Archives of Clinical Gastroenterology
Successful Treatment of Stomal Variceal Bleeding with Percutaneous Injection Sclerotherapy
Department of Gastroenterology, Sapporo Kosei General Hospital, Sapporo, Japan
Author and article information
Cite this as
Sato T, Kimura M, Yamaguchi M, Ohmura T (2015) Successful Treatment of Stomal Variceal Bleeding with Percutaneous Injection Sclerotherapy. Arch Clin Gastroenterol. 2015; 1(1): 17-19. Available from: 10.17352/2455-2283.000005
Copyright License
© 2015 Sato T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Bleeding from ectopic varices is often massive and fatal with portal hypertension, and stomal varices can occur in patients with stoma. We aimed to treat a hepatitis B surface antigen positive 69 year-old male with liver cirrhosis associated hepatocellular carcinoma with bleeding stomal varices using percutaneous injection sclerotherapy. Percutaneous injection sclerotherapy was performed under fluoroscopy using 5% ethanolamine oleate with iopamidol (EOI) with a 25 gauge disposable injection needle; 5ml of 5% EOI were injected gradually. Injection sclerotherapy controlled acute bleeding in this patient without serious complication. The patient experienced no further episodes of bleeding during the 8 months following treatment with percutaneous injection sclerotherapy. In conclusion, percutaneous injection sclerotherapy remains an option for the treatment of patients with bleeding stomal varices.
Portal hypertension can result in the reopening of collapsed embryonic channels within existing adult veins [1]. Ectopic varices are defined by portosystemic venous collaterals occurring anywhere in the gastrointestinal tract other than the esophagogastric region. Therapeutic options for bleeding stomal varices include surgical ligation, stoma revision, portosystemic shunt, and liver transplantation. We present a case with bleeding stomal varices which were successfully treated by percutaneous injection sclerotherapy.
Case Report
A 69-year-old man with hepatitis B virus surface antigen-positive liver cirrhosis was admitted to our hospital in November 2014 with severe stomal hemorrhage. He had been diagnosed with hepatocellular carcinoma at 50 years of age, based on imaging studies, and underwent hepatic resection. He was diagnosed with liver cirrhosis during that surgery. The patient had undergone Miles' operation for rectal carcinoma at 65 years of age. At 69 years of age, he received radiation for recurrent rectal carcinoma. After the rectal surgery, the patient developed several stomal bleeding episodes over a 2 year period. Local relief of pressure to the stoma site had been performed but with a transient effect.
On admission, he had anemic conjunctivae. His blood pressure was 109/65 mmHg, pulse 72/min and regular, and body temperature 35.8°C. The laboratory findings were: red blood cells 286x104/mm3 (normal: 353-466x104/mm3), hemoglobin 5.9 g/dL (10.6-14.4 g/dL), white blood cells 6300/mm3 (3000-7800/mm3), platelets 10.8x104/mm3 (13.8-30.9x104/mm3), serum albumin 3.3 g/mL (4.0-5.2 g/mL), total bilirubin (T.Bil) 0.8 mg/mL (0.2-1.2 mg/mL), glutamic oxaloacetic transaminase (GOT) 34 IU/L (8-38 IU/L), glutamic pyruvic transaminase (GPT) 31 IU/L (4-44 IU/L), alkaline phosphatase (ALP) 262 IU/L (104-338 IU/L), blood urea nitrogen (BUN) 16.7 mg/dL (7.0-24.0 mg/dL), creatine (Cr) 0.9 mg/dL (0.4-0.9 mg/dL). The prothrombin time was 58% (90-140%).
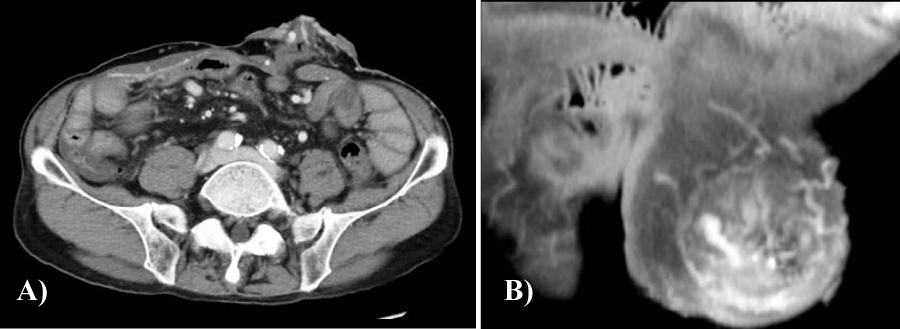
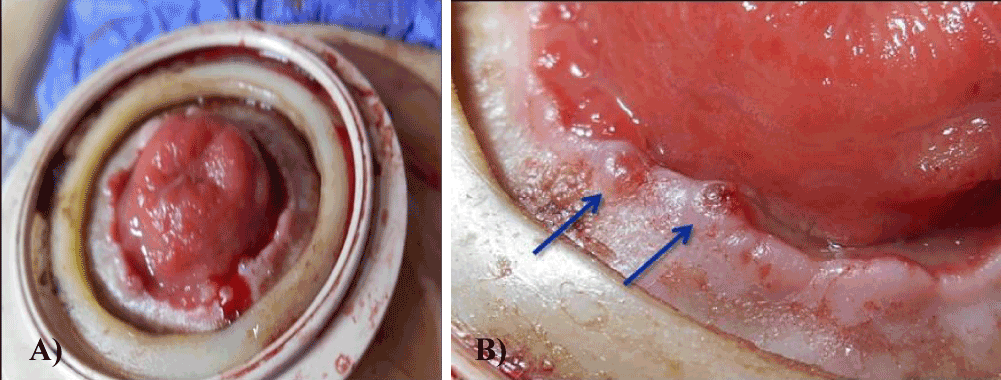
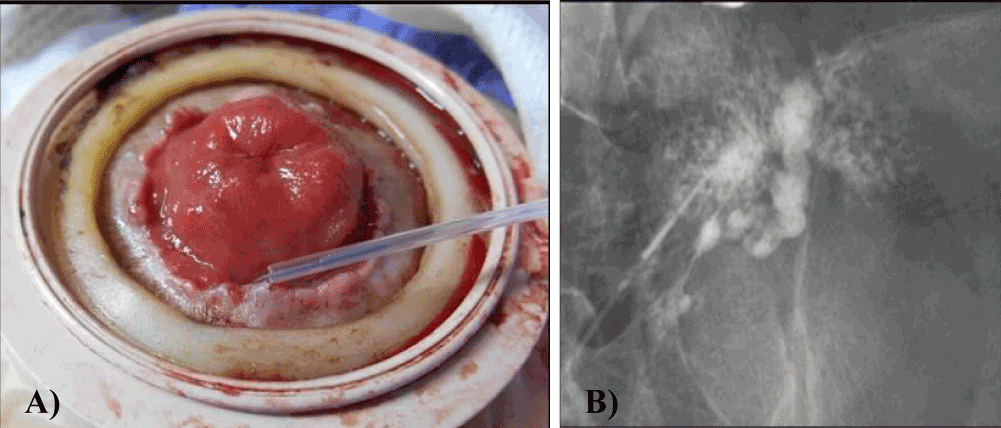
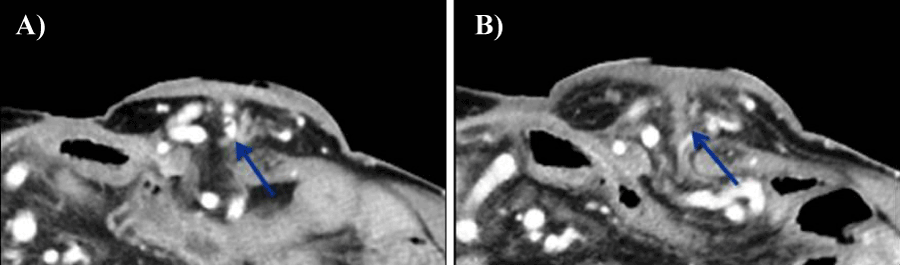
Multidetector helical computed tomography (MDCT) demonstrated stomal varices in the abdominal wall around the stoma (Figures 1a,b) and thrombosis of the portal vein. Colonoscopy through the stoma did not reveal any other active bleeding point. During an episode of active bleeding, we identified the active bleeding point in the peristomal skin (Figures 2a,b). Immediately after the diagnosis, percutaneous injection sclerotherapy was performed using 5% ethanolamine oleate with iopamidol (EOI) with a 25 gauge disposable injection needle (Top Co., Tokyo, Japan) (Figure 3a). Injection sclerotherapy was performed under fluoroscopy and 5 ml 5% EOI were injected gradually (Figure 3b). The bleeding site was effectively treated using injection sclerotherapy. The patient's daily activity improved and he was doing well after treatment. The postoperative biochemical indicators such as hepatic, renal function remained unchanged. Following treatment, MDCT revealed improvement of the stomal varices (Figures 4a,b). The patient experienced no further episodes of bleeding during the 8 months following treatment with percutaneous injection sclerotherapy.
Discussion
Stomal varices are rare in patients with portal hypertension. We present a case of stomal varices and portal hypertension with successful treatment by percutaneous injection sclerotherapy. Ectopic varices have been reported to occur at numerous sites, including 18% in the jejunum or ileum, 17% in the duodenum, 14% in the colon, 8% in the rectum, and 9% in the peritoneum [2].
Stomal varices are a rare condition of stomal bleeding. This can occur in patients with surgically created stoma with portal hypertension. The hemorrhage is recurrent and potentially fatal [3]. Massive bleeding from stomal varices occurs rarely but several articles have reported a mortality rate from stomal variceal hemorrhage ranging from 3% to 4% [3]-[5]. Stomal varices may occur with variceal erosion or trauma of the peristomal skin.
Various medical treatments, such as interventional radiology and surgery have been used to control bleeding from stomal varices; however, there is no best treatment strategy for stomal varices. Surgical portosystemic shunting leads to a reduction in portal pressure [6], however, this also may lead to significant morbidity and mortality. Local relief of pressure to the stoma site is not effective for the control of recurrent hemorrhage [6]. In patients with a poor condition, interventional radiologic techniques, such as transjugular intrahepatic portosystemic shunts (TIPS), percutaneous transhepatic obliteration (PTO) and balloon-occluded retrograde transvenous obliteration (B-RTO) have been used successfully for stomal variceal bleeding as a non-surgical option. PTO for stomal variceal bleeding also has been performed successfully [7]-[11]. The potential complications of PTO include bile leakage, bleeding, liver trauma, and portal vein thrombosis. Although B-RTO is a new interventional modality for gastric fundic varices [12], a definitive treatment for bleeding stomal varices has not been established. Minami et al. first performed successfully B-RTO using 5% ethanolamine oleate with iopamidol (5% EOI) for recurrent hemorrhaging stomal varices [13]. B-RTO is also practical for treating stomal varices and also may be used for patients in a serious condition. On the other hand, TIPS is an effective alternative for hemorrhaging stomal varices [4,14],[15]. TIPS is a relatively safe and effective means of decompressing the portal pressure but has certain limitations in patients with severe liver atrophy and complications such as encephalopathy and cerebral embolization.
Injection sclerotherapy is effective in controlling acute stomal variceal hemorrhage [14]. Several reports have revealed the usefulness and problems of injection sclerotherapy as a treatment of stomal varices [4,5],[16]-[20]. In our case, percutaneous injection sclerotherapy was performed under fluoroscopy using 5% EOI, without complication. This harsh chemical agent acts by denaturing biologic tissue, bringing about complete endothelial destruction and fibrosis following injection into a vein [21]. The sclerosant should be injected slowly, taking care to ensure that the agent does not flow into the systemic circulation during treatment and avoiding stomal damage due to para-variceal injection. The para-variceal injection of 5% EOI carries a variable risk of peristomal ulceration, stricture, and necrosis. In this emergency case, percutaneous injection sclerotherapy was chosen as a non-invasive and effective treatment. The optimal treatment of stomal variceal bleeding in patients with portal hypertension has not been established. Percutaneous injection sclerotherapy is safe and non-invasive and can be carried out in patients in poor condition. This method should be taken into consideration.
Conclusion
Percutaneous injection sclerotherapy was very useful for stomal variceal bleeding in this liver cirrhotic patient. However, 8 months follow-up was not sufficient and this may be a limitation of this report.
Acknowledgement
We thank DR Ito for investigation of total colonoscopy.
- Walsh G, Williams MP (1995) Case report: Giant pararectal varices-computed tomographic appearances. Br J Radiol 68: 203-204.
- Lebrec D, Benhamou JP (1985) Ectopic varices in portal hypertension. Clin Gastroenterol 14: 105-121.
- Handschin AE, Weber M, Weishaupt D, Fried M, Clavien PA (2002) Contrast-enhanced three-dimensional magnetic resonance angiography for visualization of ectopic varices. Dis Colon Rectum 45: 1541-1544.
- Ryu RK, Nemcek AA Jr, Chrisman HB, Saker MB, Blei A, et al. (2000) Treatment of stomal variceal hemorrhage with TIPS : case report and review of the literature. Cardiovasc Intervent Radiol 23: 301-303.
- Johnson PA, Laurin J (1997) Transjugular portosystemic shunt for treatment of bleeding stomal varices. Dig Dis Sci 432: 440-442.
- Conte JV, Arcomano TA, Naficy MA, Holt RW (1990) Treatment of bleeding stomal varices. Report of a case and review of the literature. Dis Colon Rectum 33: 308-314.
- Kishimoto K, Hara A, Arita T, Tsukamoto K, Matsui N, et al. (1999) Stomal varices: treatment by percutaneous transhepatic coil embolization. Cardiovasc Intervent Radiol 22: 523-525 .
- Naidu SG, Castle EP, Kriegshauser JS, Huettl EA (2010) Direct percutaneous embolization of bleeding stomal varices. Cardiovasc Intervent Radiol 33: 201-204.
- Arulraj R, Mangat KS, Tripathi D (2011) Embolization of bleeding stomal varices by direct percutaneous approach. Cardiovasc Intervent Radiol 34: 210-213.
- Theophilidou E, Waraich N, Raza T, Agarwal PK (2012) Liver metastases, a rare cause of portal hypertension and stoma bleeding. Brief review of literature. Int J Surg Case Rep 3: 173-176.
- Wang L, Zhou JL, Yang N, Zhang GN, Lu JY, et al. (2015) Ectopic variceal bleeding from colonic stoma: two case reports. Medicine 94: e406.
- Kanagawa H, Mima S, Kouyama H, Gotoh K, Uchida T, et al. (1996) Treatment of gastric fundal varices by balloon-occluded retrograde transvenous obliteration. Gastroenterol Hepatol 11: 51-58.
- Minami S, Okada K, Matsuo M, Kamohara Y, Sakamoto I, et al. (2007) Treatment of bleeding stomal varices by balloon-occluded retrograde transvenous obliteration. J Gastroenterol 42: 91-95.
- Minami S, Okada K, Matsuo M, Kamohara Y, Sakamoto I, et al. (1995) Bleeding stomal varices: treatment with a transjugular intrahepatic portosystemic shunt in two pediatric patients. J Vasc Interv Radiol 6: 233-236.
- Morris CS, Najarian KE (2000) Transjugular intrahepatic portosystemic shunt for bleeding stomal varices associated with chronic portal vein occlusion: long-term angiographic, hemodynamic, and clinical follow-up. Am J Gastroenterol 95: 2966-2968.
- Wolfsen HC, Kozarek RA, Bredfeldt JE, Fenster LF, Brubacher LL (1990) The role of endoscopic injection sclerotherapy in the management of bleeding peristomal varices. Gastrointest Endosc 36: 472-474.
- Thompson J (1993) Caput medusae: peristomal varices. J ET Nurs 20: 216-219.
- Mosquera DA, Walker SJ, McFarland JB (1998) Bleeding stomal varices treated by sclerotherapy. J R Coll Surg Edinb 33: 337.
- Morgan TR, Feldshon SD, Tripp MR (1986) Recurrent stomal variceal bleeding. Successful treatment using injection sclerotherapy. Dis Colon Rectum 29: 269-270.
- Tan ST (2014) Sclerotherapy for rare bleeding stomal varices after ileal conduit urinary diversion: an effective and noninvasive method. Scott Med J 59: e5-7.
- Duffy DM (2010) Sclerosants: a comparative review. Dermatol Surg 2: 1010-1025.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
