International Journal of Dermatology and Clinical Research
Characterization of recessively inherited X-Linked ichthyosis in Bajaur Agency
1Department of Biotechnology, Shaheed Benazir Bhutto University, Sheringal, Dir (Upper), Pakistan
2School of Life Sciences, Henan University, Jinming Campus, Henan 475004, China
Author and article information
Cite this as
Ullah U, Shah AW, Ullah M, Ullah I (2023) Characterization of recessively inherited X-Linked ichthyosis in Bajaur Agency. Int J Dermatol Clin Res. 2023; 9(1): 1-6. Available from: 10.17352/2455-8605.000047
Copyright License
© 2023 Ullah U, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Recessively inherited X-linked Ichthyosis (XLI) is the second most generic form of Ichthyosis and is characterized by scaly, dry, thickened, and mild erupted skin. It is caused by a mutation in the STS gene ensuing lower production of Steroid sulfatase. A current study was performed to characterize XLI and its complications in patients of Bajaur Agency, Pakistan. We also wanted to record critical factors affecting the progression of XLI.
Methods: An Ichthyosis examination questionnaire was prepared and detailed information about the symptoms and management was recorded from 51 affected male patients of 17 families. Personal data such as age and gender were also recorded.
Results: Our results indicate that 53% of the patients were collodion while other symptoms appeared in the first month after birth. Almost every part of the patient has symptoms of the disease; scales were found on the extensor and flexor muscles (98%) of limbs followed by the ears (82.53%). All the patients had normal nails, palms and soles.
Conclusion: The age of the patients seems to have a significant effect on the color of the scales changing from white to brown to blackish. The disease progresses with the age and worsens in cold, dry seasons. The pedigrees of all families show that disease passes from generation to generation according to the classical X-linked recessive inheritance. We recommend early diagnosis and treatment for effective management of the condition. Further work is required to elucidate the genetic, biochemical, and environmental factors involved in the disease.
Ichthyosis represents a group of skin disorders characterized by scaly, dry and thickened skin. The term is derived from the Greek word “Ichthy” meaning Fish, the condition is called “Ichthyosis” because the patient’s skin gives the appearance of Fish-Scales. The most common signs include dry and scaly skin, hyperkeratosis, blisters, and excessive skin shedding. The symptoms of Ichthyosis include itching, overheating, and pain due to the injury of the living tissues of the Stratum Corneum [1]. X-linked Ichthyosis (XLI) is an X-linked recessive disorder thatmanifestsmild skin eruptions due to disturbance in the gene governing keratinization [2]. It affects approximately one out of 2000 to 6000 male population and has no geographical predilection. Typically, it develops by birth or in early infancy usually the first month, and extracutaneous manifestations are possible [3]. XLI is one of the five main types of Ichthyosis i.e.Lamellar Ichthyoses (LI), epidermolysis hyperkeratosis (EHK) or Bullous Ichthyosis (BI), Ichthyosis vulgaris (IV), Localized Ichthyosis. XLI is the second most common type of Ichthyosis after Ichthyosis vulgaris [4].
Steroid sulfatase (STS) is a microsomal enzyme that is membrane-bound and capable of hydrolyzing sulfated steroid hormones and cholesterol sulfate. STS catalyzes the conversion of sulfated steroid precursors to the free steroid [5]. A deficiency of this enzyme can result in XLI. Excessive skin scaling or hyperkeratosis is caused by the accumulation of unhydrolyzed cholesterol sulfate in the outer layers of the skin. Cholesterol sulfate is a sterol that stabilizes cell membranes and adds cohesion [6,7]. STS gene is located on the locus Xp22.3 on the distal short arm of the X-chromosome, a region associated with a high frequency of deletions. XLI is caused by a genetic defect or mutation in the STS gene [8]. In 90% of XLI patients, it is caused by complete deletion of the gene, and in 10% by point mutation or partial deletion of the STS gene. The origin of the X chromosome with the deletion of the STS gene is believed to be the grandfather of the proband [9].
XLI is characterized by glowing white color scaling during the initial stage which progresses to larger, dark scales affecting the extensor and sometimes flexor regions of the extremities, neck, and upper trunk [10]. The scales are usually spread equally all over the body, however, they are more visible on the extensor parts of the limbs, mainly on the lower extremities. The size of the scales varies from individual to individual however in general, they are bigger on the extensor areas of the legs. The face and head are typically not affected by the symptoms. The symptoms of this disease generally improve in the summer and worsen in the winter [11].
Female carriers rarely display a skin phenotype, they usually carry the genes of this disease and pass it to their male offspring (Sons). There have been few cases reported in females [12], it is thought that these women have inherited the ichthyosis gene from both sides of the family [13]. Affected men, married to non-carrier women must have unaffected sons because they transfer only Y-chromosomes to the sons, however, their daughters will be the next carriers [14].
There is no permanent cure for XLI however; doctors prescribe the treatment as per signs and symptoms. Mostly creams, lotions, or ointments are used to reduce skin dryness. The aim of treatment is the prevention and elimination of hyperkeratosis [15]. This study was performed to document the physiological, physical, and environmental factors involved in the progression of XLI in patients of Bajaur Agency, FATA, Pakistan. We have also examined various stages of the disease, and the degree of symptoms on different body parts of the patients.
Materials and methods
Survey area
We have collected the data of patients from the three Tehsils of Bajaur Agency; Khar, Salarzai, and Utmankhel. The combined population of this area is about 253,720 (GOP, 1998). The survey was conducted from July 2014 to June 2015.
Survey method
A questionnaire was prepared to collect specific information from the patients regarding personal information, family history, skin disease history, general medical history, dermatological examination, and physical appearance. Pictures were taken where appropriate. We also inquired about the seasonal effects and management practices employed by the patients.
Data analyses
The data was sorted into different tables in MS Excel, based on gender, age, and symptoms. A chi-square test was performed to see the difference between the actual ratio of XLI male progeny and the expected according to Mendelian genetics.
Results
Demography
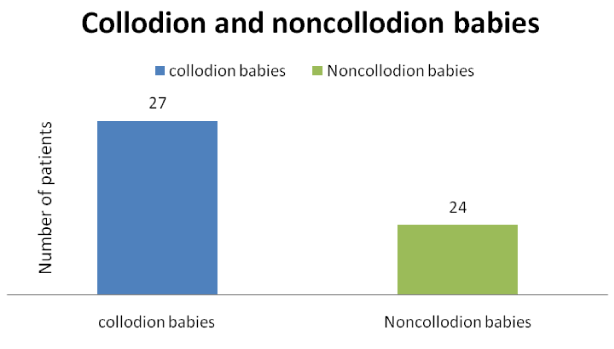
A total of 51 patients of XLI belonging to 17 families were recorded during this survey. The families were named XLI-1, XLI-2…. XLI-17. All patients were male, we could not find any female patients of XLI. Almost half (27) of the total 51 patients were born with the disease or were Collodion babies.
Epidemiology
Symptoms of ichthyosis were present in almost the whole body of the patients as presented in Table 1, especially the trunk and the limbs (Figure 1). However, the color and size of the scales varied.
Scalp
In the reported 51 patients only 6 XLI patients were observed with the affected scalp. Two of them were under ten years, 2 from ten to twenty, 1 under thirty, and 1 under forty years.
Face
In the observed 51 patients, only 3 patients were recorded with an affected face which is 6% of the total patients. All of them were in the age category of 10 to 20 years.
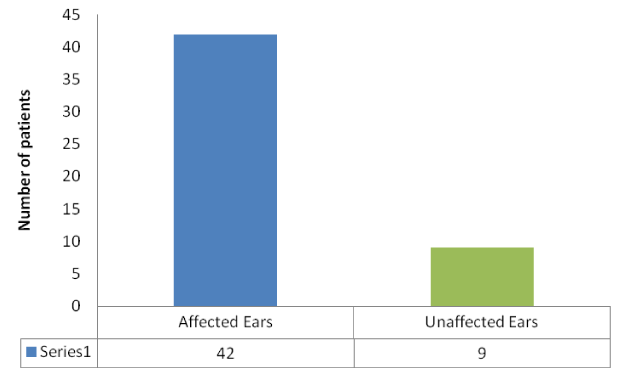
Ears
Scales on the ears and neck were observed in 42 patients out of 51, which is 82.53% of the total observed patients.
Extensor and flexor muscles
Except for one 27-year-old, all the patients of XLI had scales on their extensor and flexor muscles (50 out of 51). However, other body parts of that patient were affected.
Genital organs
Only one patient was reported who had symptoms on the genital organ. Shyness could be a reason for not revealing such kind of information to the public. People in rural areas in Pakistan are too shy even to talk about genital parts.
Hair loss
Hair loss symptom was rare in the patients of XLI. In the observed 51 patients, only 4 showed symptoms of scalp hair loss. A total of 3 patients were observed under 10 years and 1 patient under twenty years of age. Other patients in this family did not have this abnormality. The loss of body hair was also rare in the patients of XLI. Only 3 patients were observed to have lost the body hairs.
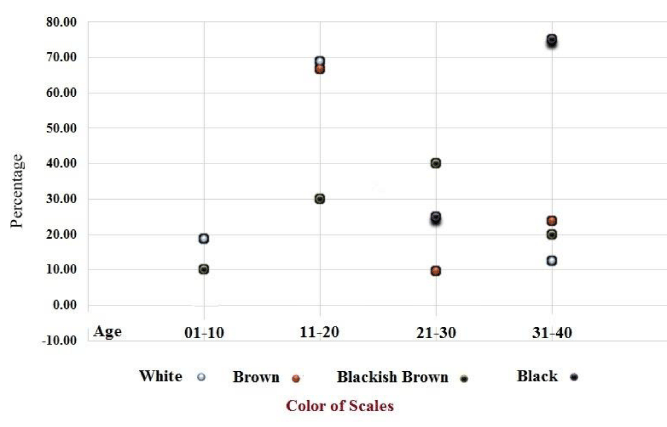
Color of scales
Scales of four colors were observed during the survey; white, brown, blackish-brown, and black. Twenty-eight patients had brown color scales, which is 55% of the total patients. The rarest color is white (4 patients), which is only 7.84% of the total visited patients. The second rare color is blackish-brown [7] which is 13.73%, and the third one is black color [13] which is 23.53%. When the percent color was drawn against the age of the patients. The white and brown scales were abundant (75%) in the younger patients from age 1 to 20 while, the brownish-black and black scales were mostly (71%) found in the older patients of age 21 to 40. The graphical representation is given in Figure 2.
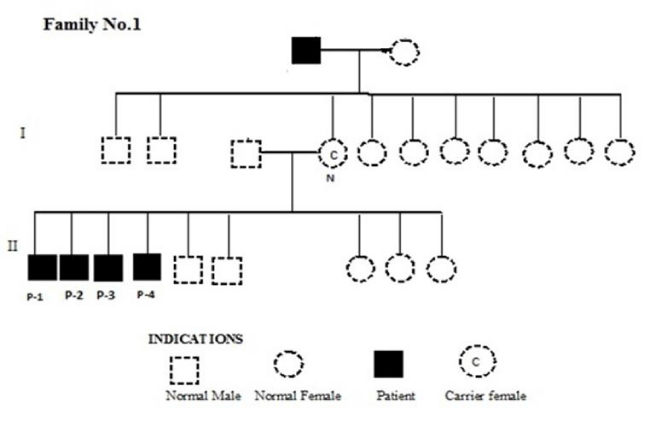
Pedigree analyses
In all the 51 patients and 17 families, the disease has traveled by female carrier mothers to the sons of affected maternal grandfathers (Figures 3-5). The chi-square test showed that in most cases, the actual percentage of total XLI patients was within the range of the distribution according to Mendelian inheritance of recessive traits (Tables 2,3). The ratio of XLI males was significantly higher than the expected 50% (at p = 0.05) in only two families; XLI-10 (χ2 = 0.004) and XLI-11 (χ2 = 0.025). These two families also took χ2 value of a total number of XLI progeny significantly higher than expected (χ2 = 0.00147).
Disease management
The patients reported that the condition is affected by the environment, i.e. in the winter season, this disease tends to be worse than in the summer. Most of the patients were from poor backgrounds and could not afford year-round expensive treatment. They usually used creams, lotions, or ointments during the wintry season to reduce skin dryness and ease the pain and itching. The basic knowledge of genetics and inheritance was lacking among the patients and their families. Furthermore, any kind of professional psychological help was non-existent in most cases.
Discussion
In the current study, 27 patients of XLI out of the total 51 were born collodion babies, which is more than half of the total patients. The symptoms of the disease appeared almost in the first month of their life, in the remaining 24 patients. Our observation is in accordance with that of Gånemo [14], who reported that a higher proportion of XLI patients were born as collodion babies. However, care must be taken of such children because, the collodion membrane offers a significantly decreased skin barrier function than the normal that may, consequently, increase trans-epidermal water loss [16]. Potential problems are hypothermia, dehydration, and hypernatremia. These conditions need cautious handling and treatment in a well-equipped neonatal care facility [11].
In this study, we observed scales on every part of the body of the XLI patients, especially the limbs and trunk. In all patients of the current study, soles, palms, and nails were observed normally. This observation is consistent with the previous reports, e.g. According to Cuevas-Covarrubias, et al. [6], the abdomen is more involved than the back and the scales are more spectacular over the extensor surfaces, pre-auricular areas, neck, and upper trunk with or without flexures involvement. Generally, palms and soles are spare and hair and nails are normal [10].
During the current survey, patients’ families have reported that the disease was more aggravated in childhood because the skin of infant patients was dry and light, and remained so till maturity however, with the passage of time symptoms show improvement. We also observed that the disease worsens in the winter season. But in the summer season, the skin was smoother and better in the same patients. Our observation is parallel with that of Hernández-Martin, et al. [15], who reported that hyperkeratosis improves during the warmer months of the year and worsens during the dry and colder months.
We observed a great variation in the color and size of the scales, and it seemed to be influenced by the age of the patient, as varied colors and sizes of scales were observed in different age groups. In the case of a neonatal baby, the skin is observed mild, light, and whitish color adherent scales on the stratum cranium. These observations agree with that of Cuevas-Covarrubias, et al. [6], who reported various sizes and colors of scales in different cases. Some of the patients were recorded with large plated scales on their extremities and some of them had small size black or brown scales, while a few patients were recorded with black color dotted spots in their stratum corneum. The scale’s color has also been reported to be influenced by environmental conditions. The color of the scales may appear light brown or brown in the summer season while blackish-brown or black in winter [4].
The results of the χ2-test showed that in fifteen families the distribution of XLI in the male offspring of carrier females was according to Mendelian rules of inheritance. Only two families (XLI-10, XLI-11) showed significant divergence in which 11 out of 12, and 5 out of 5 males were XLI patients. There was another family (XLI-14), in which 6 out of 7 males were XLI positive. These also affected the overall χ2 value of total numbers. We can only speculate the reasons behind this anomaly; some may say that it was just because of the chance mating of defective gametes. However, this complete dominance of XLI could be a result of gene recombination on the X chromosome during gamete formation in carrier females [17]. Furthermore, it is a well-known fact that the STS gene is located on the locus that is prone to all types of mutations and recombination [18,19]. We are planning a molecular exploration of these families to find further clues to solve this riddle.
During this survey, we observed increased shyness in XLI patients, and avoidance to answer the questions in detail. For example, only one out of 51 answered the question about symptoms in the genital area. These are the symptoms of social communication deficits. This fact has been acknowledged in a pivotal study by Kent, et al. (2008) [20]. They have also reported that children suffering from XLI are prone to attention deficit hyperactivity disorder (ADHD) and autism. Furthermore, XLI has been reported to affect individuals’ psychology to varying degrees in a worldwide online survey by Chatterjee, et al. (2016) [21].
Bajaur Agency has a very conservative environment, low literacy, and very little means to care for such chronic diseases. The effects of Ichthyosis on daily life and relations could be huge and have even been reported in developed countries [22]. Therefore, psychological help could do a lot of good for patients with such disorders. Furthermore, we recommend that genetic counseling regarding XLI and its inheritance pattern should be provided to the patients and their families. Efforts should also be made to eliminate social taboos about rare disorders. On the healthcare front, early/ prenatal diagnosis of XLI in carrier females can save a lot of resources. Researchers may work on developing ways for easier detection, and management of disease in a cost-effective manner.
Conclusion
This is a pioneering work in X-Linked Recessive Ichthyosis in Bajaur Agency. We gathered data from 51 male patients of XLI, most of whom were born with the disease, termed collodion babies. We observed high variation in the color and size of the scales, which seemed to be influenced by the age of the patient. Mostly the scales of younger patients were white in color and that of older ones were either brown or black. The condition is also affected by the environment, i.e. in the winter season this disease tends to be worse than in the summer. Furthermore, the patients showed symptoms of social communication deficits. In most families, the condition is inherited in Mendelian fashion of inheritance. We recommend early diagnosis and treatment for the effective management of the disease. Genetic counseling could be a viable way to provide information regarding inheritance and the prevention of disease. Further work is required to elucidate the genetic, environmental aMadnd biochemical factors involved in the progress of the disease.
Dr. Inaam Ullah was supported by Higher Education Commission, in Islamabad, Pakistan. We are grateful to patients and their families for their courage and cooperation throughout this study. This work is a precursor to future detailed molecular investigations into XLI.
- Vidyadhar TVV. A Review on Different Types of Ichthyosis and Management. PharmaTutor. 2015; 3(1):25-31.
- Fernandes NF, Janniger CK, Schwartz RA. X-linked ichthyosis: an oculocutaneous genodermatosis. J Am Acad Dermatol. 2010 Mar;62(3):480-5. doi: 10.1016/j.jaad.2009.04.028. Epub 2010 Jan 18. PMID: 20080321.
- Schmuth M, Martinz V, Janecke AR, Fauth C, Schossig A, Zschocke J, Gruber R. Inherited ichthyoses/generalized Mendelian disorders of cornification. Eur J Hum Genet. 2013 Feb;21(2):123-33. doi: 10.1038/ejhg.2012.121. Epub 2012 Jun 27. PMID: 22739337; PMCID: PMC3548255.
- Akiyama M. Updated molecular genetics and pathogenesis of ichthiyoses. Nagoya J Med Sci. 2011 Aug;73(3-4):79-90. PMID: 21928690; PMCID: PMC4831217.
- Elias PM, Williams ML, Choi EH, Feingold KR. Role of cholesterol sulfate in epidermal structure and function: lessons from X-linked ichthyosis. Biochim Biophys Acta. 2014 Mar;1841(3):353-61. doi: 10.1016/j.bbalip.2013.11.009. Epub 2013 Nov 27. PMID: 24291327; PMCID: PMC3966299.
- Cuevas-Covarrubias SA, Jiménez-Vaca AL, González-Huerta LM, Valdes-Flores M, Del Refugio Rivera-Vega M, Maya-Nunez G, Kofman-Alfaro SH. Somatic and germinal mosaicism for the steroid sulfatase gene deletion in a steroid sulfatase deficiency carrier. J Invest Dermatol. 2002 Oct;119(4):972-5. doi: 10.1046/j.1523-1747.2002.t01-1-00185.x. PMID: 12406347.
- Frascari F, Dreyfus I, Rodriguez L, Gennero I, Ezzedine K, Salles JP, Mazereeuw-Hautier J. Prevalence and risk factors of vitamin D deficiency in inherited ichthyosis: a French prospective observational study performed in a reference center. Orphanet J Rare Dis. 2014 Aug 5;9:127. doi: 10.1186/s13023-014-0127-3. PMID: 25091406; PMCID: PMC4237956.
- Cañueto J, Ciria S, Hernández-Martín A, Unamuno P, González-Sarmiento R. Analysis of the STS gene in 40 patients with recessive X-linked ichthyosis: a high frequency of partial deletions in a Spanish population. J Eur Acad Dermatol Venereol. 2010 Oct;24(10):1226-9. doi: 10.1111/j.1468-3083.2010.03612.x. PMID: 20236202.
- Preumont A, Rzem R, Vertommen D, Van Schaftingen E. HDHD1, which is often deleted in X-linked ichthyosis, encodes a pseudouridine-5'-phosphatase. Biochem J. 2010 Oct 15;431(2):237-44. doi: 10.1042/BJ20100174. PMID: 20722631.
- Dreyfus I, Bourrat E, Maruani A, Bessis D, Chiavérini C, Vabres P, Ezzedine K, Mazereeuw-Hautier J. Factors associated with impaired quality of life in adult patients suffering from ichthyosis. Acta Derm Venereol. 2014 May;94(3):344-6. doi: 10.2340/00015555-1710. PMID: 24158261.
- Vahlquist A, Bygum A, Gånemo A, Virtanen M, Hellström-Pigg M, Strauss G, Brandrup F, Fischer J. Genotypic and clinical spectrum of self-improving collodion ichthyosis: ALOX12B, ALOXE3, and TGM1 mutations in Scandinavian patients. J Invest Dermatol. 2010 Feb;130(2):438-43. doi: 10.1038/jid.2009.346. Epub 2009 Nov 5. PMID: 19890349.
- Ramesh R, Chen H, Kukula A, Wakeling EL, Rustin MH, McLean WH. Exacerbation of X-linked ichthyosis phenotype in a female by inheritance of filaggrin and steroid sulfatase mutations. J Dermatol Sci. 2011 Dec;64(3):159-62. doi: 10.1016/j.jdermsci.2011.07.006. Epub 2011 Aug 27. PMID: 21945601.
- Nagtzaam IF, Stegmann AP, Steijlen PM, Herbergs J, Van Lent-Albrechts JA, Van Geel M, Van Steensel MA. Clinically manifest X-linked recessive ichthyosis in a female due to a homozygous interstitial 1·6-Mb deletion of Xp22.31. Br J Dermatol. 2012 Apr;166(4):905-7. doi: 10.1111/j.1365-2133.2011.10685.x. Epub 2012 Feb 6. PMID: 21985695.
- Gånemo A. Hereditary ichthyosis: Causes, Skin Manifestations, Treatments and Quality of Life. Uppsala , Sweden: Acta Universitatis Upsaliensis; 2002.
- Hernández-Martin A, Aranegui B, Martin-Santiago A, Garcia-Doval I. A systematic review of clinical trials of treatments for the congenital ichthyoses, excluding ichthyosis vulgaris. J Am Acad Dermatol. 2013 Oct;69(4):544-549.e8. doi: 10.1016/j.jaad.2013.05.017. Epub 2013 Jul 16. PMID: 23870202.
- Oji V, Tadini G, Akiyama M, Blanchet Bardon C, Bodemer C, Bourrat E, Coudiere P, DiGiovanna JJ, Elias P, Fischer J, Fleckman P, Gina M, Harper J, Hashimoto T, Hausser I, Hennies HC, Hohl D, Hovnanian A, Ishida-Yamamoto A, Jacyk WK, Leachman S, Leigh I, Mazereeuw-Hautier J, Milstone L, Morice-Picard F, Paller AS, Richard G, Schmuth M, Shimizu H, Sprecher E, Van Steensel M, Taïeb A, Toro JR, Vabres P, Vahlquist A, Williams M, Traupe H. Revised nomenclature and classification of inherited ichthyoses: results of the First Ichthyosis Consensus Conference in Sorèze 2009. J Am Acad Dermatol. 2010 Oct;63(4):607-41. doi: 10.1016/j.jaad.2009.11.020. PMID: 20643494.
- Toral-Lopez J, González-Huerta LM, Cuevas-Covarrubias SA. Segregation analysis in X-linked ichthyosis: paternal transmission of the affected X-chromosome. Br J Dermatol. 2008 Apr;158(4):818-20. doi: 10.1111/j.1365-2133.2007.08405.x. Epub 2008 Jan 17. PMID: 18205863.
- Ali RH, Mahmood S, Raza SI, Aziz A, Irfanullah, Naqvi SK, Wasif N, Ansar M, Ahmad W, Shah SH, Khan BT, Zaman Q, Gul A, Wali A, Ali G, Khan S, Khisroon M, Basit S. Genetic analysis of Xp22.3 micro-deletions in seventeen families segregating isolated form of X-linked ichthyosis. J Dermatol Sci. 2015 Dec;80(3):214-7. doi: 10.1016/j.jdermsci.2015.09.007. Epub 2015 Sep 28. PMID: 26481779.
- Liu P, Erez A, Nagamani SC, Bi W, Carvalho CM, Simmons AD, Wiszniewska J, Fang P, Eng PA, Cooper ML, Sutton VR, Roeder ER, Bodensteiner JB, Delgado MR, Prakash SK, Belmont JW, Stankiewicz P, Berg JS, Shinawi M, Patel A, Cheung SW, Lupski JR. Copy number gain at Xp22.31 includes complex duplication rearrangements and recurrent triplications. Hum Mol Genet. 2011 May 15;20(10):1975-88. doi: 10.1093/hmg/ddr078. Epub 2011 Feb 25. PMID: 21355048; PMCID: PMC3080608.
- Kent L, Emerton J, Bhadravathi V, Weisblatt E, Pasco G, Willatt LR, McMahon R, Yates JR. X-linked ichthyosis (steroid sulfatase deficiency) is associated with increased risk of attention deficit hyperactivity disorder, autism and social communication deficits. J Med Genet. 2008 Aug;45(8):519-24. doi: 10.1136/jmg.2008.057729. Epub 2008 Apr 15. PMID: 18413370.
- Chatterjee S, Humby T, Davies W. Behavioural and Psychiatric Phenotypes in Men and Boys with X-Linked Ichthyosis: Evidence from a Worldwide Online Survey. PLoS One. 2016 Oct 6;11(10):e0164417. doi: 10.1371/journal.pone.0164417. PMID: 27711218; PMCID: PMC5053497.
- Mazereeuw-Hautier J, Dreyfus I, Barbarot S, Serrentino L, Bourdon-Lanoy E, Ezzedine K, Maza A, Aujoulat I, Le Rhun A. Factors influencing quality of life in patients with inherited ichthyosis: a qualitative study in adults using focus groups. Br J Dermatol. 2012 Mar;166(3):646-8. doi: 10.1111/j.1365-2133.2011.10701.x. PMID: 22014001.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
