International Journal of Vascular Surgery and Medicine
Management of serious arterial injuries of the limbs
1Cardiovascular Surgery Department, Gafsa Regional Hospital, Faculty of Medicine of Monastir, Tunisia
2Orthopedics and Traumatology Department, Tunisia
3Emergency Medicine Department, Gafsa Regional Hospital, Tunisia
Author and article information
Cite this as
Daly H, Hmidi A, Mnassri C, Smari S (2022) Management of serious arterial injuries of the limbs. Int J Vasc Surg Med. 2022; 8(1): 11-17. Available from: 10.17352/2455-5452.000042
Copyright License
© 2022 Daly H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: The majority of arterial traumas concern the arteries of the limbs and today most often occur in a multiple lesion context. In addition, the iatrogenic pathology due to catheterizations, and the specific accidents of drug addiction have been added to classic vascular trauma and pose a specific management problem.
Objective: The objective of this study is to compare the results of our series with other data from the literature. This, in order to elucidate the intersections as well as the differences, the purpose of which is to codify the principles of management of serious vascular trauma to the limbs.
Patients and methods: A retrospective review was conducted in the Cardiovascular Surgery Department of Gafsa Hospital, of 23 patients with severe vascular limb trauma between 2012 and 2020. Patient data included socioeconomic data, mechanism lesion, the clinical admission profile, the vascular axis affected, whether or not an additional examination is carried out, the associated lesions as well as the therapeutic management and evolution. Our series excluded patients lost to follow-up as well as those admitted for minor arterial trauma.
Results: The average age of our patients was 38.3 years (extremes: 3 and 81), with a clear male predominance of 86.7%. The mechanism was primarily weapon assault white (39%) followed by iatrogenic accidents (35%) and public road accidents (13%). The upper limb was the most traumatized (52%). In the most affected territories, there was the wound of the brachial artery in the first place (34.8%), followed by the territory of the common femoral artery (21.7%). The most frequent clinical picture was the association of hemorrhage with ischemia (34.8%), followed by hemorrhage (30.8%) then false aneurysms (21.7%). During our series, CT angiography was requested in 30.7% of patients, and arterial echo-Doppler for 26% of patients. The surgical intervention was an end-to-end suture (34.7%), the interposition of a venous graft was performed in 4.3% of cases, and 5 patients benefited from a bypass (21.7%). Limb salvage was 100%.
Conclusion: The management of serious vascular trauma has experienced great development in terms of diagnostic and therapeutic means which aim to revascularize the affected limb and stop the bleeding, on which the functional and vital prognosis depend respectively.
Under the name of serious vascular trauma of the limbs, are grouped all the lesions of the arterial and venous vessels threatening both the vital prognosis of the patient as well as the functional prognosis of the affected limb and whose origin is traumatic [1]. In civilian practice, arterial trauma very often forms part of polytrauma. Their local and general factors of severity are at the origin of great difficulty in diagnosis, initial management, and treatment. These modern aspects of civilian arterial trauma have largely benefited from military experience, particularly American experience during the Viet Nam War, and since then have been constantly enriched by the contribution of new techniques such as endovascular surgery [2]. The goals of the treatment are to preserve the vital prognosis by hemostasis, but also the functional prognosis by the revascularization of the limb or the territory concerned, and the simultaneous treatment of the associated lesions whenever possible [3]. The prognosis of vascular trauma to the limbs, wounds, or contusion, has been considerably improved thanks to faster transport of the injured, progress in angiographic investigations, and the development of vascular surgery techniques [4].
Through a retrospective study of 23 cases of serious vascular trauma to the limbs treated in the cardiovascular surgery department of the regional hospital of Gafsa, we will try to clarify the epidemiological profile of serious vascular lesions, the clinical manifestations of patients at admission, as well as treatment outcomes.
Materials and methods
This is a retrospective study extended over 9 years, between May 2012 and September 2020, about 23 patients with severe vascular trauma of limbs were treated in the cardiovascular surgery department of the regional hospital of Gafsa.
After studying the files of patients who had been admitted for treatment of vascular trauma of limbs, we selected those who threatened the vital and/or functional prognosis of our patients.
From our study, were excluded
- Patients lost to follow-up during the period of our study.
- Minor arterial trauma to the limbs (isolated radial artery or isolated ulnar artery).
- Pure venous wounds.
- Rupture of aneurysms on arteriovenous fistulas.
Results
We operated on 23 patients during the study period. Their average age was 38.3 years with extremes of 3 years and 81 years. The majority of vascular trauma patients were men (n=20, 86, 7%).
Vascular trauma has been found to be linked in decreasing order of frequency to:
- Aggression in 9 cases (39%). It was a bladed weapon in all cases.
- An iatrogenic accident in 8 cases (35%). It was an accident post-cardiac catheterization in 4 cases, a hemodialysis catheter in 1 case, a central venous catheter in one case, and a defective open-hearth plate, during a proximal tibial osteotomy, in 2 cases.
- A public road accident in 3 cases (13%).
- A domestic accident in 2 cases (9%).
- A work accident in 1 case (4%).
The clinical signs on patient admission are summarized in Table 1. It should be noted that of the 23 patients in our series, eight presented two clinical signs at the same time (acute ischemia with hemorrhage).
In our study, we collected 23 arterial lesions sometimes associated with venous or nerve lesions. There were 12 attacks on the upper limb (52%) and 11 attacks on the lower limb (48%).
The overall topographical distribution of arterial lesions is shown in Table 2.
The nature of the vascular lesions is distributed in order of frequency as follows:
- A total circumferential section involving the three tunics in 9 cases.
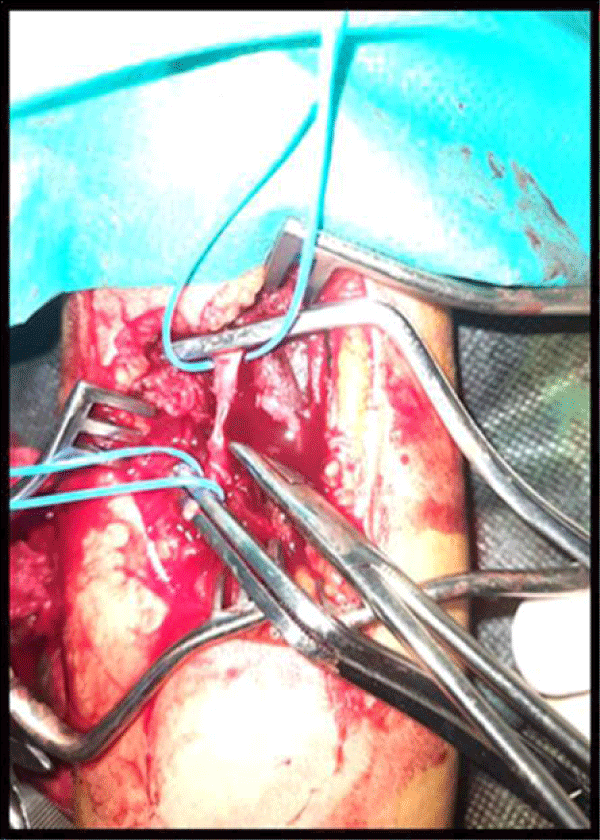
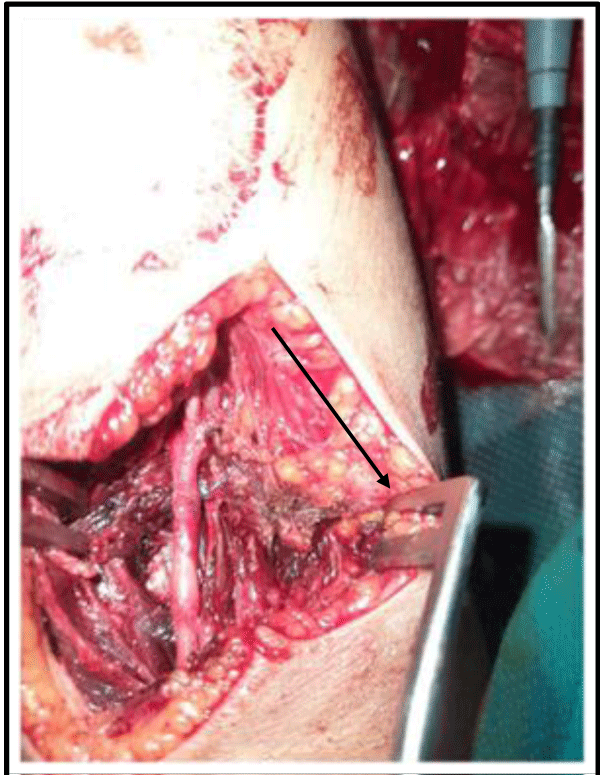
- A partial section in 6 cases Figure 1.
- An isolated false aneurysm in 5 cases.
- A contusion with thrombosis in 1 case.
- An isolated AVF in 2 cases.
It should be noted that the coexistence of a section-contusion has been recorded and has imposed, in some cases, the use of a large resection of the contused arterial wall.
Nerve damage was the associated lesion most frequently observed during vascular trauma to the limbs. We counted 8 lesions in 6 patients (26%).
During the brachial artery lesions, the associated nerve damage following a stab wound was related to a section of the median and radial nerve in 1 case and an isolated section of the musculocutaneous nerve in 2 cases.
During the bi-pedicular wounds of the forearm, the associated nerve damage was related to a section of the median and ulnar nerves in 1 case and a section of the ulnar nerve in 2 cases.
Nerve damage during vascular trauma to the lower limb was present in only 1 case. It was a lesion of the external popliteal sciatic nerve in a patient who presented with a pseudoaneurysm of the anterior tibial artery.
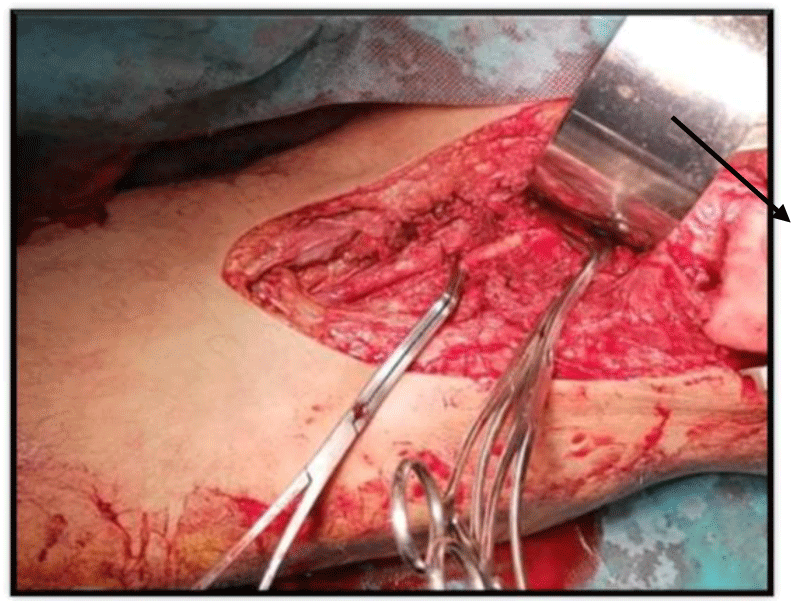
For bone lesions, one patient (4.3%) in our series had an open wrist fracture Figure 2.
Soft tissue lesions were observed in 6 patients (26%). It was a muscle section involving the biceps brachii muscle in 3 cases, and a tendinous section involving the tendons of the anterior face of the wrist in 3 cases.
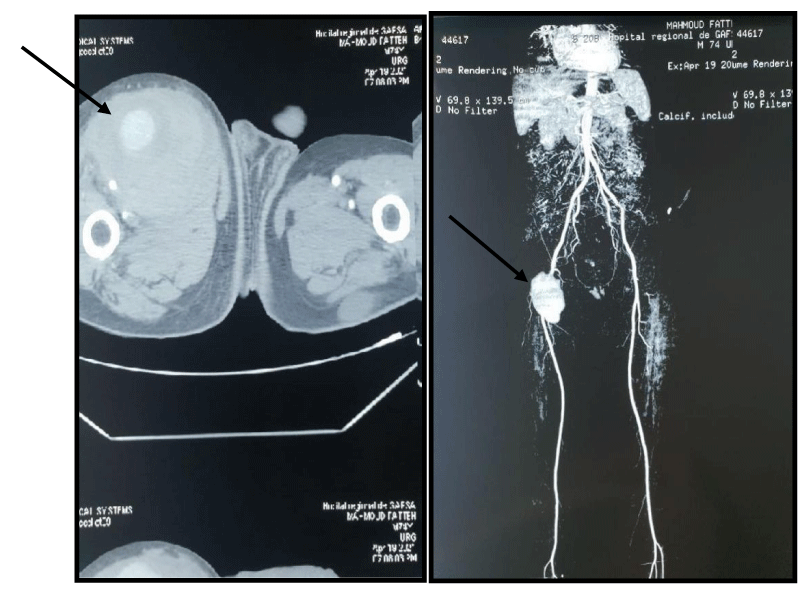
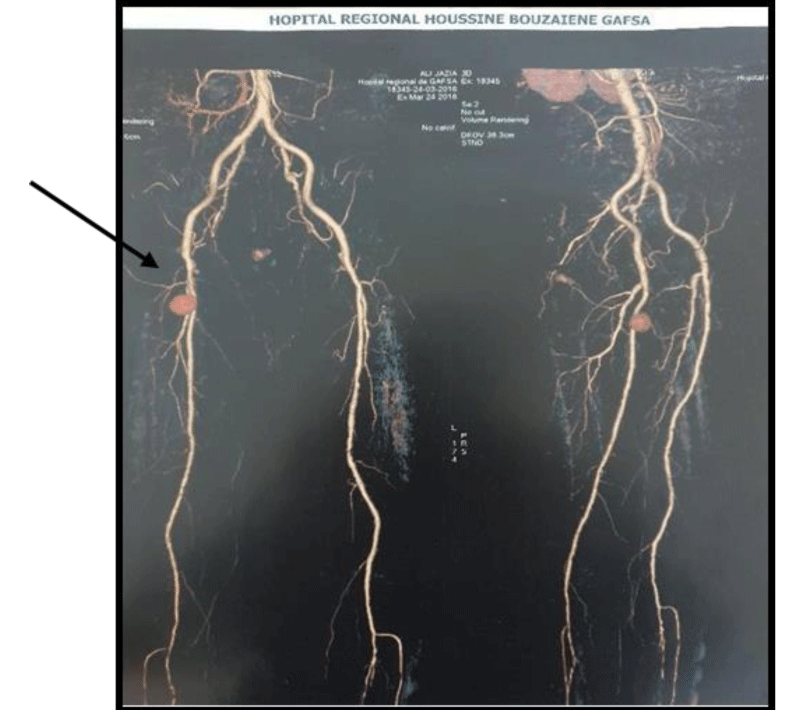
Preoperative radiological exploration was not carried out in all patients because the clinical picture is was strongly suggestive of the presence of a vascular lesion on the one hand, or the urgent nature of a restorative surgical exploration on the other go. Preoperative echo-Doppler was performed in 6 patients (26%) Figures 3,4.
Preoperative CT angiography was performed in 7 patients (30.4%), first-line in 2 cases and second-line in 5 cases; it was in favor of a pseudoaneurysm (n=5) involving the common femoral artery in 2 cases, the artery deep femoral artery in 1 case and the superficial femoral artery in 1 case and the anterior tibial artery in 1 case. Thrombosis was observed in 1 case involving the popliteal artery and an isolated AVF in a single case also involving the common femoral artery.
The simple lateral suture was performed in 2 patients (8.7%), it was a wound of the external iliac artery (n=1) and the common femoral artery (n=1). The end-to-end suture was performed in 8 cases (34.7%), during the repair of the brachial artery (n=5), and during a section of the two pedicles of the forearm in 3 cases. Vein graft interposition was used in 1 patient (4.3%) due to a complete section of the brachial artery with loss of substance and absence of arterial and graft end incongruence. venous. We opted for the technique of venous bypass by the reversed saphenous vein in 5 patients (21.7%), in view of the presence of a complete arterial section with loss of substance and incongruence of the arterial ends and the venous graft. During the section of the axillary artery (n=1), a complete section of the brachial artery in (n=1), a partial section of the common femoral artery (n=1), and a lesion of the popliteal artery (n=2) (one thrombosis and one hemisection).
Surgical treatment of pseudoaneurysms involves first checking the common femoral artery or the external iliac artery via a supracrural approach, then opening the aneurysmal pocket and closing the arterial breach using separate stitches. For the false aneurysm involving the anterior tibial artery, we checked the sub-articular popliteal artery. We performed this technique on 5 patients (21.7%).
Exclusion of the femoral AVF (n=1) was done by the conventional Scarpa approach. Arteries and veins upstream and downstream of the AVF were dissected. After general heparinization and clamping, the fistula was flattened. We repaired the vein and the artery with separate stitches using Prolene 6/0.
The humor-basilic arteriovenous fistula (n=1) was excluded by approaching the brachial artery and the basilic vein at the elbow crease.
We did not collect any deaths in our series. Acute ischemia of the postoperative upper limb by thrombosis at the proximal clamping site was recorded in 1 case for which the patient underwent an embolectomy with good evolution. In the long term, 22 patients (95.6%) have evolved well. Estimation of the residual functional impotence of the affected limb secondary to nerve damage accompanying a bipedicular lesion was faced with the difficulties of long-term follow-up of a patient.
Discussion
In our series, penetrating stab wounds constitute the first cause of serious vascular trauma to the limbs (39%), followed by iatrogenic accidents (35%), accidents on public roads (13%), domestic accidents (9%), and accidents at work (4%).
This clear predominance of penetrating stab wounds during our series is also seen in other reviews conducted in countries with socio-cultural and economic similarities with ours [5-7].
In the study conducted by Hoseong Cho [8] in South Korea, the circumstances of the occurrence of these lesions were in report with penetrating lesions in 28.6% of cases, blunt trauma in 71.4%, and following an iatrogenic accident in 32% of patients. Bains [9], for his part, carried out a cohort study that collected 182 cases of vascular trauma, during which iatrogenic trauma dominated the mechanism of occurrence with 73% of cases.
In comparison with the Western series by Mary [10], Magee [11] and Bains [9], in which public road accidents and iatrogenic trauma represent one of the most frequent causes of serious vascular lesions of the limbs, we note that in our series they represent only 13% and 35% for each. This is explained on the one hand by the high standard of living of the population which is manifested by the number of individual vehicles, road traffic, and therefore the number of AVPs.
The association of hemorrhage and ischemia represents the most frequently observed clinical form during our study (34.8%). Hemorrhage was the first warning sign in almost 80% of cases during the series of Fokou [6], Luan [7], and Mary [10], however, ischemia only comes second with rates of 18.3%, 9.75%, and 30.6% respectively. The studies of Singh [12] in India and Naser [13] in Iran had known a clear predominance of ischemia, 85%, and 61% respectively followed by hemorrhage. This variability in clinical aspects can be explained by the fact that a state of hemorrhagic shock or associated paralysis can mask the picture of acute ischemia.
During our series, we note the predominance of upper limb involvement in 52% of cases. This predominance is related to stabbing as the primary etiological factor. This topography has been noted by other authors in civil practice such as Rasouli [5] in Iran, Fokou [6] in Cameroon, Magee [11] and Perkins [14] in Great Britain, Menakuru [15] in India, Cakir [16] in Turkey, and Franz [17] and Diamond [18] in the United States. On the other hand, the predominant involvement of the arteries of the lower limbs has been described by Singh [12] in India and Rozycki [19] in the United States. In the upper limb, trauma to the subclavian artery is rare and potentially fatal, estimated at 1 to 2% of all vascular trauma [20]. In our study, we collected only one case of axillary artery trauma. During our series, involvement of the brachial artery was predominant. Several studies in the literature mention this predominance [11,15]. On the other hand, in Fokou [6] and Rasouli [5] in their studies carried out respectively in Cameroon and Iran, countries having socio-cultural and economic similarities with ours, the lesion of the two pedicles of the forearm was predominant. As for the lower limb, the lesion of the common femoral artery was the most frequent (21.7%) of the lesions of the lower limb in our series, something which has not been described by most of the authors of the literature, this is explained by the frequency of iatrogenic accidents observed during vascular trauma, in particular cardiac catheterization and access for hemodialysis.
Nerve damage is a mechanism of contusion and elongation with tearing or nerve injury. Their frequency is variable with a predominance in the upper limbs. These neurological lesions condition the functional prognosis. Their existence is a very unfavorable prognostic factor [1]. It is important to be informed about the high frequency of nerve damage because the preoperative estimate of neurological function is difficult to determine in an ischemic limb, especially in a patient who is unconscious or sometimes under the influence of alcohol or drugs. . Even intraoperatively, nerve damage may not be recognized if it is not actively sought [21]. In our series, the nerve damage was present in 26% of cases, mainly in the upper limb (83.3%).
Associated osteoarticular lesions are particularly frequent in lesions of the brachial artery and the popliteal artery. These traumas pose the problem of the sequence of osteo-ligament repairs and arterial restoration [1]. In our series, they existed in 4.3% of cases. The low percentage of associated bone lesions in our series is due to the fact that the etiology of the majority of vascular trauma to the limbs is related to penetrating stab wounds, whereas fractures are seen mainly during fairly violent trauma in a public road accident and work accidents.
The presence of classic signs commonly linked to major arterial trauma, such as the perception of a thrill, an expanding hematoma, and ischemia, has a sensitivity close to 100%, allowing the use of surgical exploration to be considered mandatory [22]. Rapid detection of an arterial lesion as well as its location and anatomopathological characteristics remains essential for efficient management [23].
Apart from serious vascular trauma where the diagnosis is often obvious, echo-Doppler can have a place in the exploration of cases where the arterial lesion is suspected. Its advantages are its rapid implementation at the patient’s bedside and its non-invasive nature. Its repetition is easy to judge a possible evolution. This examination takes all its interest in the detection of arterial lesions that are not very symptomatic [1]. The limits of echo-Doppler are however obvious because it is an operator-dependent examination and does not detect lesions of the collateral arterial branches, nor isolated intimal lesions. It is also very difficult to do a Doppler on a bruised and painful limb or after the placement of a plaster splint [1]. In our series, echo-Doppler was performed in 6 cases (26%).
Some authors, like Zahi [24] and Johansen [25], have highlighted the role of systolic pressure index (SPI) measurement in the diagnostic management of limb vascular trauma. Their results were in favor of a sensitivity close to 80% and a specificity of up to 100% in the detection of these arterial lesions. As a result, they concluded that the arterial Doppler associated with the measurement of the SPI should be an integral part of the management of vascular trauma to the limbs, without being able to prejudge the mandatory nature of the surgical indication.
CT angiography has become the paraclinical examination of choice in the detection of paucisymptomatic arterial lesions and has served to reduce the number of white surgical explorations [22]. In the study by Dina et al. [26] Having focused on 38 patients who presented with penetrating trauma to the lower limb in a level I trauma center, the use of first-line CT angiography for the initial evaluation did not show any false negatives. The CT angiography in our series was performed on 7 patients (30.4%) requiring preoperative exploration. In the study by Soto et al [27] CT angiography had a sensitivity of 90% and a specificity of 100% in the detection of arterial lesions proximal to the limbs. Two other studies, Inaba [28] and Rieger [29], showed a sensitivity of 95 to 100% with a specificity of 87 to 100% in highlighting vascular lesions of the limbs.
Arterial repair follows well-known principles; it must be as conservative as possible (suture or resection anastomosis), with the help of dissection of the two extremities and the collaterals to mobilize the artery and perform a tension-free anastomosis in a perfectly healthy area [30]. Associated osteoarticular lesions are particularly frequent in lesions of the brachial artery and the popliteal artery. These osteovascular traumas pose the problem of the sequence of osteoligamentary repairs and arterial restoration [1].
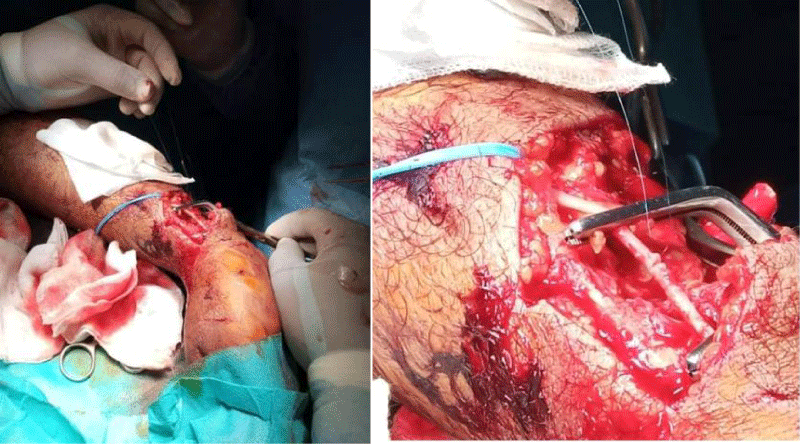
Approaches differ depending on the level of arterial damage, which is often difficult to predict [4]. The approach should expose the vascular pedicle so if possible, using a classic elective incision, which gives rapid access to the arterial axis while avoiding blunt skin wounds due to trauma [1]. In our series, the most used surgical technique was the end-to-end suture (34.7%) Figure 5. This stems from the predominance of complete sections, which were the most frequently encountered lesions. These gestures are the most performed, although in different proportions by certain authors, notably Fokou [6] (63.4%), Luan Jaha [7] (58.3%), and Singh [12] (57.8%). Direct suturing is possible in some lateral wounds after checking the intima on either side of the wound. The direct suture of a longitudinal wound always leads to relative stenosis which is tolerable on an artery of more than 10 mm in diameter. It is, on the other hand, dangerous on a small diameter artery which usually requires the use of an enlargement patch [1]. The flattening of the false aneurysm with arterial suture and venous bypass comes in the background during our experience (21.7%), and finally, the interposition of a venous graft in one case (4.3%); this last technique was used in the reviews by Magee (21.3%) [11] and Luan (15%) [7]. The VSI bypass is used when the end-to-end anastomosis is impossible because of the excessive tension generated by the resection. Magee [11] reports in his series that VSI bypass was the most common method of treatment of arterial damage at 44.5%, while in our series it was only 21.7%. Autogenous vein grafting between the two arterial ends is the best revascularization technique when the loss of substance is significant. It is a reliable technique suitable for the treatment of extensive arterial contusions [1]. Most authors [31] conclude that the autologous vein should be considered the material of choice in arterial repairs. The reversed long saphenous vein is suitable for all subcrural, axillo-subclavian, and subaxillary revascularizations. In the absence of a usable saphenous vein, a prosthetic bypass is possible. The use of vascular prostheses in arterial trauma has led to many controversies [1].
If nerve damage is to be actively sought, primary nerve repair along with the vascular repair is questionable. For some authors, early surgery, after two weeks of trauma, is proposed to optimize the functional outcome of nerve repair [21]. In Brown’s series [32], 42% of patients had undergone repair undertaken at the time of arterial repair. These patients tend to have a better outcome compared to patients who have had delayed nerve repair, because of the greater degree of severity of the damage they presented. Indeed, according to the author, these were patients who were unstable or whose viability of the limb was very uncertain. Pailler [3] and Saide [33] report that in the event of nerve damage, suturing is justified from the outset in clean, open wounds; on the other hand, it seems preferable to postpone the repair in the debilitating traumas. Optimal complete revascularization optimizes nerve repair. The 2-week delayed nerve repair procedure will also allow the nature of the lesion to be correctly diagnosed [21] (Figure 6).
Best [34] and Mellesi [35] report that despite a large number of experiments and clinical studies, the dynamism and mechanism of nerve repair have not been established. Leclerq [36] reports that the results of nerve reconstruction after arterial repair are superior to cases where the arteries are intact. He explains this improvement by the fact that the periarterial sympathectomy performed during vascular repair probably facilitates the revascularization of the distal nerves. In our practice, we prefer to perform nerve and vascular repairs at the same time, in collaboration with the trauma team. Thus in our series, the associated nerve lesions were repaired at the same time as the vascular repair in 5 patients (83.3%).
Bone trauma is often the witness of the violence of the shock and is associated with significant lesions of the soft parts, in particular in the event of open trauma [3]. The use of an external fixator represents the most suitable osteosynthesis for osteovascular trauma to the limbs because it does not require an elective first, it does not aggravate the tissue contusion and does not present a risk of exposure. during aponeurotomy and it is a quick procedure that reduces the ischemia time [1]. Some authors prefer to carry out the reduction and stabilization of the bone foci before revascularization, to avoid any secondary mobilization which could compromise the permeability of the arterial revascularization. In this case, a temporary arterial shunt was once useful to reduce the arterial ischemia time [37,38].
Although bone repairs followed by vascular repairs appear to be the most appropriate method in vascular injuries associated with unstable fractures, the final decision must be made on an individual basis. In this approach, cooperation between vascular surgeons and traumatologists is important [39].
The limitations of this study include the small number of cases of vascular trauma, the presence of fewer cases of contending trauma than of open and iatrogenic trauma, and the non-randomized retrospective observational design of the study which partly explains the absence of death and primary or secondary amputation.
Conclusion
Severe vascular trauma to the limbs is seen mainly in young adult males. The mechanism of injury seems to vary between different parts of the world. The circumstances of occurrence in our context were mainly dominated by stab wounds. The nature of the arterial lesion is a frank rupture involving the three coats in most cases. The treatment performed is often end-to-end anastomosis resection or venous bypass. The evolution is favorable for all the patients even those who had a nerve lesion. Improving the prognosis of vascular trauma to the limbs requires rapid treatment, minimizing the time to revascularization and treatment, if possible, of the associated nerve damage.
Hafedh daly: Acquisition, data analysis, and writing
Abderrahim Hmidi, Sandess SMARI, and Cyrine MNASSRI: Acquisition, and analysis of results.
- Ricco J.-B., Fébrer G. Traumatismes vasculaires des membres. EMC, techniques chirurgicales - chirurgie vasculaire, 43-025, 2006.
- Traumatismes artériels des membres. Université de Lyon 1.
- Pailler JL, Baranger B, Chemla E. principes généraux du traitement chirurgical des traumatismes artériels des membres. Les traumatismes artériels E. Kieffer. Edition AERCV Nov 1995 : 45-53.
- Leguerrier A, Lebeau G, Leveque JM, Rosat P. traumatismes vasculaires des membres. Bilan de 106 lésions vasculaires chez 76 blessés. J chir 1986. 123(2):108-116.
- Rasouli MR, Moini M, Khaji A. Civilian traumatic vascular injuries of the upper extremity:report of the Iranian national trauma project. Ann Thorac Cardiovasc Surg. 2009 Dec;15(6):389-93. PMID: 20081748.
- FokouM., Chichom M., Eyenga V. and all. les traumatismes vasculaires périphérique en pratique civile. A propos de 41 lésions opérés au Cameroun. Chirurgie thoracique cardiovasculaire- 2011; 15(3):145-149.
- Jaha L, Andreevska T, Rudari H, Ademi B, Ismaili-Jaha V. A decade of civilian vascular trauma in Kosovo. World J Emerg Surg. 2012 Jul 20;7(1):24. doi: 10.1186/1749-7922-7-24. PMID: 22817978; PMCID: PMC3472200.
- Cho H, Huh U, Lee CW, Song S, Kim SH, Chung SW. Traumatic Peripheral Arterial Injury with Open Repair: A 10-Year Single-Institutional Analysis. Korean J Thorac Cardiovasc Surg. 2020; 53(5):291-296.
- Bains SK, Valchou PA, Rayt HS, Dennis M. The Royal Colleges of Surgeons of Edinburgh and Ireland. Surgeon. 2009; 7 ; 6 : 332-35.
- Giswold ME, Landry GJ, Taylor LM, Moneta GL. Iatrogenic arterial injury is an increasingly important cause of arterial trauma. Am J Surg. 2004 May;187(5):590-2; discussion 592-3. doi: 10.1016/j.amjsurg.2004.01.013. PMID: 15135671.
- Magee TR, Collin J, Hands LJ, Gray DW, Roake J. A ten year audit of surgery for vascular trauma in a British teaching hospital. Eur J Vasc Endovasc Surg. 1996 Nov;12(4):424-7. doi: 10.1016/s1078-5884(96)80007-4. PMID: 8980430.
- Singh D, Pinjala RK. Management Of Peripheral Vascular Trauma: Our Experience. The Internet Journal of Surgery. 2005; 7.
- Kohli A, Singh G. Management of extremity vascular trauma: Jammu experience. Asian Cardiovasc Thorac Ann. 2008 Jun;16(3):212-4. doi: 10.1177/021849230801600307. PMID: 18515670.
- Perkins ZB, De'Ath HD, Aylwin C, Brohi K, Walsh M, Tai NR. Epidemiology and outcome of vascular trauma at a British Major Trauma Centre. Eur J Vasc Endovasc Surg. 2012 Aug;44(2):203-9. doi: 10.1016/j.ejvs.2012.05.013. Epub 2012 Jun 2. PMID: 22658774.
- Menakuru SR, Behera A, Jindal R, Kaman L, Doley R, Venkatesan R. Extremity vascular trauma in civilian population: a seven-year review from North India. Injury. 2005 Mar;36(3):400-6. doi: 10.1016/j.injury.2004.06.017. PMID: 15710157.
- Cakir O, Subasi M, Erdem K, Eren N. Treatment of vascular injuries associated with limb fractures. Ann R Coll Surg Engl. 2005 Sep;87(5):348-52. doi: 10.1308/003588405X51146. PMID: 16176694; PMCID: PMC1963979.
- Franz RW, Goodwin RB, Hartman JF, Wright ML. Management of upper extremity arterial injuries at an urban level I trauma center. Ann Vasc Surg. 2009 Jan-Feb;23(1):8-16. doi: 10.1016/j.avsg.2008.04.012. Epub 2008 Jul 21. PMID: 18640813.
- Diamond S, Gaspard D, Katz S. Vascular injuries to the extremities in a suburban trauma center. Am Surg. 2003 Oct;69(10):848-51. PMID: 14570361.
- Rozycki GS, Tremblay LN, Feliciano DV, McClelland W.B.Blunt vascular trauma in the extremity: diagnosis, management and outcome. J. Trauma 2003; 55 : 814-824.
- Rich NM, Hosson RW, Jarstfer BS. Subclavian artery trauma. J. Trauma. 1973 ; 13 : 485-96.
- Shaw AD, Milne AA, Christie J, Jenkins AM, Murie JA, Ruckley CV. Vascular trauma of the upper limb and associated nerve injuries. Injury. 1995 Oct;26(8):515-8. doi: 10.1016/0020-1383(95)00090-v. PMID: 8550137.
- Foster BR, Anderson SW, Soto JA. CT angiography of extremity trauma. Tech Vasc Interv Radiol. 2006 Dec;9(4):156-66. doi: 10.1053/j.tvir.2007.02.009. PMID: 17709080.
- Doody O, Given MF, Lyon SM. Extremities--indications and techniques for treatment of extremity vascular injuries. Injury. 2008 Nov;39(11):1295-303. doi: 10.1016/j.injury.2008.02.043. Epub 2008 Oct 8. PMID: 18845300.
- Nassoura ZE, Ivatury RR, Simon RJ, Jabbour N, Vinzons A, Stahl W. A reassessment of Doppler pressure indices in the detection of arterial lesions in proximity penetrating injuries of extremities: a prospective study. Am J Emerg Med. 1996 Mar;14(2):151-6. doi: 10.1016/S0735-6757(96)90122-9. PMID: 8924136.
- Johansen K, Lynch K, Paun M, Copass M. Non-invasive vascular tests reliably exclude occult arterial trauma in injured extremities. J Trauma. 1991 Apr;31(4):515-9; discussion 519-22. PMID: 2020038.
- Dina W, Yaghoubian A, Rosing D. L’angioscanner comme examen diagnostique de référence dans les lésions vasculaires pénétrantes des membres inférieurs : L’expérience d’un trauma-center de niveau I. Ann Vasc Surg 2011; 25: 620-623.
- Soto JA, Múnera F, Morales C, Lopera JE, Holguín D, Guarín O, Castrillón G, Sanabria A, García G. Focal arterial injuries of the proximal extremities: helical CT arteriography as the initial method of diagnosis. Radiology. 2001 Jan;218(1):188-94. doi: 10.1148/radiology.218.1.r01ja13188. PMID: 11152800.
- Inaba K, Potzman J, Munera F, McKenney M, Munoz R, Rivas L, Dunham M, DuBose J. Multi-slice CT angiography for arterial evaluation in the injured lower extremity. J Trauma. 2006 Mar;60(3):502-6; discussion 506-7. doi: 10.1097/01.ta.0000204150.78156.a9. PMID: 16531846.
- Rieger M, Mallouhi A, Tauscher T, Lutz M, Jaschke WR. Traumatic arterial injuries of the extremities: initial evaluation with MDCT angiography. AJR Am J Roentgenol. 2006 Mar;186(3):656-64. doi: 10.2214/AJR.04.0756. PMID: 16498092.
- Perry MO, Thal ER, Shires GT. Management of arterial injuries. Ann Surg. 1971 Mar;173(3):403-8. doi: 10.1097/00000658-197103000-00011. PMID: 4927238; PMCID: PMC1397393.
- Razmadze A. Vascular injuries of the limbs: a fifteen-year Georgian experience. Eur J Vasc Endovasc Surg. 1999 Sep;18(3):235-9. doi: 10.1053/ejvs.1999.0857. PMID: 10479630.
- Brown KR, Jean-Claude J, Seabrook GR, Towne JB, Cambria RA. Determinates of functional disability after complex upper extremity trauma. Ann Vasc Surg. 2001 Jan;15(1):43-8. doi: 10.1007/s100160010016. PMID: 11221943.
- Saide R, Jacobsen DC, Bloch JH, Philips CV. Management of peripheral vascular trauma. Am Surg. 1981; 47(10):429-438.
- Best TJ, Mackinnon SE. Peripheral nerve revascularization: a current literature review. J Reconstr Microsurg. 1994 May;10(3):193-204. doi: 10.1055/s-2007-1006587. PMID: 8071907.
- Peripheral nerve surgery today, turning point or continuous development? Part III. Proceedings. Vienna, Austria, November 23-26, 1991. J Reconstr Microsurg. 1994 May;10(3):205-19. PMID: 7915323.
- Leclercq DC, Carlier AJ, Khuc T, Depierreux L, Lejeune GN. Improvement in the results in sixty-four ulnar nerve sections associated with arterial repair. J Hand Surg Am. 1985 Nov;10(6 Pt 2):997-9. doi: 10.1016/s0363-5023(85)80023-x. PMID: 3908550.
- Bassett FH 3rd, Silver D. Arterial injury associated with fractures. Arch Surg. 1966 Jan;92(1):13-9. doi: 10.1001/archsurg.1966.01320190015003. PMID: 5901252.
- Wolma FJ, Larrieu AJ, Alsop GC. Arterial injuries of the legs associated with fractures and dislocations. Am J Surg. 1980 Dec;140(6):806-9. doi: 10.1016/0002-9610(80)90122-1. PMID: 7457706.
- Katsamouris AN, Steriopoulos K, Katonis P, Christou K, Drositis J, Lefaki T, Vassilakis S, Dretakis E. Limb arterial injuries associated with limb fractures: clinical presentation, assessment and management. Eur J Vasc Endovasc Surg. 1995 Jan;9(1):64-70. doi: 10.1016/s1078-5884(05)80227-8. PMID: 7664015.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
