Global Journal of Anesthesiology
Airway Management of Ludwig’s Angina in a Paediatric Patient
1Professor, Department of Anaesthesia, Christian Medical College and Hospital, Ludhiana, Punjab-141008, India
2Assistant Professor, Department of Anaesthesia, Christian Medical College and Hospital, Ludhiana, Punjab-141008, India
3Resident, Department of Anaesthesia, Christian Medical College and Hospital, Ludhiana, Punjab-141008, India
Author and article information
Cite this as
Abraham V, et al. Airway Management of Ludwig’s Angina in a Paediatric Patient. Glob J Anesth. 2026; 13(1): 1-5. Available from: 10.17352/2455-3476.000061
Copyright License
© 2026 Abraham V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Diffuse cellulitis affecting the bilateral submandibular, sublingual, and submental spaces characterizes Ludwig’s angina, a quickly developing, potentially fatal soft tissue infection. It is a medical emergency due to its sudden onset and rapid spread. In this report, we describe a case of a widespread odontogenic infection that spread to the cervical region with an elevated floor of the mouth and compromised airway. The affected spaces were drained.
Case report: A 9-year-old female child with Ludwig’s angina was taken up for emergency incision and drainage. The airway management was anticipated to be difficult. Initial tracheal intubation was difficult, and an attempt at tracheostomy was made, which led to drainage of pus, but the trachea could not be identified due to inflammation. Following the drainage of pus, oral intubation was done with a smaller tube (4.5), and the airway was secured.
Conclusion: In a case of Ludwig’s angina, difficult mask ventilation due to swelling of the soft tissues, difficult laryngoscopy due to swelling and inflammation of the floor of the mouth, and difficult intubation should be anticipated by the anaesthesiologists. Hence, there should be minimal airway manipulation with a trial of intubation by an experienced anaesthesiologist and tracheostomy is considered the mainstay of airway management. In the paediatric age group, tracheostomy could be associated with tracheal stenosis; hence, endotracheal intubation is usually preferred over tracheostomy as the first line of airway management.
Hb: Hemoglobin; TLC: Total Leukocyte Count; CT: Computed Tomography, Inj: Injection
Introduction
A potentially fatal, virulent streptococcal brawny swelling is Ludwig’s angina. Anaesthetic difficulties during airway manipulation result from hemodynamic instability and restricted mouth opening [1]. About 24% - 30% of the cases that are reported involve children. Malnutrition, diabetes mellitus, dental caries, immunocompromised conditions, and poor oral hygiene are among the risk factors [2]. The Latin word “angere,” which means “strangle,” is where the word “angina” originates [3]. Wilhelm Friedrich, a German physician, first described the illness in 1836 and is credited with coining the term [4]. The clinical criteria for the diagnosis of Ludwig’s angina were proposed by Grodinsky [5]:
- Bilateral infection involving more than one compartment of the submandibular space
- Gangrenous serosanguinous infiltrate with or without pus
- Involvement of the connective tissue, fascia and muscle, but not the glandular structures
- Spread by continuity rather than by lymphatics
Anatomically, the tongue is displaced upwards and backwards, leading to painful obstruction of the airway. Swelling of the posterior aspect of the tongue pushes the equally edematous epiglottis posteriorly, leading to further narrowing of the airway [6]. It can extend into the deep fascial layers of the neck, leading to glottic edema, further leading to airway compromise. The most common site of infection is lower second and third molars, but also seen in peritonsillar or parapharyngeal abscesses, submandibular gland sialadenitis, mandibular trauma, oral neoplasia, lymphangiomas, and penetrating injuries to the floor of the mouth, like tongue piercing [2]. The fatal, life-threatening complications include glottic edema, subphrenic abscess, aspiration pneumonia, necrotizing fasciitis, and descending necrotizing mediastinitis, leading to high mortality rates [2,3].
Ludwig’s angina can be divided into: Mild – patients aged <40 years without respiratory distress. Moderately severe patients aged <40 years with symptoms of respiratory distress; those aged between 40-60 years with or without respiratory symptoms; and those aged >60 years without respiratory distress. Severe patients aged >60 years with respiratory distress and associated co-morbidities [7].
Odontogenic infections commonly involve a mixed microbial flora [2]. Airway management is the main goal of treatment. Securing the airway either with endotracheal intubation (if possible), tracheostomy, or cricothyroidotomy is necessary as per the expertise and judgement of the treating physician. Traditionally, tracheostomy was regarded as the definitive method for securing the airway. Elective awake tracheostomy was often advocated in cases of deep neck space infections to circumvent the risks associated with performing an emergency tracheostomy in the presence of a critically compromised airway [7]. Treatment starts with broad-spectrum antibiotics with immediate surgical drainage, which involves wide decompression and drainage of the suprahyoid spaces to protect the airway [6]. A trained multidisciplinary team is required for the management of Ludwig’s angina [7].
Case presentation
A 9-year-old female child, weighing 29 kg, presented to the dental department with complaints of a left molar infected tooth for 2 weeks, associated with fever for 5 days. For the first week, she was managed elsewhere with analgesics, and her swelling had resolved. Then she developed pain, which was sharp and non-radiating in nature, and swelling on both sides of the lower jaw with restricted mouth opening and difficulty in taking oral intake (solids followed by clear fluids). There was no history of breathlessness or dyspnea on exertion. She was initially admitted to one of the outside hospitals during the second week of her symptoms, for 2 days and received IV antibiotics, IV analgesics, and IV fluids. Later, she was discharged. As the swelling was increasing with mild stridor, she was brought to our hospital during the third week of her symptoms.
On examination, she was conscious, oriented, and anxious, with a heart rate of 172/min, stable blood pressure, and a saturation of 96% on room air. She had a fever of 102°F. There was a 4 x 2 cm swelling on the bilateral submandibular region, submental region, and both sides of the cheek, with overlying skin mildly erythematous. The mouth opening was approximately 2 finger breaths. There was total restriction of flexion and extension of the neck. Hb was 9.9 g/dL, and TLC was 27700 cells/mcgL.
A diagnosis of Ludwig’s angina was made, and after giving Inj. Paracetamol, she was taken for emergency drainage of pus. In the theatre, monitors were attached. Heart rate, blood pressure, and saturation were noted and were within normal limits. She was preoxygenated with 100% oxygen. Inj. Ketamine 20 mg was given slowly intravenously with oxygen and sevoflurane. Mask holding was difficult, as the angle of the jaw was obliterated, and the soft tissue was hard due to pus collection. As we were able to ventilate the patient with adequate chest rise, Inj. Scoline 50 mg was given intravenously, as scoline is a short-acting muscle relaxant. Ideally, the patient should be deepened with inhalational anaesthetic agents. Laryngoscopy was difficult, as the tongue was swollen and was like a ball in shape. The epiglottis was flattened and pushed to one side. So immediately the laryngoscope was withdrawn, and mask ventilation was started. Ventilation was difficult, and she developed stridor. We tried to insert an oral airway, but stridor increased. She started breathing spontaneously, so a nasal airway was slowly inserted, but she started bleeding from the nose. Oxygen and sevoflurane were given through the nasal airway, and the nostril was pressed with a gauze piece. A small laryngoscope blade (blade number 2) was slowly inserted into the mouth, and the tongue was depressed to prevent the obstruction. Adrenaline was diluted to 1:10,000, and 4 drops were introduced into the nostril every 4 to 5 minutes for three times to prevent bleeding and laryngeal edema.
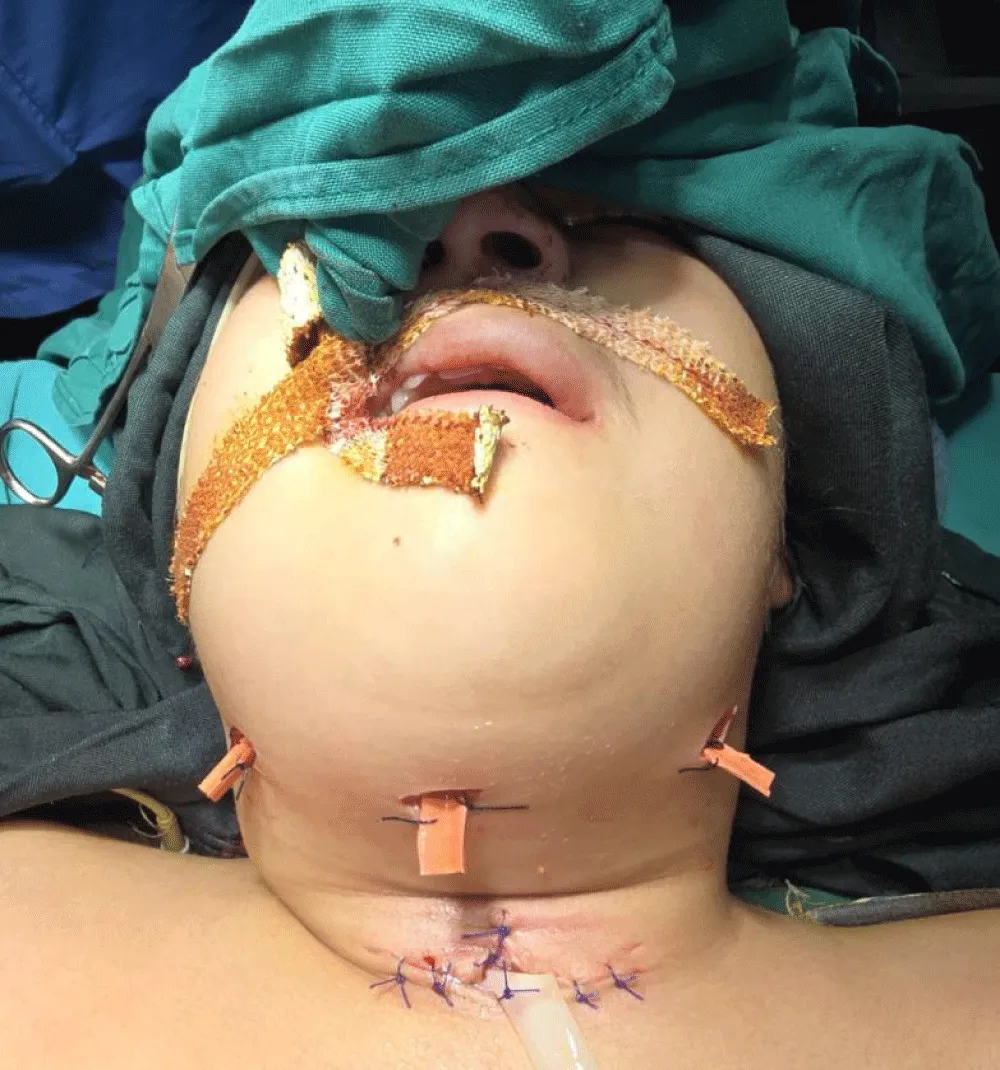
Saturation was maintained around 80%, and the pediatric surgery team was called for emergency tracheostomy. An 18-gauge needle was introduced after feeling the trachea, and pus came out through the needle. A small horizontal incision was made, from which a gush of pus was drained. About 80 cc of pus was drained from the anterior neck space. Further exploration was done, and the trachea and esophagus were inflamed but could not be identified, so laryngoscopy was attempted again—the tip of the epiglottis was viewed, and an uncuffed endotracheal tube of size 4.5 was inserted blindly after seeing the bubble below the tip of the epiglottis, following which the airway was secured. Saturation had increased to 100%. She was kept on spontaneous respiration for the rest of the surgery with intermittent low doses of ketamine (5 mg) and sevoflurane with oxygen. Intraoperatively, 50 cc of pus was drained from the right submandibular space and 3 cc from the submental space, and a corrugated rubber drain was placed. Postoperatively, the patient was shifted to the ICU with stable vitals, unextubated, for further management. On post-op day 1, she was managed with sedation on pressure support mode. IV antibiotics, chest physiotherapy, and nebulizations were continued for another 3 days. She was extubated on the 3rd postoperative day. Her vitals were stable, awake, and she was breathing adequately. She was shifted to the ward, and she was discharged the next day in a stable condition (Figure 1).
Discussion
Ludwig’s angina is a potentially life-threatening diffuse gangrenous cellulitis affecting the floor of the mouth, extending to the anterior neck spaces—submandibular by penetration of the thin inner cortex of the mandible and submental spaces via connective tissue, muscle, and fascial planes rather than via the lymphatic system [4]. Ludwig’s angina affects a wide age range, from day 1 to more than 50 years old. According to Okoji’s study, it typically affected a mean age of 47.7 years [8].
The patients usually present with fever, malaise, and fatigue, with a painful woody brawny swelling in the submandibular, sublingual, and submental regions. Our patient on presentation was anxious with fever, dysphagia, fatigue, and drooling of saliva, with signs of respiratory distress like stridor. Logistic regression analysis has identified the presence of co-morbidities and bilateral submandibular swelling as significant predictors of mortality in patients with Ludwig’s angina. According to the article by Singh H, et al. our patient can be categorized under mild Ludwig’s angina, her age being 9 years, with no systemic illness [7,9].
From the study of Braimah, et al. (2016), 89.3% of the patients survived, while 3% perished. A study by Yusuf Fakir, et al. (2008) showed that 88% of the patients did not require an artificial airway, with a mean admission of 14 [10]. In our case, she presented after 2 weeks of dental infection with progressively increasing swelling in the submandibular region. In view of the anticipated involvement of the floor of the mouth with impending respiratory distress, she was taken up for emergency incision and drainage of the same with an anticipated difficult airway. All the necessary precautions and equipment for difficult mask holding and difficult intubation were taken, along with the execution of the intubation by a skilled and experienced anaesthesiologist as demanded by the situation. The theatre was prepared with an appropriately sized paediatric mask, smaller-sized endotracheal tubes, a video laryngoscope, a bougie, adequately working suction with Mapleson F, and an oral and nasal airway.
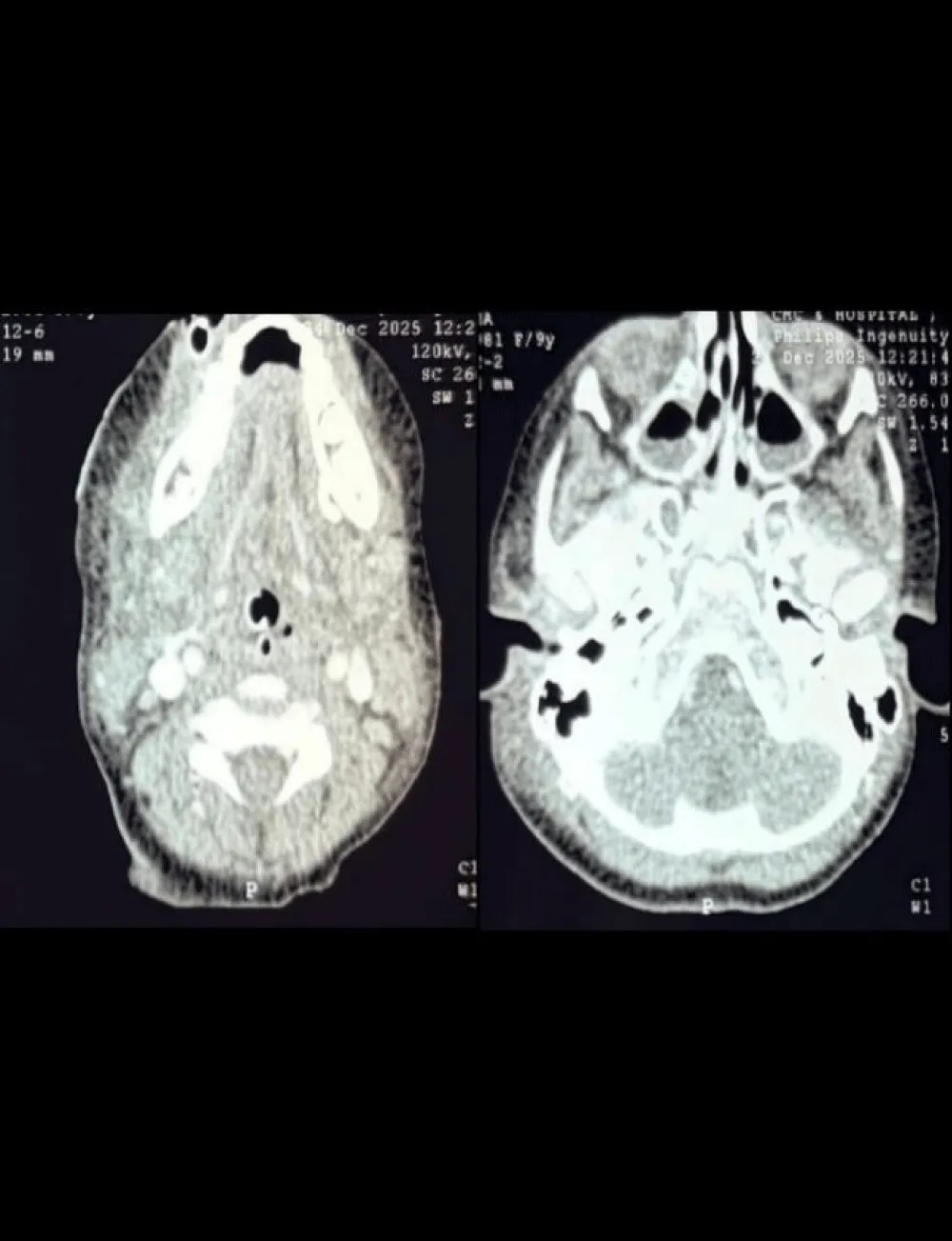
CT scanning is highly effective in evaluating deep neck spaces and mediastinal abscesses. Although MRI provides superior soft tissue resolution, its longer acquisition time limits its utility in acute settings; CT is the imaging modality of choice [7,11]. In our case, the patient had no comorbidities, and her recovery from the illness was hastened after the surgical decompression and broad-spectrum intravenous antibiotics. Contrast CT imaging of the neck was done, which illustrated ill-defined collections involving the floor of the mouth, right parotid space, bilateral submandibular space, right masticator space, anterior cervical space on the left side, and right parapharyngeal space. Inferiorly extending to the visceral space of the neck at the T1/T2 intervertebral disc level (Figures 2,3).
According to a study conducted by Fellini RT, et al. in a case report of Airway management in Ludwig’s angina: a challenge, finalized with a report of a failed attempt of oral and nasal intubation, following which a flexible fiberoptic laryngoscope was tried [12]. In view of a failed flexible fiberoptic laryngoscopy, emergency tracheostomy was done. Spitalnic and Sucov reported a case of Ludwig’s angina in which a flexible fiberoptic laryngoscope failed, and finally a tracheostomy was done [13]. In our patients, different modalities of airway management were used—initially intubation with the availability of videolaryngoscope and bougie, followed by oral and nasal airway. We gave a short-acting muscle relaxant, succinylcholine, as we could ventilate. We can also deepen the patient with sevoflurane. Then a small laryngoscope blade was used to depress the tongue. In view of the failed attempt to secure the airway by the above modalities, cricothyroidotomy was tried, but pus was drained from the site. Tracheostomy was attempted, but due to inflammation and pus, the trachea could not be identified. Finally, blind endotracheal intubation was done to secure the airway.
Airway management using broad-spectrum antibiotics that cover gram-positive, gram-negative, and anaerobic coverage forms the basis of treatment for these patients. Before and after airway manipulation, soft tissue swelling, facial edema, and airway edema can be reduced with intravenous steroids, the preferred steroid being dexamethasone [4]. Airway blockage is lessened by nebulized epinephrine (1 millilitre of 1:1000 diluted to 5 millilitres of 0.9% saline) [11]. In our patients, steroids were given pre-induction in view of anticipated airway and glottic edema. Diluted adrenaline was given 4-5 drops every 5 min for 15 minutes to control bleeding from the inflamed mucosa. Intermittent puffs of Duolin and Budecort were also given to relieve the airway hyperactivity after the first laryngoscopy attempt.
Mask ventilation is often difficult due to neck swelling and obliteration of the angle of the mouth. In our patient, difficult mask ventilation was anticipated, but adequate preoxygenation was done before the trial of intubation. Blind oral and nasotracheal intubation and supraglottic airway devices are discouraged because of the risk of airway trauma, worsening edema and failed placement. Awake fiberoptic nasotracheal intubation is the preferred technique, with readiness for emergency surgical airway. In advanced and late stages, cricothyrotomy or tracheostomy is indicated [11]. In this case, after the first attempt at laryngoscopy, further attempts were not tried after the initial view of the difficult airway. The second attempt was taken only after the failed attempt at tracheostomy, and about 100 cc of pus was drained in anticipation of the relative relief of pressure from the anterior neck spaces on the larynx. Multiple laryngoscopies were avoided to avoid airway trauma in view of the inflamed mucosa. The video laryngoscope also showed distorted anatomy due to edema and inflammation. Endotracheal intubation was done blindly with a small uncuffed endotracheal tube (number 4.5) only after viewing the tip of the epiglottis. The patient was breathing spontaneously throughout the procedure with a low dose of sedation and sevoflurane.
In our case, we would like to emphasize the proper positioning of the child during mask holding with avoidance of long-acting muscle relaxants after the view of the first laryngoscopy. We allowed the patient to breathe spontaneously throughout the surgery. A small laryngoscope blade (number 2) was used to push the tongue downwards and toward one side to relieve airway obstruction. The nasal airway was placed till the airway was secured, and volatile anaesthetic agents were given through the nasal airway. In view of a failed tracheostomy attempt, a second laryngoscopy was tried after about 100 cc of pus was drained. The tip of the epiglottis was viewed, and the patient was intubated with a small uncuffed endotracheal tube; soon, 100% saturation was attained. Postoperatively, the patient was shifted to the ICU and was kept intubated for 3 days for the swelling to subside with IV antibiotics and nebulizations.
The strength of this study was the efficient management of the compromised airway by a team of experienced anaesthesiologists, which was needed for further resuscitation of the patient.
Conclusion
Ludwig’s angina can be life-threatening, and we should anticipate difficult intubation. An experienced anaesthesiologist should be available to manage these cases. A muscle relaxant should be administered only if you are 100% sure of mask ventilation. A difficult intubation cart trolley should be available.
Acknowledgment
All the authors declare that they have: Substantial contributions to the conception or design of the work, or the acquisition, analysis, or interpretation of data for the work, AND drafting the work or revising it critically for important intellectual content AND final approval of the version to be published AND agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. We would like to thank the Department of Anaesthesia, Christian Medical College, for the institutional support. We certify that Dr Elzeba Susan Varghese will correspond on behalf of all the authors with the editorial board. We also grant him the right to carry out the necessary changes as per the recommendations of the journal and act as a guarantor for the manuscript on our behalf. We also certify that no external funding/grants were received.
- Dr. Valsa Abraham
- Dr Narjeet K Osahan
- Dr Himani garg
- Dr Elzeba Susan Varghese
- Dr Harman
- Jamil S, Turki S, Singh P. Anesthetic challenges in a patient of atypical Ludwig’s angina. Indian J Clin Anaesth. 2024;11(1):118-119. Available from: http://doi.org/10.18231/j.ijca.2024.025
- Quetzal MR, Soler González J. Ludwig’s angina: case presentation. Belize J Med. 2023;12(1):28-31. Available from: https://doi.org/10.61997/bjm.v12i1.289
- Ahmed YJ, Younis AG, Tawfeeq BA, Al-Rawee RY. Clinical survey for Ludwig’s angina cases presented in the emergency department of Al-Salam Teaching Hospital. Surg Res. 2024;6(4):1-6. Available from: https://www.scivisionpub.com/pdfs/clinical-survey-for-ludwigs-angina-cases-presented-in-the-emergency-department-of-alsalam-teaching-hospital-3375.pdf
- Kamala KA, Sankethguddad S, Sujith SG. Ludwig’s angina: emergency treatment. J Health Sci Res. 2017;8(1):46-48. Available from: http://doi.org/10.5005/jp-journals-10042-1048
- Al Jabery A, Al Kaabi S, Al Kaabi A, Al Tatari H. Group B Streptococcus infection presenting as Ludwig’s angina beyond infancy. Pediatr Infect Dis. 2017;2(3). Available from: https://doi.org/10.21767/2573-0282.100039
- Kshirsagar RA, Banerjee P, Bhende R, Singh V. Ludwig’s angina – a brawny cellulitis: a case report. Int J Curr Res. 2019;11(4):3034-3037. Available from: https://www.journalcra.com/article/ludwig%E2%80%99s-angina-%E2%80%93-brawny-cellulitis-case-report
- Singh H, Singh R, Goyal G, Dhillon V, Arora V, Sarkar A. Ludwig’s angina: analysis of clinical features and their management strategy: a study of 30 patients. Int J Otorhinolaryngol Head Neck Surg. 2020;6(10):1830-1836. Available from: http://doi.org/10.18203/issn.2454-5929.ijohns20204184
- Okoje VN, Ambeke OO, Gbolahan OO. Ludwig’s angina: an analysis of cases seen at the University College Hospital, Ibadan. Ann Ibd Pg Med. 2018;16(1):61-68. Available from: https://pubmed.ncbi.nlm.nih.gov/30254560/
- Pandey M, Kaur M, Sanwal M, Jain A, Sinha SK. Ludwig’s angina in children: an anesthesiologist’s nightmare—case series and review of literature. J Anaesthesiol Clin Pharmacol. 2017;33(3):406-409. Available from: https://doi.org/10.4103/0970-9185.214318
- Shaikh NH, Shaik Kareemulla N. Ludwig's angina: a systematic review. Int J Enhance Res Med Dent Care. 2022;9(11):38-44. Available from: https://www.erpublications.com/uploaded_files/download/dr-shaik-nida-hafsa-dr-nehla-shaik-kareemulla_UJgIH.pdf
- Vasanth S, Chandran S, Pandyan DA, Gnanam P, Djeramane S, Wong LS, et al. Case report: Ludwig’s angina – the danderous space. F1000Research. 2022;11:1511. Available from: https://doi.org/10.12688/f1000research.127242.2
- Fellini RT, Volquind D. Airway management in Ludwig’s angina – a challenge: case report. Braz J Anesthesiol. 2017;67(6):637-640. Available from: https://doi.org/10.1016/j.bjan.2014.10.004
- Spitalnic SJ, Sucov A. Ludwig's angina: case report and review. J Emerg Med. 1995;13(4):499-503. Available from: https://doi.org/10.1016/0736-4679(95)80007-7
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
