Archives of Clinical Gastroenterology
Perianal paget’s disease: A case report
1Gastroenterology Department, University Hospital Virgen Macarena, Seville, Spain
2Anatomical Pathology Department, University Hospital Virgen Macarena, Seville, Spain
3Galera Anatomical Pathology Centre, Seville, Spain
4University of Seville, Spain
Author and article information
Cite this as
Hernández PN, Delgado TV, Aguado JM, González-Cámpora R, Arias FA (2022) Perianal paget’s disease: A case report. Arch Clin Gastroenterol. 2022; 8(3): 50-51. Available from: 10.17352/2455-2283.000112
Copyright License
© 2022 Hernández PN, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The incidence of extramammary Paget’s disease (EMPD) is very low. It is very important to distinguish between primary Paget’s disease and secondary process. An 85-year-old man was consulted for the presence of an erythematous plaque located in the anal and gluteal area, confirming Paget cells in the biopsy.
Perianal Paget’s disease (PPD), a subset of extramammary Paget’s disease, is a rare cutaneous neoplasm that is often misdiagnosed and undertreated. Its incidence accounts for less than 1% of perianal disease and 1.3% of Paget’s disease cases.
Case report
We present the case of an 85-year-old man diagnosed 20 years ago with ulcerative colitis (UC) that received maintenance treatment with oral mesalazine 3g/24h and correct control of his disease. The last colonoscopy was performed in 2017 and the biopsies were compatible with minimal inflammatory changes, ruling out dysplastic changes.
In 2019 he lost to follow-up due to the COVID-19 pandemic. Two years later he consulted for anal itching and pain, which he initially attributed to his UC and sometimes improved with topical ointments.
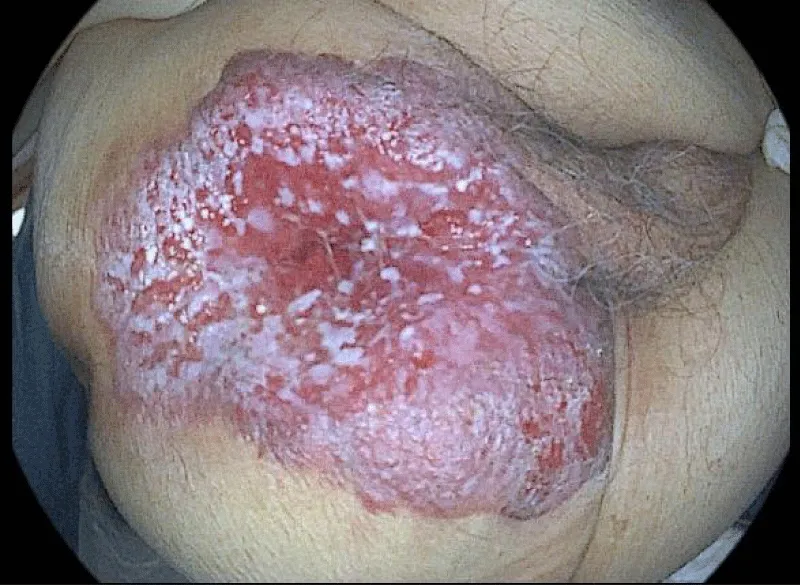
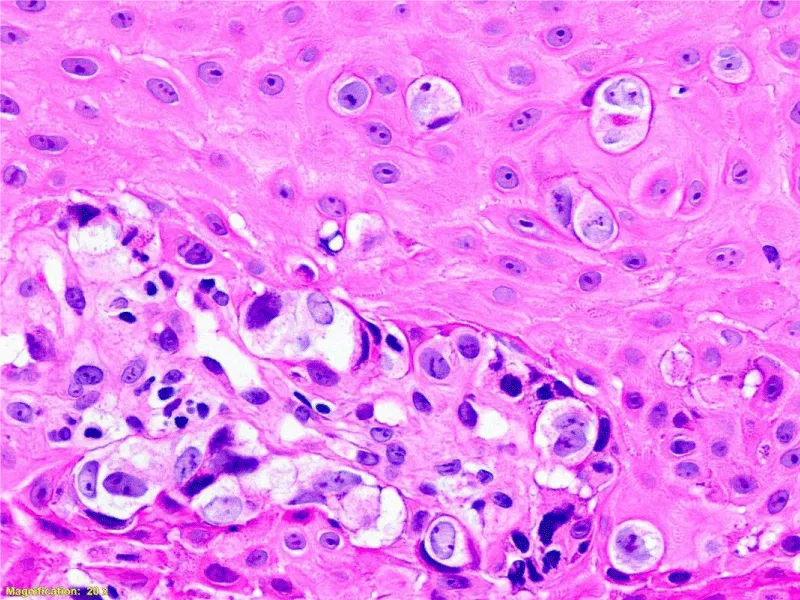
Physical examination revealed a hard, erythematous plaque with raised edges, about 10cm in diameter, in the perianal area (Figure 1). After the biopsy, a primary PPD was diagnosed (Figures 2,3). Colonoscopy and thoraco-abdominal CT scan were normal. Due to the invasive nature of the lesion and the age of the patient, treatment with radiotherapy was decided. Nevertheless, nine months later the patient died due to the dissemination of the disease.
Discussion
PPD is classified as Primary PPD if the tumor arises from the intraepidermal cells themselves and secondary PPD, when the primitive cancer is usually occult in adjacent organs, mainly digestive or genitourinary [1].
Although clinical suspicion and biopsy are usually the basis for diagnosis, distinguishing between primary and secondary disease is essential to make a correct evaluation, provide an accurate treatment plan and predict survival.
It occurs most frequently in women between 60-70 years of age with the formation of erythematous, hard, well-demarcated, pruritic and sometimes painful plaques or macules [2].
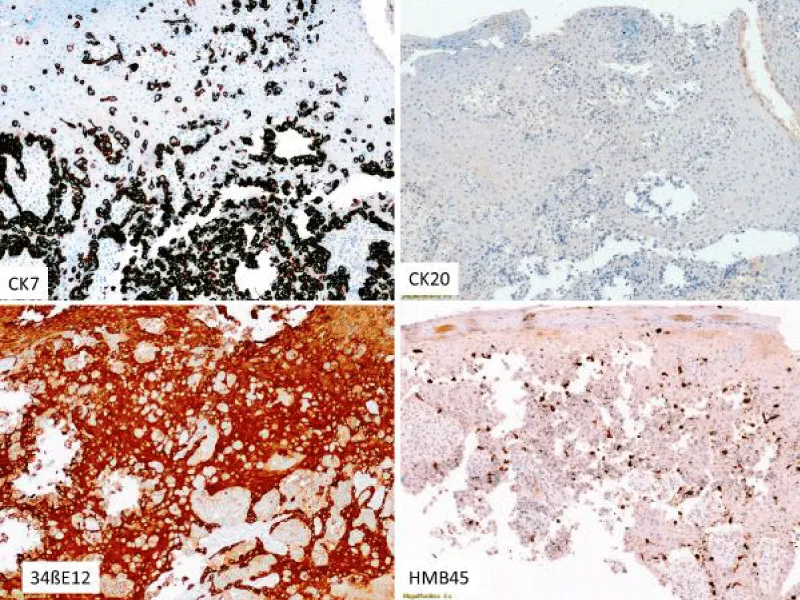
Immunohistochemical findings allow us to differentiate between primary and secondary PPD. Typically primary extramammary PD is positive for CK7 and 34ßE12 and negative for other markers such as HMB45, CK20 and CDX2 [3].
Primary PPD has a better prognosis when it is intraepithelial, but it can progress to invasive disease with metastasis.
From a therapeutic point of view, there is currently no established protocol, so the choice of therapy will depend on the type (primary or secondary), involvement and clinical experience. In cases of secondary PPD, management will be directed towards the associated carcinoma.
When the disease is localized, surgical resection is the treatment of choice [4]. Although no clinical trials are available to compare surgery versus radiotherapy, radiotherapy may be considered in selected cases as an effective alternative to surgery. Radiotherapy and/or chemotherapy are generally chosen for metastatic disease, although they can be used as neoadjuvant or adjuvant therapy [5]. Whether early or advanced stage, recurrence is common and therefore long-term follow-up is essential.
Whether it is an early or advanced stage, recurrence is frequent and therefore, long-term follow-up is essential.
Conclusions
There are no cases described in the literature that establishes a relationship between ulcerative colitis and PPD. We don´t know, therefore, whether the presence of inflammatory bowel disease or its activity could be related to a carcinogenic stimulus [6] that pathophysiologically triggers PPD. More cases and more studies would be needed to corroborate this hypothesis.
- Thompson HM, Kim JK. Perianal Paget's Disease. Dis Colon Rectum. 2021 May;64(5):511-515. doi: 10.1097/DCR.0000000000002000. PMID: 33661234; PMCID: PMC8336900.
- Ito T, Kaku-Ito Y, Furue M. The diagnosis and management of extramammary Paget's disease. Expert Rev Anticancer Ther. 2018 Jun;18(6):543-553. doi: 10.1080/14737140.2018.1457955. Epub 2018 Mar 27. PMID: 29575944.
- Hikita T, Ohtsuki Y, Maeda T, Furihata M. Immunohistochemical and fluorescence in situ hybridization studies on noninvasive and invasive extramammary Paget's disease. Int J Surg Pathol. 2012 Oct;20(5):441-8. doi: 10.1177/1066896912444159. PMID: 23001873.
- Ito T, Kaku-Ito Y, Furue M. The diagnosis and management of extramammary Paget's disease. Expert Rev Anticancer Ther. 2018 Jun;18(6):543-553. doi: 10.1080/14737140.2018.1457955. Epub 2018 Mar 27. PMID: 29575944.
- Kim CW, Kim YH, Cho MS, Min BS, Baik SH, Kim NK. Perianal Paget's Disease. Ann Coloproctol. 2014 Oct;30(5):241-4. doi: 10.3393/ac.2014.30.5.241. Epub 2014 Oct 28. PMID: 25360433; PMCID: PMC4213942.
- Yao D, Dong M, Dai C, Wu S. Inflammation and Inflammatory Cytokine Contribute to the Initiation and Development of Ulcerative Colitis and Its Associated Cancer. Inflamm Bowel Dis. 2019 Sep 18;25(10):1595-1602. doi: 10.1093/ibd/izz149. PMID: 31287863.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
