International Journal of Vascular Surgery and Medicine
Surgical Management of Peripheral Arterial Disease in Cameroon: A Case Series and Review of the Literature
1Division of Cardiac Surgery, Shisong Cardiac Center, Kumbo, Cameroon
2Division of Thoracic and Cardiovascular Surgery, Yaoundé General Hospital, Yaoundé, Cameroon
3Department of Surgery, Faculty of Medicine and Biomedical Sciences, University of Yaoundé l, Yaoundé, Cameroon
4Department of Internal Medicine, Faculty of Medicine and Biomedical Sciences, University of Yaoundé l, Yaoundé, Cameroon
5Department of Surgery, Faculty of Medicine and Pharmaceutical Sciences, University of Douala, Douala, Cameroon
Author and article information
Cite this as
Mvondo CM, et al. Surgical Management of Peripheral Arterial Disease in Cameroon: A Case Series and Review of the Literature. Int J Vasc Surg Med. 2026; 12(1): 1-5. Available from: 10.17352/2455-5452.000048
Copyright License
© 2026 Mvondo CM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Peripheral arterial disease (PAD) is an increasingly recognized manifestation of atherosclerotic cardiovascular disease in sub-Saharan Africa (SSA). However, the condition remains frequently underdiagnosed, and many patients present at advanced stages with chronic limb-threatening ischemia (CLTI). This study aimed to describe the surgical management of PAD in Cameroon and to compare our findings with previously reported African and low- and middle-income country (LMIC) series.
Methods: We conducted a retrospective case series of patients treated surgically for peripheral arterial disease between March 2025 and February 2026 at the Division of Thoracic and Cardiovascular Surgery at the Yaoundé General Hospital in Cameroon. Demographic characteristics, cardiovascular risk factors, clinical presentation, and surgical procedures were analyzed. A narrative review of the literature on PAD management in SSA and LMICs was also performed.
Results: Thirty-two patients (n = 32) underwent surgical treatment for PAD. The mean age was 69 ± 5 years (range: 65 – 75), and all patients were male. Hypertension was present in 23 patients (71.8%), smoking in 15 (46.8%), and diabetes mellitus in 8 (25.0%). Most patients presented with advanced CLTI, including Rutherford stage 5 in 8 patients (25.0%) and stage 6 in 14 patients (43.7%). Twenty-four patients (n = 24, 75.0%) required amputation, including 16 major amputations and 8 minor amputations, whereas only 8 patients (25.0%) underwent limb revascularization procedures with femoro-popliteal bypass. Limb salvage was achieved in 7 of the 8 revascularized patients (87.5%). Similar patterns have been reported in several African studies, where late presentation and limited access to vascular surgery contribute to high amputation rates.
Conclusion: In our setting, most patients with PAD present at advanced stages when revascularization is no longer feasible. Strengthening early diagnosis and expanding vascular surgical services are essential to reduce the burden of limb loss in sub-Saharan Africa.
Peripheral arterial disease (PAD) is a manifestation of systemic atherosclerosis affecting the lower limb arteries and represents a major cause of morbidity worldwide [1,2]. The global prevalence of PAD has increased considerably over the past decades, particularly in low- and middle-income countries undergoing epidemiological transition [2].
In sub-Saharan Africa (SSA), the rising prevalence of hypertension, diabetes mellitus, dyslipidemia, and tobacco use has contributed to a growing burden of atherosclerotic vascular diseases, including PAD [1-3]. Despite this trend, PAD remains substantially underdiagnosed in many SSA countries due to limited screening programs, lack of awareness among healthcare providers, and restricted access to vascular imaging [3,4]. As a consequence, many patients present late with chronic limb-threatening ischemia characterized by rest pain, ulceration, or gangrene. While early diagnosis and revascularization have significantly reduced amputation rates in high-income countries, delayed presentation and limited vascular surgical capacity continue to result in high rates of limb loss in many African settings [5-7].
The aim of this study was therefore to describe the surgical management of PAD at our institution in Cameroon and to compare our findings with those of previously reported African and LMIC series.
Methods
Study design and setting
This retrospective observational study was conducted at the Division of Thoracic and Cardiovascular Surgery at the Yaoundé General Hospital in Cameroon. The aim was to evaluate the surgical management of peripheral arterial disease and to compare the findings with previously reported studies from SS and other low- and middle-income countries (LMICs).
Patient population
All consecutive patients undergoing surgical treatment for peripheral arterial disease between March 2025 and February 2026 were included. Peripheral arterial disease was defined clinically and confirmed using available vascular imaging when feasible. Patients presenting with chronic limb-threatening ischemia requiring surgical intervention were eligible for inclusion. The exclusion criteria were: acute limb ischemia and traumatic vascular injuries.
Demographic characteristics, cardiovascular risk factors, clinical presentation, Rutherford classification, surgical procedures and related outcomes were collected from medical records.
Literature review
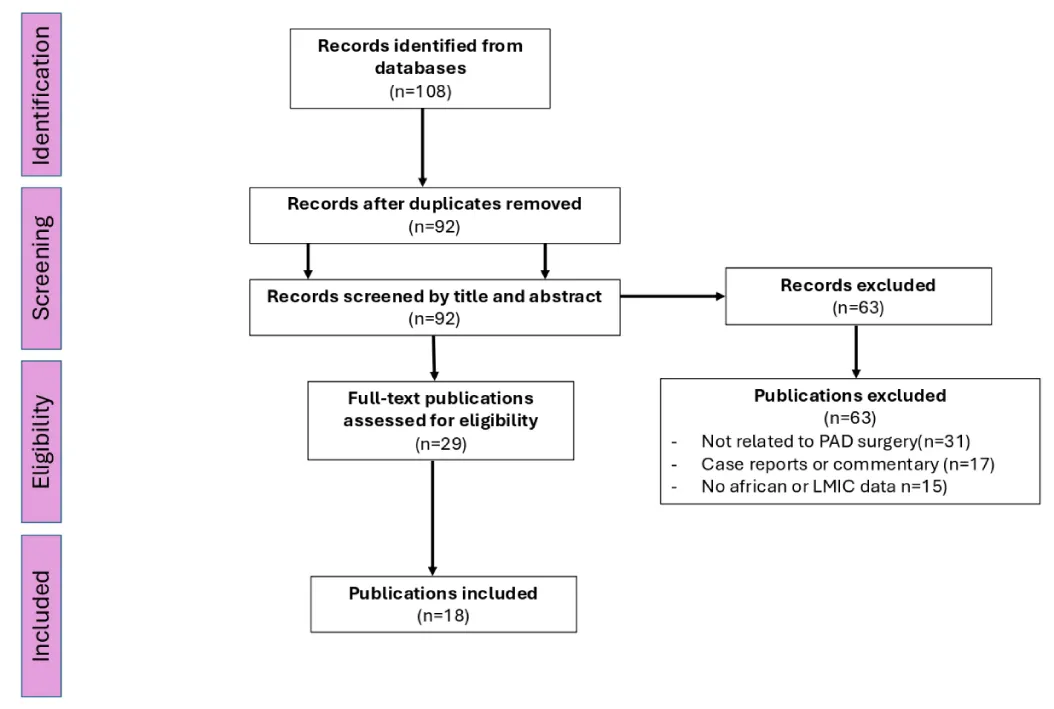
A narrative literature review was conducted following PRISMA principles. Electronic databases, including PubMed/MEDLINE, Scopus, and African Journals Online, were searched for studies reporting the surgical management of PAD in Africa and other LMICs. Search terms included combinations of “peripheral arterial disease,” “critical limb ischemia,” “vascular surgery,” “revascularization,” “amputation,” and “Africa.” Titles and abstracts were screened, and relevant studies were reviewed in full text according to predefined eligibility criteria (Figure 1).
Statistical analysis
Statistical analysis was primarily descriptive due to the exploratory nature of the study and the relatively small sample size. Continuous variables were expressed as mean ± standard deviation (SD), whereas categorical variables were presented as frequencies and percentages. All analyses were performed using SPSS statistical software (IBM Corp., Armonk, NY, USA).
Results
Patient characteristics
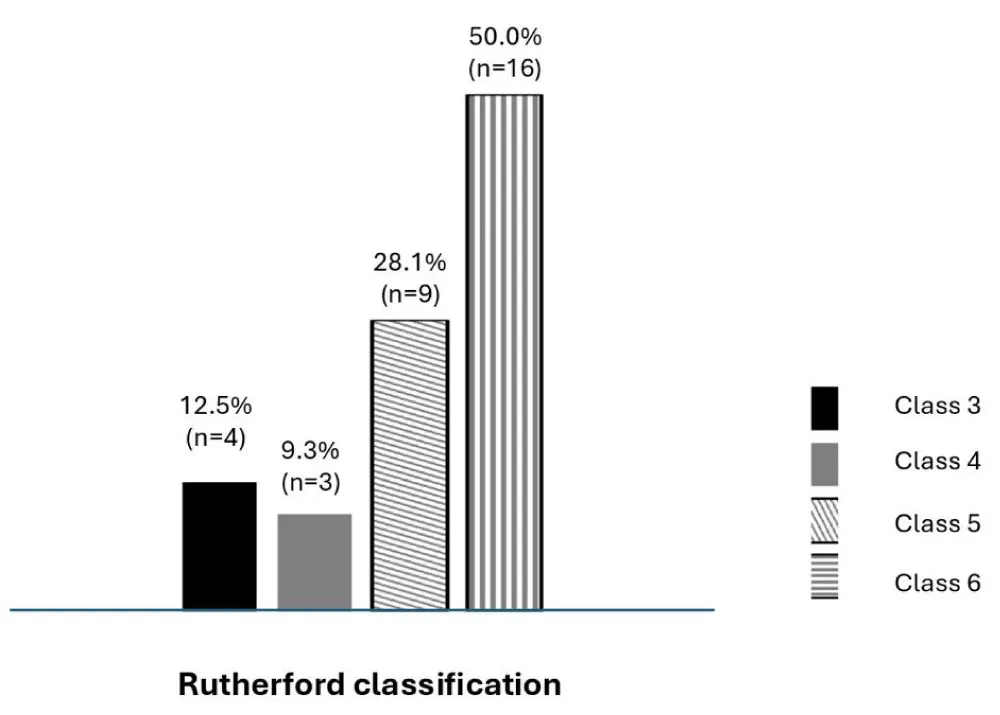
Thirty-two patients underwent surgical treatment for PAD during the study period. The mean age was 69 ± 5 years (range: 65 – 75), and all patients were male. Hypertension was present in 23 patients (71.8%), smoking in 15 (46.8%), and diabetes mellitus in 8 (25.0%). Most patients presented with advanced disease. According to the Rutherford classification, 25 patients (78.1%) presented at stages 5–6 (Figure 2).
Patients’ demographics are summarized in Table 1.
Surgical management
Among the 32 patients treated surgically, 24 patients (75.0%) had amputation: 16 (50.0%) were major amputation procedures (above-knee: 7 patients; below-knee: 9 patients). Minor amputations (n = 8, 25.0%) were Chopard amputation (3 patients) and toe disarticulation (5 patients).
A total of 8 patients (25.0%) had limb revascularization. The revascularization procedures were femoropopliteal bypass with inverted saphenous vein (n = 7/8, 87.5%) and prosthetic vascular graft (n = 1/8, 12.5%). No perioperative mortality was reported. Postoperative complications included 3 cases of superficial wound infection (n = 3/8, 37.5%). Limb salvage was achieved in 7 of the 8 revascularized patients (87.5%) at follow-up (mean duration: 5 months (range: 3–8). A graft failure leading to secondary amputation was reported three weeks after discharge in a 65-year old male patient who underwent femoro-popliteal bypass with PTFE graft. The patient was a heavy smoker with poor compliance with prescribed antiplatelet therapy.
The surgical procedures are listed in Table 2.
Literature review
The literature search identified 108 records, of which 92 remained after removal of duplicates. After screening titles and abstracts, 29 full-text articles were assessed for eligibility, and 18 studies were ultimately included in the review (Figure 1).
Most studies were conducted in sub-Saharan Africa, including South Africa, Ghana and Nigeria. Studies from centers with vascular surgical expertise reported higher limb-salvage rates after revascularization, such as the 88% limb-salvage rate with a 13% major amputation rate reported by Islam and Robbs [8] and the 56% limb-salvage rate at two years after femoro-distal bypass reported by Mwipatayi, et al. [9].
In contrast, studies focusing on diabetic-foot or amputation cohorts reported substantially higher amputation rates, including the 36% major amputation rate reported in the Nigerian cohort by Ugwu, et al. [10]. In Ghana, Bediako-Bowen et al. Reported that PAD was present in approximately 60% of patients undergoing lower-limb amputation [7].
A comparison between the present series and the studies identified in the literature review is summarized in Table 3.
Discussion
PAD is an increasingly important health problem in SSA due to the rising prevalence of non-communicable diseases such as diabetes, hypertension, and smoking [1,2]. However, PAD remains significantly underdiagnosed across the region. Screening studies have demonstrated substantial prevalence of PAD in African populations, particularly among diabetic patients, suggesting that a large number of cases remain undetected until advanced stages of disease [3,6].
Indeed, a key feature of PAD in SSA is late presentation. In many African healthcare systems, patients do not seek medical attention until the development of severe symptoms such as rest pain, ulceration, gangrene, or infected diabetic foot lesions. Several studies have shown that PAD is frequently diagnosed only in patients presenting for amputation or with advanced diabetic foot complications [7].
Another major challenge is the limited vascular surgical capacity available in many African countries. National assessments of surgical infrastructure have revealed substantial deficits in diagnostic imaging, trained vascular surgeons, and revascularization technologies. Consequently, patients who might benefit from revascularization are often treated with primary amputation due to the absence of specialized vascular care [5]. Consequently, the high amputation burden reported in many SSA series illustrates the consequences of this situation, as demonstrated in a previous series [7].
Despite these challenges, the 87.5% limb salvage rate observed in our series demonstrates that open surgical revascularization can provide meaningful benefit when performed in centres with appropriate surgical expertise. These results are consistent with previously reported surgical outcomes where limb salvage rates between 70% and 90% have been reported depending on patient characteristics and lesion severity [4,10].
Improving PAD outcomes in Africa requires a broader strategy beyond surgical intervention alone. Prevention and early detection are essential components of PAD management. Screening high-risk populations using ankle-brachial index measurement and increasing awareness among healthcare providers may facilitate earlier diagnosis and referral. Multidisciplinary collaboration is also critical. Effective CLTI management involves coordination between vascular surgeons, diabetologists, cardiologists, radiologists, wound-care specialists, and rehabilitation teams. International guidelines emphasize the importance of multidisciplinary limb salvage programs in reducing amputation rates [4].
Finally, African vascular programs should progressively consider the integration of endovascular and hybrid techniques when resources permit. Hybrid procedures combining open and endovascular approaches may allow treatment of complex multilevel disease while reducing operative trauma in high-risk patients. Current vascular guidelines recommend individualized revascularization strategies based on anatomy, patient risk profile, and available expertise [4,12]. In the Cameroonian context, the development of endovascular techniques is currently limited by high costs, lack of equipment, and insufficient specialized training. However, gradual integration of hybrid approaches may represent a pragmatic strategy to improve outcomes while adapting to resource constraints.
Developing vascular care in Africa will therefore require strengthening diagnostic capacity, expanding vascular training, improving referral systems, and gradually introducing endovascular technologies alongside traditional open surgery [13-18].
Limitations
This study has several limitations. It is a retrospective single-center study with a relatively small sample size. Detailed vascular imaging was not available for all patients, and long-term follow-up data were limited. Additionally, the absence of endovascular treatment options restricted the range of therapeutic strategies evaluated. Data on dyslipidemia and family history were not consistently available and could not be reliably analyzed.
Conclusion
Peripheral arterial disease and chronic limb-threatening ischemia represent increasing surgical challenges in sub-Saharan Africa. Late diagnosis, limited vascular surgical capacity, and high amputation rates remain major obstacles to effective management. Nevertheless, open surgical revascularization can achieve satisfactory limb salvage outcomes when performed in appropriate centers. Strengthening vascular surgical services, promoting early diagnosis, and expanding multidisciplinary care pathways are essential steps to reduce the burden of limb loss in Africa.
Study strengths
This study provides one of the few surgical series describing the management of PAD in Central Africa. By combining clinical data with a literature review of African and LMIC studies, the study highlights the persistent challenges of late presentation and limited vascular surgical capacity in the region.
Clinical implications
Our findings highlight the urgent need for earlier detection of PAD in sub-Saharan Africa. Increased awareness among primary care physicians and systematic screening of high-risk populations could facilitate earlier referral for vascular evaluation. Strengthening vascular surgical capacity and progressively introducing endovascular techniques may significantly improve limb salvage outcomes.
- Johnston LE, Stewart BT, Yangni-Angate KH, Veller M, Upchurch GR, Gyedu A, et al. Peripheral arterial disease in sub-Saharan Africa: a review. JAMA Surg. 2016;151(6):564-572. Available from: https://doi.org/10.1001/jamasurg.2016.0446
- Fowkes FG, Rudan D, Rudan I, Aboyans V, Denenberg JO, McDermott MM, et al. Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. Lancet. 2013;382(9901):1329-1340. Available from: https://doi.org/10.1016/s0140-6736(13)61249-0
- Dewhurst MJ, Newell J, Dewhurst F, Gray WK. The prevalence of peripheral arterial disease in older people in Africa: a systematic review and meta-analysis. Age Ageing. 2012;41(3):327-331.
- Conte MS, Bradbury AW, Kolh P, White JV, Dick F, Fitridge R, et al. Global vascular guidelines on the management of chronic limb-threatening ischemia. Eur J Vasc Endovasc Surg. 2019;58(1 Suppl):S1-S109.e33. Available from: https://doi.org/10.1016/j.ejvs.2019.05.006
- Gyedu A, Stewart BT, Nakua EK, Otupiri E, Donkor P, Mock CN, et al. Assessment of risk of peripheral vascular disease and vascular care capacity in low- and middle-income countries. Br J Surg. 2016;103(1):51-59. Available from: https://doi.org/10.1002/bjs.9956
- Weledji EP, Alemnji GA, Nouediou C. The use of ankle-brachial pressure indices in a cohort of black African diabetic patients. Ann Med Surg. 2018;35:20-24. Available from: https://doi.org/10.1016/j.amsu.2018.09.009
- Bediako-Bowen AA, Adjei GO, Clegg-Lamptey JNA, Naaeder SB. Peripheral arterial disease among patients undergoing lower limb amputation in Accra, Ghana. Ghana Med J. 2017;51(3):108-114.
- Islam J, Robbs JV. Comparison between superficial femoral artery stenting and bypass surgery in severe lower limb ischemia. Cardiovasc J Afr. 2015;26(1):34-37. Available from: https://doi.org/10.5830/cvja-2014-074
- Mwipatayi BP, Jeffery PC, Motale P, Matley PJ, Kahn D, Welman CJ. Femoro-distal bypass surgery at Groote Schuur Hospital: a retrospective review. S Afr J Surg. 2004;42(3):81-85. Available from: https://pubmed.ncbi.nlm.nih.gov/15532614/
- Ugwu E, Adeleye O, Gezawa I, Okpe I, Enamino M, Ezeani I. Predictors of lower extremity amputation in patients with diabetic foot ulcer: findings from MEDFUN, a multi-center observational study. J Foot Ankle Res. 2019;12:34. Available from: https://doi.org/10.1186/s13047-019-0345-y
- Guerchet M, Aboyans V, Mbelesso P, Mouanga AM, Salazar J, Bandzouzi B, et al. Epidemiology of peripheral artery disease in elderly populations of Central Africa: a population-based study. Eur J Vasc Endovasc Surg. 2012;44(2):164-169. Available from: https://doi.org/10.1016/j.ejvs.2012.05.019
- Paquissi FC. Peripheral arterial disease in sub-Saharan Africa: epidemiology and management challenges. Vasc Health Risk Manag. 2016;12:305-310.
- Motsumi MJ, Naidoo NG. Pattern and distribution of peripheral arterial disease in diabetic patients with critical limb ischemia. S Afr J Surg. 2017;55(3):48-54. Available from: https://pubmed.ncbi.nlm.nih.gov/28876565/
- Adam DJ, Beard JD, Cleveland T, Bell J, Bradbury AW, Forbes JF, et al. Bypass versus angioplasty in severe ischemia of the leg (BASIL): multicentre randomised controlled trial. Lancet. 2005;366(9501):1925-1934. Available from: https://doi.org/10.1016/s0140-6736(05)67704-5
- Farber A, Menard MT, Conte MS, Kaufman JA, Powell RJ, Choudhry NK, et al. Surgery or endovascular therapy for chronic limb-threatening ischemia. N Engl J Med. 2022;387(25):2305-2316. Available from: https://doi.org/10.1056/nejmoa2207899
- Gornik HL, Aronow HD, Goodney PP, Gupta R, Maron DJ, Mohler ER, et al. 2024 ACC/AHA guideline for the management of patients with lower extremity peripheral artery disease. Circulation. 2024;149:e000-e000. Available from: https://doi.org/10.1161/cir.0000000000001251
- Farber A, Eberhardt RT. The current state of critical limb ischemia: a systematic review. JAMA Surg. 2016;151(11):1070-1077. Available from: https://doi.org/10.1001/jamasurg.2016.2018
- Chaudhry MA, Bashir M, Raza S, Rashid H, Ahmed S. Hybrid procedures in the management of complex peripheral arterial disease. Ann Vasc Surg. 2021;72:538-545.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
