Archives of Clinical Hypertension
Medication adherence and its associated factors among hypertensive patients in a tertiary health facility in Minna, North Central Nigeria
1B. Pharm, MSc (Clinical Pharmacy) Pharmacy Department IBB Specialist Hospital, Minna, Niger State, Nigeria
2B. Pharm. Pharmacy Department IBB Specialist Hospital, Minna, Niger State, Nigeria
3B. Pharm, MSc (Clinical Pharmacy) Department of Clinical Pharmacy and Pharmacy Practice, Ahmadu Bello University Zaria, Kaduna, Nigeria
4B. Pharm, MSc (Clinical Pharmacy) State House Medical Center, Asokoro Abuja, Nigeria
Author and article information
Cite this as
Usman MN, Umar MD, Idris FA, Abdullahi Y (2019) Medication adherence and its associated factors among hypertensive patients in a tertiary health facility in Minna, North Central Nigeria. Arch Clin Hypertens. 2019; 5(1): 3-7. Available from: 10.17352/ach.000021
Copyright License
© 2019 Usman MN, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Poor adherence to anti-hypertensive medications has caused increased cardiovascular risk and death. Nigerians have been shown to have a worse prognosis from hypertension, poor blood pressure control, and increased risk of complications arising from poor adherence to anti-hypertension medication.
Objective: The objective of this study was to assess anti-hypertensive medication adherence and associated factors among hypertensive patients attending a tertiary health facility in Niger State, Nigeria
Method: A hospital based cross-sectional study was conducted by administering Morisky medication adherence questionnaire to 237 study participants between February and May 2018.
Result: The overall adherence of participants to medication was 39.2% (n=237). Medication adherence was higher in younger participants (74.2%) and among females (52.7%). Similarly, adherence was more among those who took ≥3 pills (73.1%) and those who received pharmacist counseling (82.8%).
Conclusion: A low adherence level was observed in the study which needs to be recognized and improved through general adherence advocacy.
Hypertension is a major health problem in both developed and developing countries and is estimated to cause more than 13% of deaths annually [1]. It is a global public health issue affecting nearly one billion people and is estimated to increase to 1.56 billion adults by the year 2025, with two-thirds in developing countries [2,3]. Approximately 77.9 million American adults (1 in 3 people) and approximately 970 million people worldwide have high blood pressure (BP). The overall occurrence of hypertension is similar in men and women, but differs with age. For those younger than 45 years old, high BP is more common in men than women. For those 65 years old or older, high BP affects women more than men. African Americans (47% in women, 43% in men) develop high BP more often and at an earlier age, due to genetic predisposition, obesity and sensitivity to salt, inactivity and smoking. This is followed by Caucasians (31% in women, 33% in men) and Mexican Americans (29% in women, 30% in men). BP values increase with age, and hypertension is very common with the elderly. The lifetime risk of developing hypertension among those 55 years of age and older who currently have normal BP is 90% [4]. Optimal blood pressure (BP) control with levels below 140/90mmHg is associated with significant reduction in cardiovascular complications such as stroke and coronary heart disease [3]. Anti-hypertensive medication is one of the measures to manage hypertension to an optimal BP control level [2,4]. Adherence to anti-hypertensive medication is necessary for controlling blood pressure and preventing complications. However, certain factors affect hypertensive patient’s behavior regarding adherence to anti-hypertensive treatments. These factors can support or hinder adherence behavior. Some of these factors include patient related factors (e.g. socio-demographic), health system related factors (such as treatment cost and patients’ resources), and provider related factors (such prescriber-patient, pharmacist-patient relationship and communication). Although some studies have shown the prevalence of hypertension and factors associated with antihypertensive adherence in some parts of Nigeria [1,5,6], information about the level of medication adherence and its associated factors in the present study area is limited. Therefore, the aim of this study is to assess anti-hypertensive medication adherence and associated factors among hypertensive patients attending the Ibrahim Badamasi Babangida (IBB) Specialist Hospital Minna, Niger State, Nigeria.
Methods
Study design and Setting
This was a hospital based cross-sectional study to establish factors associated with adherence to antihypertensive medication. The study was conducted between February and May 2018. It was carried out at Ibrahim Badamasi Babangida (IBB) Specialist Hospital which is a tertiary health facility in Minna, the capital of Niger State in North Central Nigeria. The hospital has a bed capacity of 100, with staff enrolment including physicians in different specialties, pharmacists, nurses, laboratory scientists and technologists, physiotherapists and other ancillary health workers. It is specially equipped for the management of renal, cardiovascular, endocrine diseases, pediatric surgery, ear, nose and throat (ENT) and obstetrics and gynecology. There are two outpatient departments; the surgical outpatient department (SOPD) and medical outpatient department (MOPD) each on its days. Hypertension patients were followed up in the MOPD which holds twice every week, with an average of 30 patients attending each clinic.
Sampling size and procedure
The sampling frame included all hypertensive patients on follow up at the hospital hypertension clinics. Patients aged 18 years and above were eligible to participate in the study. Enrollment of study participants was carried out at the beginning of each clinic day. This was done at the MOPD desk where all patients report for their registration and appointment bookings. 237 study participants were selected by simple random sampling technique using the lottery method. Participants were informed on the need to participate only once. Patient informed consent was taken and proper records of enrolled patients were kept to avoid multiple enrollment.
Data collection tool and procedure
Data was collected by the principal researcher and a research attendant using a structured questionnaire. The data collection tool was pretested on approximately 10% of the sample size. These patients were excluded from the main study population. Necessary adjustments to the questionnaire were made as informed by the findings of the pilot study to improve on the reliability of the data to be collected in the main study. The questionnaire captured socio-demographic data and other patient related, disease related, medication related and organizational factors that may influence adherence to anti-hypertensive medication. The Morisky Green Levine Scale which has high reliability and validity was used for assessing patient adherence [20]. It measures both intentional and unintentional adherence based on forgetfulness, carelessness, stopping medication when feeling better, and stopping medication when feeling worse. Response categories were either yes or no for each item. In all, 0 point was allocated to a yes response and 1 point to a no response. The total score ranged from 0 (non-adherent) to 4 (adherent). The results were scored for all questions of medication adherence with a score of ≥3 classified as “having good adherence”.
Data processing and analysis
After each clinic day, data collected was entered into an excel spreadsheet where it was cleaned for errors and any other inconsistencies. At the end of data collection, the entire database in excel spreadsheet was categorized, coded and analyzed using Statistical Package for Social Sciences version 20 (SPSS Inc, Chicago, Illinois, USA). Pearson correlation was used to ascertain associations between adherence to anti-hypertensive medication and patient related, medication related, disease related and organizational factors. Descriptive statistics, frequency distribution tables and graphs were used to present the collected data. A p-value of less than 0.05 was considered statistically significant.
Ethical consideration
Clearance was sought from Research and Ethical Committee (REC) of Ibrahim Badamasi Babangida Specialist Hospital to carry out the study. Explanation to the study subjects on the purpose and the benefits of the study, confidentiality of their information and volunteerism was carried out in addition to obtaining an informed consent from the study subjects. Data obtained were treated with confidentiality at all times.
Results
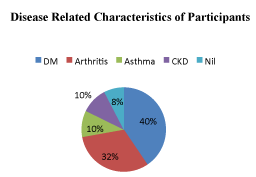
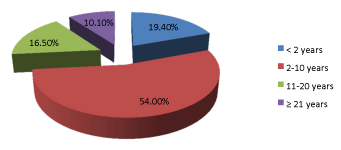
A total of 237 hypertensive patients participated in this study. The mean age of the participants was 40.5 years (SD=10.3 years), ranging from 23 to 64 years. 161 (67.9%) were female, 119 (50.2%) were from the Nupe ethnic group, and 120 (50.6%) were within the age of 40-60 years. More than two-thirds of the participants (79.7%) were married, and 93 (39.2%) were employed (Tables 1-3) (Figures 1,2).
Discussion
Adherence to medication is a key factor in preventing disease progression and complications. This study has identified some factors that contribute to lack of adherence to anti-hypertensive medication. Identifying these factors can give an insight into areas that needs intervention from prescribers and pharmacists. This study showed that 39.2% of hypertensive patients had good adherence to their antihypertensive medication. This implies that about two out of three patients are non-adherent to their medication. This finding was in line with those of studies done in Southwest Nigeria (44.7%) [1], and in Boston USA (34.6%) [7]. It was higher than studies done in Saudi Arabia (27.9%) [5], in urban and rural areas of Aligarh (23.7%) [8], and among hypertensive patients attending Government General Hospital Guntur, Andhra Pradesh (15.3%) [9]. However, it was lower than studies done in Kano, Nigeria (54.2%) [6], in Kiambu District Hospital Nairobi, Kenya (62%) [10], among hypertensive patients attending the Debre Tabor General Hospital, Northwest Ethiopia (75.1%) [2] and in rural India (73%) [11]. The possible reasons for the difference might be due to variations in the methods of measurement used to assess medication adherence among different participants, the study population, better access and care to patients in some of these countries. Another possible reason could be variations in the levels of education of participants. A statistical significant association was observed between patient age and medication adherence (r = 0.242, p < 0.05). Hypertensive patients’ ≥ 61 years were 25.8% less likely to adhere to their anti-hypertensive medication compared to younger respondents. This is consistent with findings of studies done among rural adults in India [11] and in Ethiopia [2]. The possible reasons might be that older patients take less medication in order to avoid cost burden. In particular, older adults managing other chronic conditions are more likely to experience financial difficulties as most are either retired or depends on family assistance. Also, age-related cognitive impairment, which is usually seen in older people might significantly reduce adherence to medication. In contrast, a study by Rao B.B et al showed that adherence rate towards antihypertensive medication was better among patient above 60 years of age (67.2%) and this was found to be statistically significant (p=0.02, OR (95% CI) = 1.91 (1.08-3.40) [12]. Female respondents were more adherent to their medication compared to male respondents (r = 0.262, p < 0.05). This is consistent with the findings of a study done in the medical outpatient clinics in Kiambu District Hospital, Nairobi, Kenya, and in India, where female respondents were more adherent than their male counterparts (p=0.024) [8,10]. This could be explained by the fact that men are burdened by the outdoor activities which make them busy and make them forget their medications. Also, many male respondents cited work related travelling and distance of the health facility as reasons for their poor adherence, while others question their BP status as they were normotensive until diagnosed during a routine checkup, and so does not see any need to take medication regularly. Female participants are likely to enjoy better family attention and support and even receive significant medical support from physicians and other hospital personnel. There was a negative significant correlation (r = -0.191, p = 0.003) between the duration of treatment of hypertension and medication adherence, with respondents treating hypertension for ≥21 being 25.8% less adherent to their medication compare to respondents treating hypertension for shorter duration. This is consistent with the finding of study done among individuals with hypertension in a Semi-Urban community of Southern Nigeria. The reason for this might be related to the fact that most hypertensive patients are not fully aware that managing their disease is lifelong. This could lead to patients being fade up with taking medication when they finally know the nature of regimen of management of their disease. The number of pills that patients were taking had a negative correlation with medication adherence (r = -0.002, p = 0.973). Patients who took ≥ 3 pills per day were three times as likely to adhere to their prescription compared to patients who took fewer pills per day. This finding is in line with those of a study done among Pakistani hypertensive patients [13], among hypertensive patients on follow up in public hospitals in Northern Ethiopia [14] , and in India [11]. This is however in contrast to what have been reported in other studies [2,10,12,15]. One reason for this finding could be that patients on multiple pills feel that the severity of their disease is significant and hence become more serious with their therapy, compared to those on ≤ 2 pills, who may take treatment lightly. Another reason may perhaps be that when patients have to take multiple pills, they are less likely to forget to take them, compared to having to take only one pill. There was also a significant negative correlation between side effects and medication adherence (r = -0.0475, p = 0.001). Respondents that did not experience any side effect were 83.9% more adherent than those that had side effects 16.1%. A study done in Greece reported that adverse drug effects were an issue of great concern for the majority of study participants. Some of them had stopped their treatment because they were afraid of the possible side effects [16]. In another study done in Botswana, 29.5% of respondents experienced adverse drug events and 17% out of this population stopped taking their medication [17]. It therefore means that drug adverse event experienced by patients impacts their medication adherence. Poor medication adherence could also be attributed to the cost of anti-hypertensive medication. Respondents that spent about three thousand naira (#3,000) were less adherent compared to those that spent lesser amount, and this was found to be statistically significant (r = 0.271, p = 0.001). This is consistent with the findings of studies done among hypertensive patients in North Central Nigeria [18], among patients in Ghana and Nigeria [3]. Majority (39.2%) of the participants were public servants earning monthly renumiration that may not take care of their family needs and paying for the cost of their medication could be a burden that may be difficult to consistently maintain.
A novel finding of this study was the interaction observed between patients and pharmacists. Respondents that had medication counseling from their pharmacists were 82.8% more adherent to their medication compared to those that did not receive any form of counseling 17.2%. Participants trusted their pharmacist’s advice on taking the appropriate medication for more serious conditions such as hypertension. Pharmacists counseled and provided additional information on treatment, such as whether patients should take the drug before or after meal, taking drugs in the mornings as with diuretics, advising patients on side effects of their medication and the consequences of non-adherence with treatment. This was consistent with the findings of studies done in Nigeria and Greece [18-20]. Several studies within and outside Nigeria and African only reported the finding associated with patient-physician relationship, without significant consideration to patient-pharmacists relationship [2,6,10]. Pharmacists can assist patients respect the intervals of drug administration, the number of doses, and effectiveness of treatment or avoid interactions. Pharmacists can equally give information to hypertensive patients that each drug lowers blood pressure in a unique and individual manner to help achieve their blood pressure goals. Offering patient’s adherence aids like patient information leaflets for example, to assist them in adhering to their therapy and also talking to patients about refilling anti-hypertensive medication in the pharmacy. Advising patients to carry a personal medication record (PMR) and to develop a relationship with their pharmacist to help with medication adherence.
There were several limitations to this study, even though patient self-report is a simple and inexpensive way of assessing adherence and has been used extensively throughout the literature, it may not provide a true picture of actual adherence as a primary measure of adherence to medication. Recall bias could have under estimated or overestimated the level of adherence reported in the study. Patients may generally give overly optimistic reports about adherence so as not to disappoint the researchers. Also the sample size of our study is small to generalize the findings to a large extent. This is due to the fact that the study center is a referral facility and not a general hospital. However there is a paucity of literature on adherence to anti-hypertensive medications in the study setting. Further studies are recommended across the area to assess the adherence level as well as the various other factors influencing it.
Conclusion
Adherence to anti-hypertensive medication was low (39.2%). However, age, gender, number of pills and pharmacist counseling are some of the factors affecting adherence. These findings could be an opportunity for adherence interventions to be carried out on vulnerable groups and also promoting the importance of adherence among patients and health care providers.
Authors’ contribution
MNU conceived, designed, executed the work and wrote the manuscript. MDU contributed in data collection and management. FAI and AY contributed in writing of the manuscript and reviewed the entire work.
The authors wish to thank Pharm. Alfa Isah, consultant pharmacist at the Niger State Hospitals Management Board and Ndagi Umar PhD, head of pharmacy department IBB Specialist Hospital Minna, Niger State, for their immense contribution during the design and data collection. We also acknowledge Dr. Shafi’u Moh’d of the department of clinical pharmacy and pharmacy practice Faculty of Pharmaceutical Sciences Ahmadu Bello University Zaria, for his ideas and guidance.
- Ajayi EA, Adeoti AO, Ajayi IA, Ajayi AO, Adeyeye VO (2013) Adherence to Antihypertensive Medications and Some of Its Clinical Implications in Patients Seen At a Tertiary Hospital in Nigeria. Journal of Dental and Medical Sciences 8: 36–40. Link: https://tinyurl.com/yyon2u3u
- Destaw F, Teshome K, Bantie B, Yohannes H, Abebaw A (2017) Medication adherence and its associated factors among hypertensive patients attending the Debre Tabor General Hospital, Northwest Ethiopia. Dove Press Journal 1–7. Link: https://tinyurl.com/y4rcbpt5
- Boima V, Ademola AD, Odusola AO, Agyekum F, Nwafor CE, et al. (2015) Factors Associated with Medication Nonadherence among Hypertensives in Ghana and Nigeria. Int J Hypertens 1: 8. Link: https://tinyurl.com/yxrybqxg
- Alsolami F, Hou X, Correa-velez (2012) Factors Affecting Antihypertensive Treatment Adherence : A Saudi Arabian Perspective. Clinical Medicine and Diagnostics 2: 27–32. Link: https://tinyurl.com/y49b9srp
- Kabir M, Iliyasu Z, Abubakar IS, Jibril M (2004) Compliance to medication among hypertensive patients in Murtala Mohammed Specialist Hospital, Kano, Nigeria. Journal of Community Medicine & Primary Health Care 16: 16–20. Link: https://tinyurl.com/y3n4pnhz
- Ulasi II, Ijoma CK, Onodugo OD (2010) A Community-Based Study of Hypertension and Cardio-Metabolic Syndrome in Semi-Urban and Rural Communities in Nigeria. BMC Health Serv Res 10: 71. Link: https://tinyurl.com/y4pjzecl
- Hashmi SK, Afridi MB, Abbas K, Sajwani RA, Saleheen D (2007) Factors Associated with Adherence to Anti-Hypertensive Treatment in Pakistan. PLoS One 20. Link: https://tinyurl.com/yxlqahep
- Ali MA, Bekele ML, Teklay G (2014) Antihypertensive medication non-adherence and its determinants among patients on follow up in public hospitals in Northern Ethiopia. International Journal of Clinical Trials 1: 95–104. Link: https://tinyurl.com/y5wn7hef
- Asha K, Sneha DM, Avinash S, Sravan K, Reddy T, et al. (2016) Assessment of treatment adherence among hypertensive patients in a coastal area of Karnataka, India. International Journal of Community Medicine and Public Health 3. Link: https://tinyurl.com/y2u6ye7l
- Koulierakis G, Kyriopoulos J (2010) Factors affecting adherence to antihypertensive medication in Greece : Results from a Qualitative Study. Dove Press Journal 2010: 335–343. Link: https://tinyurl.com/yyrt4677
- Naar-king S, Kaljee LM, Panthong A, Koken JA (2010) Applying the Information-Motivation-Behavioral Skills Model in Medication Adherence Among Thai Youth Living with HIV : Aids patient care and stds 24: 787-794. Link: https://tinyurl.com/yyp9qgaq
- Saseen JJ, MacLaughlin (2014) Hypetension Pharmacotherapy: A pathophysiologic approach. New York. McGraw-Hill Medical 338-445.
- Lulebo AM, Mutombo PB, Mapatano MA, Mafuta EM, Kayembe PK (2015) Predictors of non‑adherence to antihypertensive medication in Kinshasa , Democratic Republic of Congo: a cross ‑ sectional study. BMC Research Notes 8: 526. Link: https://tinyurl.com/y4ovhwv6
- Srivastava AK, Kandpal SD, Sati H (2015) Predictors for Adherence in Hypertensive Therapy- A Study in Rural Area of District Dehradun, Indian. Journal of Community Health 27. Link: https://tinyurl.com/y6pjh3pz
- Svensson S (2006) Medication Adherence, Side Effects and Patient-Physician Interaction in Hypertension. Link: https://tinyurl.com/y4ms4gta
- Olin BR, June T (2018) Hypertension: The Silent Killer: Updated JNC-8 Guideline Recommendations. Alabama Pharmacy Association. Link: https://tinyurl.com/y2bp3k8c
- Kırılmaz A, Naharc İ, Pınar M, Yılmaz MB, Uzun M (2009) The effect of the content of the knowledge on adherence to medication in hypertensive patients. Anadolu Kardiyol Der 9: 183–188. Link: https://tinyurl.com/y2qkrgg6
- Hernandez-vila E (2015) A Review of the JNC 8 Blood Pressure Guideline. Tex Heart Inst J 42: 226–228. Link: https://tinyurl.com/y3hv7mr6
- Hedna K, Hakkarainen KM, Gyllensten H, Jönsson AK (2015) Adherence to Antihypertensive Therapy and Elevated Blood Pressure : Should We Consider the Use of Multiple Medications? PLoS One 1-14. Link: https://tinyurl.com/yxq7cd4j
- Morisky DE, Green LW, Levine DW (1986) Concurrent and predictive validity of a self-reported measure of medication adherence. Medical Care 24: 67-74. Link: https://bit.ly/2XTyXt6
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
