International Journal of Dermatology and Clinical Research
Multiple Autoimmune Syndrome with Vitiligo, Autoimmune Thrombocytopenia and Autoimmune Dermoepidermal Bullous Dermatosis
1Department of Dermatology Venereology, Hassan II University Hospital Fez
2Department of internal medicine, Hassan II University Hospital Fez
Author and article information
Cite this as
Amraoui N, Meziane M, Lahlou A , Gallouj S, Rabhi S, et al. (2015) Multiple Autoimmune Syndrome with Vitiligo, Autoimmune Thrombocytopenia and Autoimmune Dermoepidermal Bullous Dermatosis. Int J Dermatol Clin Res. 2015; 1(1): 11-13. Available from: 10.17352/2455-8605.000005
Copyright License
© 2015 Amraoui N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Multiple auto-immune syndrome is defined by the coexistence of at least three different autoimmune diseases. Immune genetic predisposition and abnormalities of humeral and cell-mediated immunity seems to be implicated in their genesis.
In this observation, we describe a combination of three autoimmune diseases in the same patient namely vitiligo evolving since childhood, autoimmune dermo epidermal bullous dermatosis and autoimmune thrombocytopenia. The discovery of such associations may limit the therapeutic arsenal. And temporal sequence indicates that long-term surveillance of these patients is necessary to watch the occurrence of another autoimmune disease.
Multiple autoimmune syndrome is defined by the coexistence of at least three different autoimmune diseases which can occur simultaneously or over several years of evolution. We report an exceptional association of vitiligo, autoimmune thrombocytopenia and autoimmune dermoepidermal bullous dermatosis.
Observation
A young patient of 35 years presented since the age of 14 achromic non-painful or pruritic lesions which gradually extended to the level of the body. 4 years ago he developed intermittent oral and nasal erosions associated with red eyes and a decrease of visual acuity impeding his daily and professional activities. He also reported episodic appearance of some liquidiennes skin lesions without signs of infection or systemic disease.
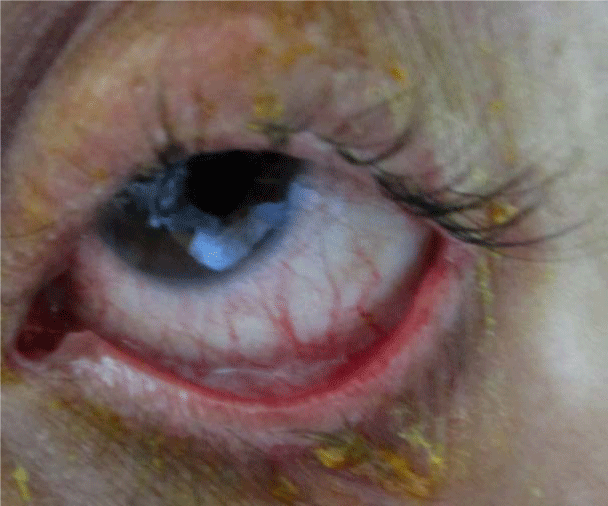
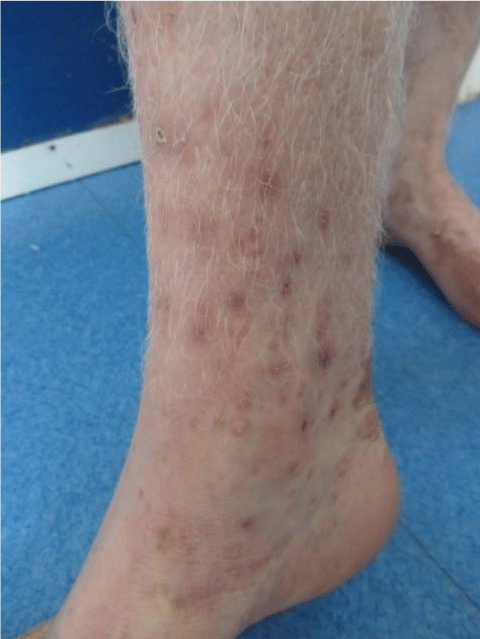
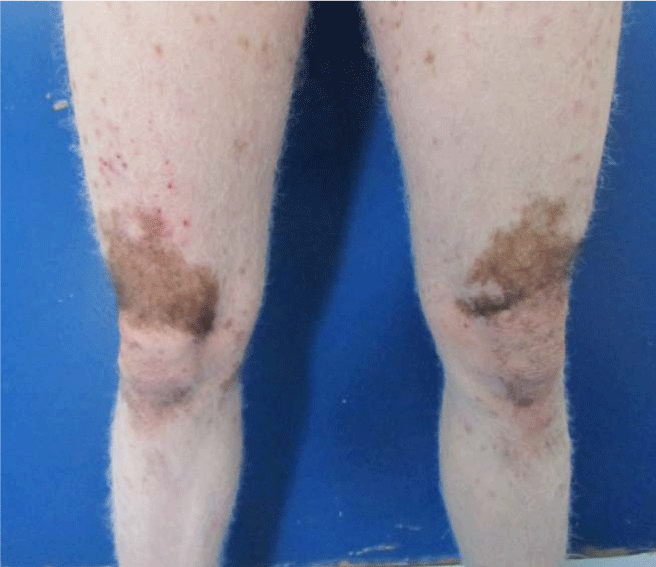
Ocular examination revealed bilateral red eyes with Symblepharon, and corneal dystrophy (Figure 1). Cutaneous examination revealed at the left leg the presence of tense bullae with clear contents based on healthy skin, associated with hemorrhagic erosions (Figure 2). The Nikolsky's sign was negative. There were also extensive achromic patches (Figure 3).
Laboratory test showed thrombocytopenia at 32000 / mm3. We completed the investigation by sternal puncture which showed a hypercellular marrow with megakaryocytic hyperplasia in support of a peripheral autoimmune origin. Thyroid and anti-nuclear antibody were negative. Conjunctively biopsy made by ophthalmologists initially objectified the presence of functional cleavage and direct immunofluorescence showed immunoglobulin G and complement C3 deposition in a linear band at the dermal-epidermal junction. The immune microscopy was not performed because this technique is not available in our hospital.
According to the clinical context and the results of immune histology we retained in our patient the combination of three autoimmune diseases: vitiligo, autoimmune thrombocytopenia with autoimmune bullous derma epidermal dermatitis most probably cicatricle pemphigoid. Epidermolysis bullosa acquisita that looks like cicatricle pemphigoid cannot be ruled out given the lack of examination by immune-microscopy.
The patient was initially put on oral corticosteroids at a dose of 1mg / kg / day until normalization of platelet levels. Then treatment with daps one at a dose of 2 mg / kg / day associated with mycofenolate mofetil at a rate of 2g / day was initiated with a clinical and laboratory monitoring. The evolution was marked by the stabilization of the disease and a slight improvement in ocular involvement.
Disscussion
We report a unique case characterized by the association of vitiligo, an autoimmune thrombocytopenia and autoimmune dermo epidermal bullous dermatosis in a male patient. It is still uncommon because different studies showed female predominance associations of auto-immune diseases [1].
Multiple autoimmune syndrome is a condition in which patients have at least three distinct autoimmune diseases [1], often with at least one dermatological condition, usually vitiligo or alopecia areata. Indeed in many cases of multiple autoimmune syndromes reported in the medical literature, vitiligo is the first autoimmune disease to be diagnosed. In these cases, the vitiligo is usually bilateral and symmetrical, which is illustrated by our observation. Autoimmune thyroid disease was also present in the multiple autoimmune syndrome including vitiligo [1]. It is not the case of our patient or may be not yet. In a predisposed person real cascade of autoimmune diseases may extend over several years (17 years in our case) and must therefore be watched to intervene on time. Other combinations are possible so we asked routinely laboratory tests to look for other most frequent associations which are anemia, diabetes, and systemic lupus. Other autoimmune related diseases are described in the literature as alopecia, inflammatory colitis, Myasthenia, Sjogren's syndrome, scleroderma, rheumatoid arthritis, psoriasis and pemphigus [2,3].
For autoimmune thrombocytopenia, its association with autoimmune derma epidermal bullous dermatitis has been reported in patients with bullous pemphigoid but has never been described with a cicatricle pemphigoid [4] or epidermolysis bullosa acquisita.
The presence of auto-immune disorders associated with cicatricial pemphigoid is increased compared to the risk of the general population. A study on a group of 34 patients with cicatricial pemphigoid showed that thirty-two percent of patients had autoimmune disease against 7% in the control population (p less than 0.002) [5,6]. Another study by Foster on a series of 130 patients followed for cicatricial pemphigoid noted the presence of autoimmune diseases associated in 17.7%, which is significantly higher compared to the 4% risk observed in the general population [5]. Associations reported in this context are lupus [7], rheumatoid arthritis [8], or mixed connectivitis [9,10].
For the epidermolysis bullosa acquisita, it has been reported in association especially with inflammatory colitis [11] with a few cases of association with multiple myeloma [12], psoriasis, rheumatoid arthritis, Hashimoto's thyroiditis and diabetes [13].
Autoimmune diseases involve genetic and environmental factors [14]. Concerning the genetic factor, the clinical observation of familial cases suggests that there are genes that predispose to such diseases, on the other hand once triggered the autoimmune disease amplifies via a cellular destruction mechanism that induce release of new auto antigens that were previously protected by a cytoplasmic or nuclear membrane, and have not been in contact with cells of the immune system. The immune system will then elicit immune responses against these «unknown» auto antigens [15,16].
Conclusion
The presence of autoimmune disease increases the risk of developing other autoimmune diseases indicating the need of monitoring of these patients.
- Humbert P, Dupond JL (1988) Multiple autoimmune syndromes. Ann Med Interne 139: 159-168 .
- Jacobson DL, Gange SJ, Rose NR, Graham NM (1997) Epidemiology and estimated population burden of selected autoimmune diseases in the United States. Clin Immunol Immunopath 84: 223 – 243 .
- Loftus EV, Sandborn WJ (2002) Epidemiology of inflammatory bowel disease. Gastroenterol Clin N Am 31: 1 – 20 .
- Gayle Taylor, Vanessa Venning, Fenella Wojnarowska (1993) Bullous pemphigoid and associated autoimmune thrombocytopenia: Two case reports. J Am Acad Dermatol 29: 900–902 .
- Nayar M, Wojnarowska F, Venning V, Taylor CJ (1991): Association of autoimmunity and cicatricial pemphigoid: is there an immunogenetic basis? J Am Acad Dermatol 25: 1011–1015 .
- Foster CS (1986) Cicatriciel pemphigoid. Trans Am Ophtalmol Soc 139: 159-168.
- Redman RS, Thorne EG (1981) Cicatricial Pemphigoid in a Patient with Systemic Lupus Erythematosus. Arch dermatol 117: 109-110 .
- Spigel GT, Winkelmann RK (1978) Cicatricial pemphigoid and rheumatoid arthritis. Arch Dermatol 114: 415-417 .
- Veien NK (2010): Bullous pemphigoid masquerading as recurrent vesicular hand eczema. Acta Derm Venereol 90: 4–5 .
- Malik M, Gürcan HM & Ahmed AR (2010): Coexistence of mucous membrane pemphigoid and connective-tissue disease. Clin Exp Dermatol 35: 156–159 .
- Hundorfean G, Neurath MF, Sitaru C (2010) Autoimmunity against type VII collagen in inflammatory bowel disease. J Cell Mol Med 14: 2393-2403 .
- Engineer L, Dow EC, Braverman IM (2002) Epidermolysis bullosa acquisita and multiple myeloma. J Am Acad Dermatol 47: 943-946 .
- Endo Y, Tamura A, Ishikawa O (1997) Psoriasis vulgaris coexistent with epidermolysis bullosa acquisita. Br J Dermatol 137: 783-786 .
- Gardner KM, Rajacich M (1985) Ophtalmological manifestations of adult rheumatoid arthritis and cicatriciel pemphigoid. Int Ophtalmol clin 25: 1-35 .
- Bonnott B (2004) Physiopathologie des maldies auto-immunes. Rev Med Interne 25: 648-658 .
- Vanderlugt CI, Neville KL, Nikcevich KM, Eagar TN, Bluestone JA, et al. (2000) Pathologic role and temporal appearance and newly emerging autoepitopes in relapsing experimental autoimmune encephalo-myelitis. J Immunol 164: 670-678 .
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
