Global Journal of Anesthesiology
Comparison of Hyperbaric 0.5% Bupivacaine with Hyperbaric 0.5% Levobupivacaine for Spinal Anaesthesia in Lower Abdominal and Lower Limb Surgeries
MBBS, MD Anaesthesia, Clinical Associate, Department of Critical care, SPS hospital, Ludhiana Punjab, India
Author and article information
Cite this as
Sapra T, et al. Comparison of Hyperbaric 0.5% Bupivacaine with Hyperbaric 0.5% Levobupivacaine for Spinal Anaesthesia in Lower Abdominal and Lower Limb Surgeries. Glob J Anesth. ; 13(1): 6-12. Available from: 10.17352/2455-3476.000062
Copyright License
© This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: Spinal anaesthesia is widely used around the globe for surgeries involving lower abdomen, pelvis, and lower limbs. Bupivacaine and its S-enantiomer Levobupivacaine are among the most commonly used drugs for subarachnoid block.
Aims and objectives: The present study is aimed at comparing the efficacy of spinal anaesthesia (SA) performed with hyperbaric 0.5% Bupivacaine and hyperbaric 0.5% Levobupivacaine in patients undergoing lower abdominal and lower limb surgeries.
Materials and method: This was a double blinded prospective, randomised study conducted on 70 patients aged between 18 to 60 years of either sex, American Society of Anaesthesiologists’ class 1 and 2, posted for elective lower abdominal and lower limb surgeries under spinal anaesthesia for a period of 18 months. Patients were randomly divided into 2 equal groups: Group A patients received intrathecal dose of hyperbaric 0.5% Bupivacaine 2.5 ml(12.5 mg) with 25 ug Fentanyl [3 ml] while Group B patients received an intrathecal hyperbaric 0.5% Levobupivacaine 2.5 ml(12.5 mg) with 25 ug Fentanyl [3 ml].
Results: In our study, the intra-operative readings of various hemodynamic variables showed no significant differences among the patients in both the drug groups. The maximum level of sensory blockade as well as motor blockade was achieved earlier in group A patients in comparison to group B. Moreover, the duration of blocks was also found to be longer in patients who received bupivacaine in comparison to levobupivacaine. The time for the first analgesic was significantly delayed in group A patients in comparison to group B, which showed a significantly higher VAS score reading in the early post-operative period in the patients of group B.
Conclusion: Our study showed that, both intrathecal bupivacaine and levobupivacaine with fentanyl had equally good control of hemodynamic variables during intra-operative period as well as post-operatively. However, the patients who received intrathecal bupivacaine with fentanyl showed an early onset with longer duration of sensory as well as motor block in comparison to those who were administered intrathecal levobupivacaine with fentanyl. Also, in terms of analgesic potency and duration of analgesia, intrathecal bupivacaine showed better results than intrathecal levobupivacaine.
Hb: Hemoglobin; TLC: Total Leukocyte Count; CT: Computed Tomography, Inj: Injection
Introduction
The discovery of spinal anaesthesia marked a significant advancement in medical practice, primarily facilitated by the introduction of specialized needles and syringes, alongside an improved understanding of the anatomy and physiology of cerebrospinal fluid (CSF) [1]. In 1898, Karl Gustav Bier, a German surgeon, pioneered the successful use of operative spinal anaesthesia in lower limb surgery.
Spinal block is achieved by injecting a local anaesthetic agent into the subarachnoid space to interrupt the transmission of action potentials along the nerve fibres [2]. A small amount of local anaesthetic injected in the lumbar cerebrospinal fluid provides highly effective anaesthesia, analgesia, and sympathetic and motor block in the lower part of the body [3]. Spinal anaesthesia is a widely used technique for surgeries below the level of the umbilicus like hysterectomy, haemorrhoidectomy, hernioplasty, caesarean section, inguinal hernia repair, prostate surgeries, transurethral prostatic resection, genital surgeries and for a wide range of corrective orthopaedic procedures [4]. Spinal anaesthesia is increasingly favoured in modern medical practice due to a variety of benefits that enhance patient outcomes and satisfaction, few of which include- low complication rate, enhanced pain control, earlier recovery of bowel function, proven success and predictability, lesser need for systemic opioids, easier breathing, better patient satisfaction with easier participation in physical therapy [5]. The advantage of an awake patient with minimal drug cost and rapid patient turnover has made this the method of choice for many surgical procedures.
Spinal Anaesthesia has various contraindications that include lack of consent from the patient, infection at the procedure site (risk of meningitis), allergy to local anaesthetic agent, coagulation abnormalities, elevated intracranial pressure (ICP), severe dehydration (hypovolemia) with increased risk of hypotension, fixed cardiac output conditions like severe mitral and aortic stenosis and thrombocytopenia or coagulopathy [6,7]. Although, subarachnoid blocks are considered to be highly safe; however, these anaesthesia techniques are also associated with number of complications that include various minor complications like-bradycardia, hypotension, nausea, vomiting, shivering, and urinary retention [8], along with certain major ones like-post-dural puncture headache, vertebral canal hematoma, meningitis, total spinal blockade to a complete cardiovascular collapse and even death of the patient [9,10]. Local anaesthetics used in spinal anaesthesia primarily function by blocking the generation of action potentials in nerve cells. This occurs through the inhibition of sodium channels, which raises the threshold for electrical excitation, effectively preventing the transmission of pain signals [11].
Bupivacaine, an amino amide class local anaesthetic, is a racemic mixture of its R and S enantiomers, with a 50:50 composition. This drug can cause a rapid onset of sensory blockage within one minute, with maximum motor and sensory blockage achieved at 15 minutes following intrathecal administration [12]. However, bupivacaine is more cardiotoxic than other local anaesthetics and motor blockade accompanies the analgesia, especially at higher concentrations. This generated the search for an alternative to bupivacaine, concentrating on amide-linked agents, which in current practice have largely replaced ester-type drugs. In recent years, levobupivacaine, the pure S (-) enantiomer of bupivacaine, emerged as a safer alternative for regional anaesthesia than its racemic parent. Levobupivacaine has lower cardio-toxicity potential with a faster recovery profile. Its pharmacological action is characterized by the reversible blockade of voltage-gated sodium channels in neuronal membranes, which inhibits the propagation of action potentials in both sensory and motor nerves. The pharmacokinetic properties of levobupivacaine are similar to those of bupivacaine; both are extensively metabolised in the liver and excreted in the urine and faeces [13].
Guler G, et al in 2012 compared the effectiveness of levobupivacaine with bupivacaine in spinal anaesthesia during caesarean section and concluded that though the sensory and motor block characteristics were similar with both the drugs, side-effects like hypotension, bradycardia, nausea, along with the signs of CNS toxicity are less with levobupivacaine than bupivacaine [14]. Another study conducted by Santosh Alalamath in September 2024 concluded that the levobupivacaine group exhibited fewer adverse effects with significantly shorter durations of sensory as well as motor blockade in comparison to the bupivacaine group. Although the hemodynamic stability exhibited by both the drug groups was comparable [15].
Anatol J, during his research in 2025, compared levobupivacaine with bupivacaine concluding levobupivacaine to have a longer onset time for motor and sensory blockade compared to bupivacaine. However, the anaesthetic adequacy was not compromised, levobupivacaine showed a lower likelihood of inducing cardiac or central nervous system-related toxicity, especially for individuals with elevated perioperative risk [16].
Considering the relative advantages and disadvantages of both the drug, an endeavour was made to compare the onset, duration of sensory block and motor block, postoperative analgesia and hemodynamic changes occurring with hyperbaric 0.5% Bupivacaine and hyperbaric 0.5% Levobupivacaine when given intrathecally during spinal anaesthesia in lower abdominal and lower limb surgeries [17,18].
Aims and objectives
Primary outcome
To assess the efficacy, duration of sensory and motor blocks in patients receiving hyperbaric 0.5% Bupivacaine and hyperbaric 0.5% Levobupivacaine.
Secondary outcome
To study hemodynamic changes and complications if any.
To assess post-operative analgesia.
Materials and methods
Study design and participants
This was a prospective, randomized, double blind comparative study conducted on 70 patients aged between 18 and 60 years of either sex undergoing lower abdominal and lower limb surgeries under subarachnoid block, after ethical clearance was obtained under the institutional ethics committee with approval number: BFUHS/2K24p-TH/17719.
All the patients were randomly assigned to 2 equal groups (n = 35 each), using computer-generated software. Group A patients received hyperbaric 0.5% Bupivacaine 2.5 ml (12.5 mg) with 25 ug Fentanyl, a total of 3 ml, and Group B patients received hyperbaric 0.5% Levobupivacaine 2.5 ml (12.5 mg) with 25 ug Fentanyl, a total of 3 ml. All solutions were prepared by an anaesthetist who was not directly part of the study. The researcher gave spinal anaesthesia under aseptic conditions. Surgeons and researchers who were involved in patient clinical assessment and treatment were blinded to group assignment. All the patients were aged between 18 to 60 years of either sex, American Society of Anaesthesiologists’ class 1 and 2, posted for elective lower abdominal and lower limb surgeries under spinal anaesthesia. A detailed history along with a complete physical examination was done, relevant investigations were checked, and informed consent was taken from every participant.
Anaesthesia protocol
The patients were kept nill orally for 6 hours before the surgery for solid food and 2 hours for clear liquids. On the day of surgery, all the patients were pre-medicated with Tab. Alprazolam 0.5 mg and Tab. Ranitidine 150 mg orally 2 hours before the surgery. Monitoring was done using multiparameter monitor having pulse oximetry, Electrocardiogram (ECG), and non-invasive blood pressure (NIBP). Patients were pre-loaded with Ringer’s lactate @10 ml/kg/wt.
The parameters studied were: - onset and duration of sensory blockade as well as motor blockade, total duration of analgesia with analgesic requirement, haemodynamics, along with side effects if any.
Sensory blockade was recorded bilaterally using the pinprick method by use of a hypodermic needle every one minute till no sensation (grade 2) was achieved. Grading of Sensory block done according to GROMLEY AND HILL (17) as: -Normal sensation -0, Blunted sensation-1, No sensation -2.
Motor block was assessed using the MODIFIED BROMAGE SCALE (18) as: Grade 0, No paralysis to Grade 3, complete motor block, where the patient is unable to move any part of the lower limb.
Heart rate, systolic blood pressure, diastolic blood pressure, mean arterial pressure and Spo2 were recorded using standard non-invasive monitors before intrathecal injection (baseline) and thereafter at 5,10 and then at every 10 mins till 180 mins as well as post operatively(0 minute), at 30 mins followed by hourly monitoring till 4 hours. Pain assessment was done intra-operatively as well as postoperatively using visual analogue scale (VAS) between 0-10 (0-no pain, 10-most severe pain) every 1 hour for 4 hours postoperatively.
Statistical analysis
The minimum sample size was calculated to be n = 70, 35 in each group, by using the formula N=(Z1-α/2+Z1-β)2*4σ 2 / (μ1-μ2)2, where Z1-α/2 = 1.96, is standard normal deviate at type 1 error α = 0.05, Z1-β = 0.84 is standard normal deviate at type 2 error β = 0.20, σ is the pooled standard deviation and (μ1-μ2) is the detectable difference in the mean duration of analgesia. The difference in mean duration of analgesia in levobupivacaine and hyperbaric bupivacaine is 74 minutes derived from the prior literature.
Results
Demographic and baseline characteristics
In this study, participants in both the groups had similar distribution of age, gender and ASA grading. The mean time taken for the completion of surgery in Group A was 92.29 minutes, which was observed to be longer than 83 minutes seen in patients belonging to group B.
Intraoperative haemodynamic parameters
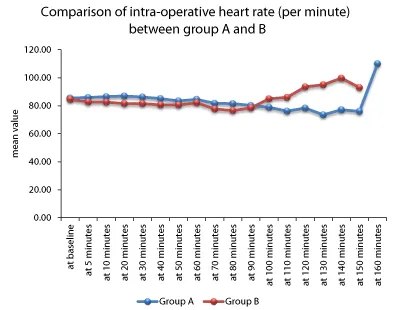
Heart rate: Our present study, observed the values for heart rate at zero minutes was comparable between the patients belonging to the groups A and B (p value 0.795).
In group A, the mean values for heart rate showed an increasing trend at 5,10, 20 & 30 mins after which it showed a decreasing trend from the baseline values at all the observed timings. In group B, the mean values for heart rate showed a decreasing trend from the baseline values during first 90 minutes of the surgery, with the maximum dip in heart rate observed at 80 minutes. Afterwards, the heart rate kept on increasing until the surgery got completed.
‡Independent t test (Figure 1)
Blood pressure (SBP, DBP, MAP)
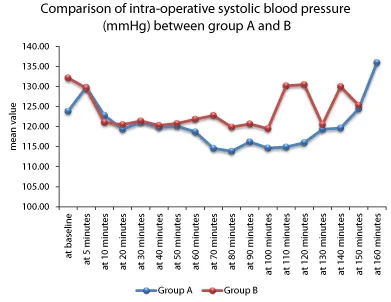
In our study, no significant differences were observed in systolic blood pressure (SBP), diastolic blood pressure (DBP), or mean arterial pressure (MAP) between the two groups. On analysing, the values for blood pressure remained almost similar and insignificantly different among the patients belonging to the two drug groups receiving different intrathecal drugs at different intervals of time starting from 0 minutes (baseline) to 3 hours.
‡Independent t test (Figure 2)
Oxygen saturation (SpO2): In our experimental trials, both groups maintained adequate oxygen saturation levels (SpO2 > 96% throughout surgery), with no significant intergroup differences.
Sensory block
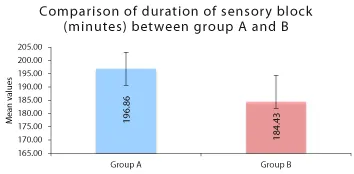
In our study, the mean ± SD onset of sensory block along with the time taken to achieve highest level of sensory block was shorter in patients belonging to group A (3.89 ± 0.87 minutes) compared to group B (5.1 ± 1.6 minutes) (p value = 0.0002). Furthermore, the duration of sensory block was also found to be subjectively longer in group A patients in comparison to group B.
‡Independent t test (Figure 3)
Motor block
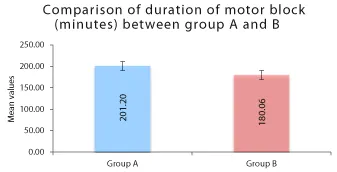
Our study analysed, Mean ± SD onset of motor block along with the time taken to achieve highest level of motor block was lower in patients belonging to group A (5.33 ± 1.18 minutes) in comparison to group B (7.04 ± 2.17 minutes) (p value = 0.0001). Furthermore, the duration of motor block was also found to be subjectively longer in group A patients in comparison to group B.
‡Independent t test (Figure 4)
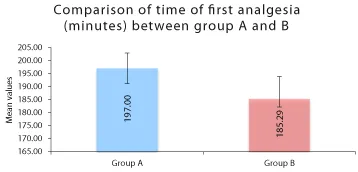
Time for first analgesic
In our study, time for first analgesic was 197 ± 13.13 minutes in patients from group A, while it was 185.29 ± 15 minutes among patients from B group, interpreting early analgesic requirement with shorter sensory block duration among patients who received intrathecal levobupivacaine in comparison to the ones who received intrathecal bupivacaine.
‡Independent t test (Figure 5)
Intra-operative & post-operative side effects/adverse events till 24 hours
We observed no significant differences in intra-operative or post-operative side-effects/adverse events till 24 hours among the two drug groups. In our study, all the patients were effectively pre-loaded with intravenous fluids, thus we observed minimal incidence of nausea and vomiting with least number of cases of hypotension.
*Fisher’s exact test, †Chi square test (Table 1)
Post-operative haemodynamics
Post-operative heart rate: Our study observed no significant differences in post-operative pulse rate between group A vs. group B at different time points, starting from 0 hours to 4 hours post-surgery.
Post-operative Blood pressure (SBP, DBP, MAP): In our study, post-operative blood pressure readings were analysed at 0 hour, ½ hour, 1 hr, 2 hrs, 3 hrs and 4 hours post-surgery. However, on statistical analysis no conclusive differences were seen in post-operative blood pressure recordings among the two drug groups.
Post-operative SPO2: Our study observed no statistical difference in post-operative SPO2 values between two drug groups at various time intervals.
Time period of analgesia
In our study, patients in the two study groups had similar distribution of analgesic duration with post-operative VAS scores slightly lower in A group in comparison to group B (0% vs. 2.86%), interpreting a slight superior analgesic potency of intrathecal bupivacaine in comparison to levobupivacaine.
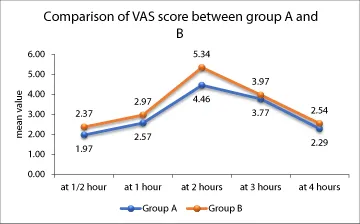
VASCORE
In our study, VAS score was monitored for post-operative pain in patients till 4 hours of surgery and the results demonstrated differences in scoring at ½ hour and 2 hours between group A and group B. On analyses, mean value for VAS score was lower in A group at ½ hour (1.97 ± 0.57 vs. 2.37 ± 0.88) and at 2 hours (4.46 ± 1.75 vs. 5.34 ± 1.49) compared to group B. Henceforth, our results demonstrated longer analgesic duration with low VAS scoring in patients who were administrated hyperbaric preparation of bupivacaine in comparison to hyperbaric levobupivacaine.
‡Independent t test (Figure 6)
Discussion
Sensory block
From present study, it was observed that the patients who received intrathecal bupivacaine had a quick and early attainment of highest level of sensory block along with a longer effective duration of the block in comparison to patients who received intrathecal levobupivacaine. These observations are in concordance with the results of Girish B.K., et al. in his trials on comparative efficacy of hyperbaric bupivacaine versus levobupivacaine in subarachnoid block for elective surgeries [19].
Although, the difference can be modest, but bupivacaine generally shows a marginal edge in observations due to its racemic nature. The (R- & S-) forms in the mixture of bupivacaine are more lipophilic in comparison to its pure S-enantiomer levobupivacaine, causing easy membrane permeability with higher lipid solubility, thus contributing to quicker diffusion with early completion and faster attainment of sensory blockade using intrathecal bupivacaine in comparison to intrathecal levobupivacaine. Moreover, levobupivacaine has less affinity for cardiac and neural sodium channels, which might contribute to slight shorter duration of action with this drug.
Motor block
Our study analysed that the patients who received intrathecal bupivacaine had a quick and early attainment of highest level of motor block along with a longer effective duration of the block in comparison to patients who received intrathecal levobupivacaine. In the study of Camorcia, et al. [20] the potencies for motor block of intrathecal ropivacaine, levobupivacaine, and bupivacaine were compared, and weaker motor block potency and shorter time period of motor block were reported with levobupivacaine group.
The S-enantiomer, levobupivacaine undergoes more rapid clearance of its unbound fraction than the R+enantiomers resulting in shortening of the effective duration of sodium channel blockade in motor fibres and thus, limiting the motor block duration with levobupivacaine in comparison to bupivacaine.
Analgesic potency
Our study interpreted an early analgesic requirement with shorter sensory block duration among patients who received levobupivacaine in comparison to the ones who received bupivacaine. Bupivacaine was observed to be associated with slightly longer lasting pain relief, reflected by lower VAS scores during post-operative period while, levobupivacaine with slight shorter sensory block duration showed high VAS scores once the regression of block occurred.
The clinical trials of Girish B.K., et al. demonstrated results consistent with our findings, holding bupivacaine superior to levobupivacaine with respect of analgesic potency [18].
Hemodynamic variations
Our study analysed that the patients in both the drug groups are comparable with respect to blood pressure, heart rate, and SpO2 values over various time intervals intra-operatively as well as post-operatively. The above findings in context to hemodynamic variables are in concordance with the observations of Thakore, et al. in his study comparing the efficacy of low-dose hyperbaric levobupivacaine (0.5%) versus hyperbaric bupivacaine (0.5%) with fentanyl for subarachnoid block [21].
Intra-operative & post-operative side effects
We observed no significant differences in intra-operative or post-operative side effects among the two drug groups. In our study, all the patients were effectively pre-loaded with intravenous fluids, thus minimal incidence of nausea and vomiting with least number of cases of hypotension were reported.
Throughout our study, the overall incidence of various complications like-hypotension, bradycardia, PONV, pruritus, tinnitus was minimal and comparable in both groups, similar to the observations made by Thakore, et al. in his clinical trials [21].
Conclusion
Hence, from our study we finally come across following interpretations:
1. Both intrathecal bupivacaine and fentanyl versus levobupivacaine with fentanyl had equally good control of hemodynamic parameters during intra-operative period and post-operatively.
2. The time period taken to achieve sensory block as well as motor block was shorter in patients who received intrathecal hyperbaric formulation of bupivacaine with fentanyl in comparison to levobupivacaine with fentanyl.
3. Furthermore, total duration of sensory block and motor block was observed to be longer in patients with intrathecal administration of hyperbaric bupivacaine and fentanyl versus levobupivacaine with fentanyl.
4. Intrathecal bupivacaine with fentanyl provides better pain control with little longer time period of analgesia in comparison to intrathecally administrated levobupivacaine with fentanyl.
- Butterworth JF, Strichartz GR. Molecular mechanisms of local anaesthesia: a review. Anesthesiology. 1990;72(4):711–734. Available from: https://doi.org/10.1097/00000542-199004000-00022
- Miller RD, Eriksson LEE, Fleisher LA, Wiener KJP, Cohen NH. Miller’s anaesthesia [ebook]. 8th ed. Philadelphia: Elsevier Health Sciences; 2014. p. 1684–1721. Available from: https://evolve.elsevier.com/cs/product/9780323352192?role=student
- Kokki H. Spinal blocks. Paediatr Anaesth. 2012;22(1):56–64. Available from: https://doi.org/10.1111/j.1460-9592.2011.03693.x
- Bors E, Comarr AE, Moulton SH. The role of nerve blocks in management of traumatic cord bladders: spinal anesthesia, subarachnoid alcohol injections, pudendal nerve anesthesia and vesical neck anesthesia. J Urol. 1950;63(5):653–666. Available from: https://doi.org/10.1016/s0022-5347(17)68810-4
- McLain RF, Kalfas I, Bell GR, Tetzlaff JE, Yoon HJ, Rana M. Comparison of spinal and general anesthesia in lumbar laminectomy surgery: a case-controlled analysis of 400 patients. J Neurosurg Spine. 2005;2(1):17–22. Available from: https://doi.org/10.3171/spi.2005.2.1.0017
- Carpenter RL, Caplan RA, Brown DL, Stephenson C, Wu R. Incidence and risk factors for side effects of spinal anesthesia. Anesthesiology. 1992;76(6):906–916. Available from: https://doi.org/10.1097/00000542-199206000-00006
- Hartmann B, Junger A, Klasen J, Benson M, Jost A, Banzhaf A, et al. The incidence and risk factors for hypotension after spinal anesthesia induction: an analysis with automated data collection. Anesth Analg. 2002;94(6):1521–1529. Available from: https://doi.org/10.1097/00000539-200206000-00027
- Tarkkila PJ, Kaukinen S. Complications during spinal anesthesia: a prospective study. Reg Anesth. 1991;16(2):101–106. Available from: https://pubmed.ncbi.nlm.nih.gov/2043522/
- Kilpatrick ME, Girgis NI. Meningitis: a complication of spinal anesthesia. Anesth Analg. 1983;62(5):513–515. Available from: https://pubmed.ncbi.nlm.nih.gov/6404195/
- Horlocker TT. Complications of spinal and epidural anesthesia. Anesthesiol Clin North Am. 2000;18(2):461–485. Available from: https://doi.org/10.1016/s0889-8537(05)70172-3
- Sonawane K, Dixit H, Jayaraj A, Thota N, Sekar C. Knowing it before blocking it: the ABCD of the peripheral nerves: part A (nerve anatomy and physiology). Cureus. 2023;15(7):e41771. Available from: https://doi.org/10.7759/cureus.41771
- Paganelli MA, Popescu GK. Actions of bupivacaine, a widely used local anesthetic, on NMDA receptor responses. J Neurosci. 2015;35(2):831–842. Available from: https://doi.org/10.1523/jneurosci.3578-14.2015
- Bajwa SJ, Kaur J. Clinical profile of levobupivacaine in regional anesthesia: a systematic review. J Anaesthesiol Clin Pharmacol. 2013;29(4):530–539. Available from: https://doi.org/10.4103/0970-9185.119172
- Guler G, Cakir G, Ulgey A, Ugur F, Bicer C, Gunes I, et al. A comparison of spinal anesthesia with levobupivacaine and hyperbaric bupivacaine for cesarean sections: a randomized trial. Open J Anesthesiol. 2012;2(3):84–89. Available from: https://www.scirp.org/journal/paperinformation?paperid=20539
- Sinchana AS, Vijaykumar TK, Alalamath S. Comparative efficacy of intrathecal hyperbaric levobupivacaine with fentanyl versus hyperbaric bupivacaine with fentanyl in elective cesarean section. Cureus. 2024;16(9):e70476. Available from: https://www.cureus.com/articles/285278-comparative-efficacy-of-intrathecal-hyperbaric-levobupivacaine-with-fentanyl-versus-hyperbaric-bupivacaine-with-fentanyl-in-elective-cesarean-section#!/
- Uzun U, İdin K. Comparison of onset times and hemodynamic changes of bupivacaine and levobupivacaine used in spinal anesthesia. Anatol J Gen Med Res. 2025;35(2):116–121. Available from: https://anatolianjmed.org/pdf/13b035c5-551c-4fd4-a824-19a1febb0519/articles/anatoljmed.2025.75537/116-121.pdf
- Chatterjee S, Bisui B, Mandal A, Sheet J, Sengupta S, Majumdar S, et al. Effects of intrathecal hyperbaric ropivacaine versus hyperbaric bupivacaine for lower limb orthopedic surgery. Anesth Essays Res. 2014;8(3):349–353. Available from: https://doi.org/10.4103/0259-1162.143138
- Glaser C, Marhofer P, Zimpfer G, Heinz MT, Sitzwohl C, Kapral S, et al. Levobupivacaine versus racemic bupivacaine for spinal anesthesia. Anesth Analg. 2002;94(1):194–198. Available from: https://doi.org/10.1213/00000539-200201000-00037
- Girish BK, Srinivas HT, Reddy SM. A comparative study of hyperbaric 0.5% levobupivacaine with bupivacaine 0.5% for spinal anaesthesia in elective surgeries. Indian J Anesth Analg. 2018;5(5):2013–2020.
- Camorcia M, Capogna G, Berritta C, Columb MO. The relative potencies for motor block after intrathecal ropivacaine, levobupivacaine, and bupivacaine. Anesth Analg. 2007;104:904–907. Available from: https://doi.org/10.1213/01.ane.0000256912.54023.79
- Thakore S, Thakore N, Chatterji R, Chatterjee CS, Nanda S. Evaluating the efficacy of low-dose hyperbaric levobupivacaine (0.5%) versus hyperbaric bupivacaine (0.5%) along with fentanyl for subarachnoid block in patients undergoing medical termination of pregnancy and sterilization: a prospective, randomized study. J Obstet Anaesth Crit Care. 2018;8(2):90–95. Available from: https://journals.lww.com/joac/fulltext/2018/08020/evaluating_the_efficacy_of_low_dose_hyperbaric.6.aspx
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
