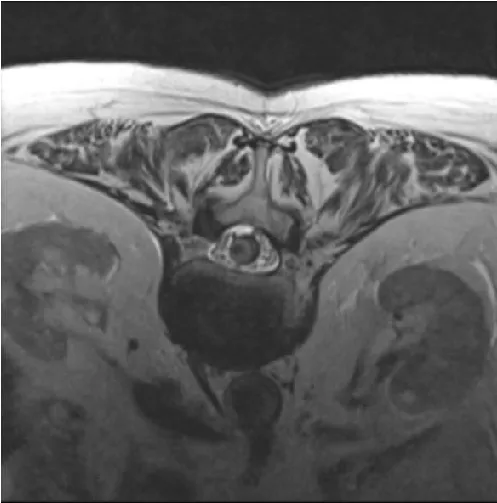
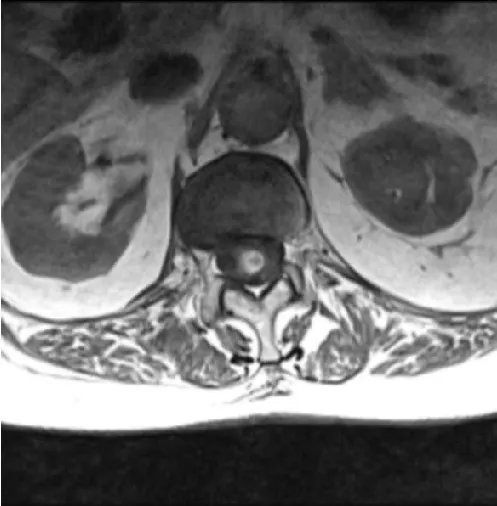
We present the case of an 80-year-old patient with sudden neurological deterioration, who debuted with hypoesthesia in the saddle, acute urinary retention, hypoesthesia, and loss of strength in the right lower limb. A spinal cord magnetic resonance was performed, showing hemorrhage in the conus medullaris cavernoma, diagnosed 20 years ago that remained asymptomatic. Despite presenting some improvement after medical treatment and rehabilitation, he suffered a second hemorrhage in 4 weeks. Hemorrhage affecting the spinal cord is rare. Spinal cord hemorrhage can be divided based on etiology, into two types: traumatic and non-traumatic. It can also be divided based on the compartment into which the hemorrhage occurs, namely: intramedullary (including hematomyelia), Subarachnoid (SAH), Subdural (SDH), and/or Epidural (EDH). Spinal cord hemorrhage is most commonly caused by trauma, vascular malformations, or bleeding diatheses. Spinal cord hemorrhage usually presents as sudden, painful myelopathy, which may reflect the anatomic level of the hemorrhage. For perfusion, three longitudinal vessels form an anastomotic network that supplies the spinal cord: two posterior spinal arteries, and the anterior spinal artery. Blood flows from the anterior spinal artery into medullary branches of the intradural vertebral arteries, and subsequently into segmental radiculomedullary arteries. Intramedullary spinal cord hemorrhage (hematomyelia) is an uncommon cause of myelopathy and can present in an acute, subacute, stepwise, or chronic fashion. Based on the existing literature, spinal vascular malformations such as intramedullary cavernous and intradural arteriovenous malformations are the most common cause of atraumatic intramedullary spinal cord hemorrhage. Additional considerations include warfarin or heparin anticoagulation, hereditary or acquired bleeding disorders, primary spinal cord tumors, spinal cord metastases, Gowers' intraspinal hemorrhage, or a delayed complication of spinal radiation. Prompt diagnosis of hematomyelia first requires recognition of a myelopathy syndrome (transverse, central, anterior, posterior, or hemi-cord) often accompanied by sudden, severe back or neck pain and sometimes radicular pain. MRI with and without gadolinium is the preferred imaging modality. There are no clinical trials to guide the management of acute intramedullary spinal cord hemorrhage, and subsequent treatment is usually directed toward the underlying cause (Figures 1-4).
Results
Complete resection of the cavernoma and intramedullary hematoma is performed under neurophysiological monitoring. Presenting the patient with a satisfactory clinical evolution, persisting the previous paresis. The pathology of the solid component was compatible with sinusoidal vessels with a diagnosis of cavernoma. The cystic component was made up of blood degradation products at different stages [5,6].
Conclusion
Intraspinal cavernomas are rare vascular lesions, intramedullary cavernomas accounting for approximately 5% - 12% of spinal cord vascular pathology. Only 7% of them are located in the lumbar region [1-3]. The cone-shaped cavernoma is rare and difficult to access. There are few cases described in the literature. In this location, the form of appearance after bleeding is rare and can be decisive [7]. It is important to keep in mind its diagnostic possibility in surgical treatment. Although there is a tendency in the literature to consider that all intramedullary cavernoma, especially if it is symptomatic, should be treated surgically, this approach must be individualized for each particular case.
- Youmans. Neurological Surgery. 7th Edition. October 11, 2016. Saunders Company.
- Rhoton. Rhoton's Cranial Anatomy and Surgical Approaches. Oxford University Press, 2019. Congress of Neurological Surgeons (CNS)
- Greenberg M. Handbook of Neurosurgery, Thieme, 2019. 9th Edition.
- Sharma R, Rout D, Radhakrishnan VV. Intradural spinal cavernomas. Br J Neurosurg. 1992;6(4):351-6. doi: 10.3109/02688699209023794. PMID: 1388829.
- Deutsch H, Jallo GI, Faktorovich A, Epstein F. Spinal intramedullary cavernoma: clinical presentation and surgical outcome. J Neurosurg. 2000 Jul;93(1 Suppl):65-70. doi: 10.3171/spi.2000.93.1.0065. PMID: 10879760.
- Badhiwala JH, Farrokhyar F, Alhazzani W, Yarascavitch B, Aref M, Algird A, Murty N, Kachur E, Cenic A, Reddy K, Almenawer SA. Surgical outcomes and natural history of intramedullary spinal cord cavernous malformations: a single-center series and meta-analysis of individual patient data: Clinic article. J Neurosurg Spine. 2014 Oct;21(4):662-76. doi: 10.3171/2014.6.SPINE13949. Epub 2014 Jul 25. PMID: 25062285.
- Steiger HJ, Turowski B, Hänggi D. Prognostic factors for the outcome of surgical and conservative treatment of symptomatic spinal cord cavernous malformations: a review of a series of 20 patients. Neurosurg Focus. 2010 Sep;29(3):E13. doi: 10.3171/2010.6.FOCUS10123. PMID: 20809754.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
