Archives of Clinical Hypertension
Isolated systolic hypertension in young adults and its relationship with ambulatory blood pressure measurements
1Cardiometabolic Diseases Unit, San Martin Hospital, La Plata, Buenos Aires, Argentina
2Faculty of Medical Sciences, National University of La Plata, Argentina
Author and article information
Cite this as
Espeche W, Minetto J, Stavile N, Cerri G, Sisnieguez CL, et al. (2024) Isolated systolic hypertension in young adults and its relationship with ambulatory blood pressure measurements. Arch Clin Hypertens. 2024; 10(1): 1-6. Available from: 10.17352/ach.000034
Copyright License
© 2024 Espeche W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: The definition of Isolated Systolic Hypertension (ISH) is accepted by guidelines, which adopt a blood pressure (BP) cutoff point of 140/90 mmHg, with elevated Systolic Blood Pressure (SBP) and normal diastolic blood pressure (DBP) in the clinic. This phenotype represents the most common form of Hypertension (HT) in young individuals.
The prognosis of ISH differs according to various explanatory mechanisms. Some associations of this phenotype with Ambulatory Blood Pressure Monitoring (ABPM) have been described, but little emphasis has been placed on its association with nocturnal BP values. To the best of our knowledge, there is no epidemiological data on young patients establishing this relationship in Latin America.
Objective: To describe the characteristics of ISH in our population of young patients and analyze its relationship with different ABPM phenotypes.
Materials and methods: Consecutive adult individuals between 16 and 40 years of age, without antihypertensive treatment, were evaluated in a cross-sectional study. They were referred for ABPM to a tertiary hospital between July 2013 and August 2022.
Each individual underwent an initial interview, three BP measurements using current standards with OMROM HEM 705 devices, and subsequent ABPM with Spacelabs 90207.
A general description of the sample was provided, and an analysis was conducted based on different patient phenotypes determined by clinic BP measurements in relation to various ABPM phenotypes.
Results: A total of 395 individuals (69% women, 29 ± 6.5 years) were finally evaluated. The frequencies according to clinic phenotypes were as follows: Normotensive = 77%, ISH = 6%, HT = 17%.
Among the ISH group, 29.2% had white coat hypertension (WCH). The Kappa agreement was 31% for clinic phenotypes vs. ABPM. Among ISH patients, 37% had at least one elevated period (daytime or nighttime), and 12.5% had elevated BP only during the nighttime.
The definition of Isolated Systolic Hypertension (ISH) is widely accepted by international guidelines, which adopt a Blood Pressure (BP) cutoff point of 140/90 mmHg [1-3]. Thus, systolic BP values above that threshold with normal diastolic BP are sufficient to confirm this condition. Remarkably, this phenotype represents the most common form of arterial hypertension in young individuals [1-3].
The prognosis of ISH differs according to the age of onset, being a seemingly benign condition in young individuals [4]. This is due to greater arterial elasticity, which allows peripheral arteries to increase the pulse wave without causing vascular wall damage [5]. However, several considerations should be taken into account: 1) the young population has various definitions and cutoff points, ranging from before the age of 30 to 50 [2] which is crucial as the pathophysiological mechanisms differ 2) the initial description of ISH predates the recognition of other non-benign mechanisms associated with ISH (arterial stiffness, increased renin-angiotensin system activity, and increased peripheral resistance) [6]; 3) most studies that showed ISH as a benign condition are predominantly cohorts of non-smoking, disease-free, and lean men [7].
On the other hand, ISH is related to ambulatory blood pressure measurements, but no study has emphasized its association with nocturnal blood pressure values [8]. Moreover, to the best of our knowledge, there is no epidemiological data on young patients with this relationship in Latin America [9]. Therefore, our objective is to describe the characteristics of young adult individuals with ISH and analyze the relationship with ambulatory blood pressure.
Materials and methods
A non-probabilistic consecutive cross-sectional sample of adult individuals aged 16 to 40 years without antihypertensive treatment was evaluated. They were referred for Ambulatory Blood Pressure Monitoring (ABPM) to the Cardiometabolic Diseases Unit of the Hospital San Martín de La Plata from July 2013 to August 2022. Pregnant women or those in the postpartum period (< 3 months) and individuals with known secondary hypertension were excluded from this study.
Each individual underwent an initial interview lasting approximately 15 minutes, which collected personal, epidemiological, and social data, cardiovascular history, and risk factors (smoking, dyslipidemia, diabetes, use of antihypertensive medications). Subsequently, measurements of body weight with loose clothing and without shoes were taken using a scale (Femto Mod.03). Weight was estimated in kilograms (kg) and height in meters (m), calculating the body mass index using the formula weight/height2. Waist Circumference (WC) and Neck Circumference (NC) were measured in a standing position above the iliac crests and cricothyroid cartilage, respectively.
After completing this stage, specially trained nurses performed three Office Blood Pressure (OBP) measurements using validated automated devices (OMRON HEM 705), using appropriate cuffs for each patient’s arm circumference [10]. These measurements were taken with the patient sitting and supported, legs uncrossed and resting on the floor, without any clothing compressing the arm, and without speaking. Immediately after, ABPM was applied using a validated oscillometric device (Spacelabs 90207 - Spacelabs On track). Measurements were scheduled every 15 minutes during the day and every 20 minutes during the night. The daytime and nighttime periods were defined according to the patient’s diary, and studies with more than 70% of the scheduled measurements and at least one measurement per hour were considered valid.
Office Blood Pressure (OBP) was defined as the average of these three measurements, and based on the OBP values, the sample was divided into: Normotension (values below 140/90 mmHg), Isolated Systolic Hypertension (systolic value above 140 and diastolic values below 90 mmHg), Hypertension (diastolic values above 90 mmHg regardless of systolic BP).
According to ABPM, four phenotypes were defined: 1) Normal blood pressure (both daytime and nighttime periods < 135/85 and < 120/70 mmHg, respectively), 2) Isolated Daytime hypertension (Daytime BP ≥ 135/85 mmHg with nocturnal BP < 120/70 mmHg), 3) Isolated Nighttime hypertension (Nocturnal BP ≥ 120/70 mmHg with daytime BP < 135/85 mmHg), 4) Sustained arterial hypertension (hypertension in both periods).
Furthermore, based on 24-hour ABPM values, the following categories were defined: 1) Isolated systolic hypertension (systolic BP > 130 mmHg and diastolic BP < 80 mmHg [ISH]), 2) Normotension (BP < 130/80 mmHg), 3) Diastolic hypertension (diastolic BP > 80 mmHg regardless of systolic BP).
For the description of categorical variables, frequencies were expressed as percentages, while means or medians were used to describe quantitative variables, as appropriate.
Differences between groups were assessed using the chi-square test for categorical variables, while differences between quantitative variables were analyzed using ANOVA or the Kruskal-Wallis test depending on the variance analysis and normality of the data.
The correlation between office-based phenotypes and ABPM phenotypes was assessed using the Kappa correlation coefficient. Pearson or Spearman correlation was also performed, as appropriate, to correlate office-based systolic and diastolic blood pressure values with their respective ABPM values.
Statistical analysis was conducted using SPSS version 25.0. A two-tailed p-value of <0.05 was considered statistically significant for all tests performed.
The study was conducted under the standards of the 2013 Helsinki Declaration and approved by the institutional research ethics committee (PROTOCOL NO. HSMLP2023/0109) and registered with the joint health research commission (EX-2023-42522616 - -GDEBA-CCISMSALGP).
Results
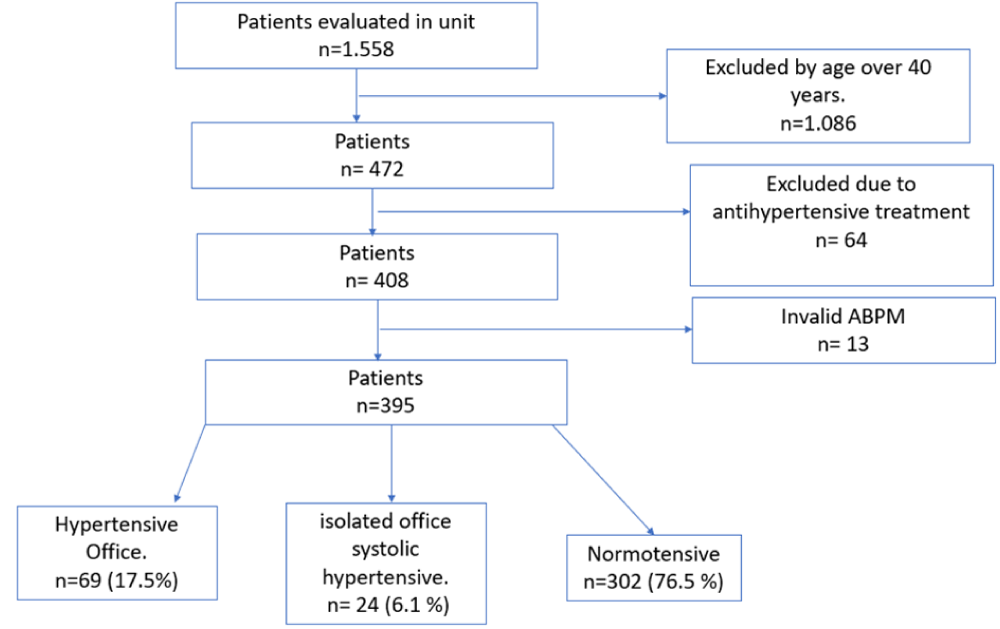
A total of 1 558 individuals were evaluated, of which 472 were between 16 and 40 years old. Sixty-four individuals were excluded due to pharmacological antihypertensive treatment, and 13 individuals were excluded due to an invalid ABPM. The remaining 395 individuals (69% women, 29 ± 6.5 years) constituted the study sample (Figure 1).
Table 1 presents the differences between the BP categories according to office-based blood pressure (BP-office): 1- Normotensive (77%), ISH (6%), and Arterial hypertension (17%). Individuals with ISH were more frequently male, younger, and had a larger neck circumference compared to other phenotypes.
Table 2 compares the BP categories with the ABPM phenotypes. It is important to note that approximately 30% of individuals with isolated systolic hypertension were normotensive on ABPM (white coat hypertension).
The agreement between the PA-Con categories and ABPM phenotypes was statistically significant but low (K = 31%). Similarly, the correlation between office-based blood pressure and 24-hour blood pressure was significant for both systolic and diastolic measurements (r = 0.62 and r = 0.63, respectively), with lower correlations observed for nighttime blood pressure measurements (r = 0.56 and r = 0.59, respectively).
Among individuals with ISH in the office setting (n = 24), 9 of them (37%) were hypertensive in at least one period on ABPM (daytime/nighttime) regardless of the 24-hour value. Twelve-point five percent (n = 3/24) of individuals with ISH had elevated blood pressure only during the nighttime period (isolated nocturnal hypertension), and 25% (6/24) had hypertension only during the daytime period (isolated daytime hypertension).
The mean values of mean arterial pressure for individuals with isolated nocturnal and daytime elevations were 90 ± 3.8 mmHg and 93 ± 4.7 mmHg, respectively.
Discussion
This study showed that 6.1% of young adults have ISH. Although the frequency cannot be directly compared to Latin America due to limited data, it is similar to that described in studies in young subjects in Asia (5.2%) [11] the United Kingdom (8%) [7], and Italy (6.8%) [8]. However, there are differences in the published data that need to be highlighted. Our study shows that the proportion of women with ISH is superior to those in other studies (29% vs. 6-10%). This may be partly attributed to the fact that our basal sample had a higher proportion of women (69% vs. ~30%) and that our patients had larger neck circumference(38 cm) and body mass index compared to other studies (~30 vs. 25) [12,13]. Both of these conditions are risk factors for the development of obstructive sleep apnea syndrome, which is more commonly observed in this type of patient population [14]. Additionally, our study demonstrates that the most common office-based blood pressure phenotype is systo-diastolic arterial hypertension rather than ISH [9].
Likewise, in our sample, there was a greater number of women, as we have mentioned, which could modify this prevalence. In the long term, although the risk of stroke may be lower [15,16]; The systolic blood pressure value where events occur in females is usually lower, with what this implies [17]. Likewise, the curve of blood pressure elevation in women has a greater slope, surpassing that of men after age 60 [18].
Thirty percent of individuals with ISH in the office setting have normal blood pressure on ambulatory blood pressure monitoring (white coat hypertension). Citoni, et al. [8] previously demonstrated this correlation with even higher coefficients (R=0.62 vs. 0.73). However, their study included individuals up to 50 years old, and approximately 45% of them were under pharmacological treatment (white coat effect) [8]. Therefore, our study emphasizes the importance of using measurements outside the office setting to confirm this phenotype. Furthermore, a recent meta-analysis evaluating the long-term cardiovascular risk of white coat hypertension showed an increased incidence of arterial hypertension and future cardiovascular diseases [19].
One-third of individuals with ISH had isolated hypertension in either the daytime or nighttime period, with 12.5% of them being hypertensive only during the nighttime period (isolated nocturnal hypertension). While this phenotype has been described in the general population by Liu [20], the prevalence was similar to our study, highlighting the importance of performing ambulatory blood pressure monitoring over home blood pressure monitoring. Therefore, being able to detect this phenotype in young and healthy individuals could lead to specific prevention and monitoring strategies.
Lastly, the correlation between nighttime measurements and office measurements is significant but of lesser value than 24-hour and daytime measurements. Therefore, the absolute value of office blood pressure alone should not be a reason for performing ambulatory blood pressure monitoring. This was described by Salazar, et al. [10], who found no difference in the frequency of isolated nocturnal hypertension among hypertensive and normotensive individuals based on office categories (optimal, normal, high-normal, and arterial hypertension).
New analyses of ABPM have been recently published. Palatini, et al. [21] described a parameter related to the incidence of sustained hypertension and the need for pharmacological treatment in young individuals with ISH. They demonstrated that mean daytime blood pressure values ≥ 97 mmHg double the risk of progressing to sustained hypertension and the need for pharmacological treatment within 6 years of follow-up. While a considerable percentage of individuals in our study with ISH had mean blood pressure below this cutoff point (90 mmHg for isolated nighttime hypertension and 93 mmHg for isolated daytime hypertension), one-third of them had these isolated elevated periods with the aforementioned implications.
Currently, isolated systolic hypertension does not have a specific prognosis, it is a heterogeneous condition and therefore the recommendations of the latest European guidelines [22] are not clearly issued regarding the time to start pharmacological treatment. However, the treatment decision is based on expert recommendations to evaluate the risk-benefit [22] and extrapolation of the benefits in other age ranges [23,24].
This study has some limitations that should be addressed. First, the individuals evaluated, although presumed to be “healthy,” were referred to a specialized unit for ABPM. Therefore, the results may not be widely applicable to the general population. Second, the phenotypes of arterial hypertension were determined based on a single office blood pressure measurement visit. However, these measurements were performed following international measurement standards and were compared with the ABPM performed on the same day. Finally, the lack of a standardized survey on physical activity and sleep quality and disorders could not identify factors that might have influenced the frequency of isolated nocturnal hypertension phenotype.
As a limitation, it must be taken into account that since it is a heterogeneous condition with different phenotypes [25,26], evaluating the long-term prognostic risk with an evaluation of 24-hour ambulatory measurements without taking into account other risk factors is imprudent.
Despite these limitations, our study demonstrates that the frequency of isolated systolic hypertension (ISH) in young individuals is like that reported in other countries. One-third of these individuals are not confirmed by ambulatory blood pressure measurements (white coat hypertension), and more than 30% of those with confirmed ambulatory hypertension are only classified based on measurements during isolated periods, with over 12% of them having isolated nocturnal hypertension. Finally, although the prognosis of ISH remains under discussion, it is crucial to continue prospective follow-up studies in young and healthy individuals to further elucidate this issue.
Conclusion
Isolated systolic hypertension is a heterogeneous entity reported in some countries as the most common subtype of hypertension in young patients. In this cross-sectional study, it is observed that systo-diastolic hypertension is more frequent even among the young. Other significant differences reported include a higher percentage of women with this condition based on our sample, which could imply different pathophysiological mechanisms and prognoses.
The use of 24-hour ambulatory blood pressure monitoring was of great importance as it uncovered a high percentage of white coat hypertension (30%), as well as other types of masked hypertension such as isolated nocturnal hypertension. The prognostic value of this condition has not been studied, and its implications should be evaluated in the future.
We would like to thank the following nurses: Mr. Jorge Belaunzaran, Ms. Irma Acero, and Ms. Celeste Rios. Former nurse: Ms. Susana Cor. Secretary: Mr. Juan Pablo Schuman.
Who work and collaborate with us in the unit.
- Unger T, Borghi C, Charchar F, Khan NA, Poulter NR, Prabhakaran D, Ramirez A, Schlaich M, Stergiou GS, Tomaszewski M, Wainford RD, Williams B, Schutte AE. 2020 International Society of Hypertension Global Hypertension Practice Guidelines. Hypertension. 2020 Jun;75(6):1334-1357. doi: 10.1161/HYPERTENSIONAHA.120.15026. Epub 2020 May 6. PMID: 32370572.
- Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, Clement DL, Coca A, de Simone G, Dominiczak A, Kahan T, Mahfoud F, Redon J, Ruilope L, Zanchetti A, Kerins M, Kjeldsen SE, Kreutz R, Laurent S, Lip GYH, McManus R, Narkiewicz K, Ruschitzka F, Schmieder RE, Shlyakhto E, Tsioufis C, Aboyans V, Desormais I; ESC Scientific Document Group. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018 Sep 1;39(33):3021-3104. doi: 10.1093/eurheartj/ehy339. Erratum in: Eur Heart J. 2019 Feb 1;40(5):475. PMID: 30165516.
- Mahmud A, Feely J. Spurious systolic hypertension of youth: fit young men with elastic arteries. Am J Hypertens. 2003 Mar;16(3):229-32. doi: 10.1016/s0895-7061(02)03255-7. PMID: 12620702.
- O'Rourke MF, Vlachopoulos C, Graham RM. Spurious systolic hypertension in youth. Vasc Med. 2000;5(3):141-5. doi: 10.1177/1358836X0000500303. PMID: 11104296.
- Papadakis JA, Ioannou P, Theodorakopoulou V, Papanikolaou K, Vrentzos G. Metabolic profile of patients with isolated systolic hypertension. Hormones (Athens). 2021 Jun;20(2):377-380. doi: 10.1007/s42000-020-00266-y. Epub 2021 Jan 6. PMID: 33409906.
- Bavishi C, Goel S, Messerli FH. Isolated Systolic Hypertension: An Update After SPRINT. Am J Med. 2016 Dec;129(12):1251-1258. doi: 10.1016/j.amjmed.2016.08.032. Epub 2016 Sep 14. Erratum in: Am J Med. 2017 Sep;130(9):1128. PMID: 27639873.
- McEniery CM, Yasmin, Wallace S, Maki-Petaja K, McDonnell B, Sharman JE, Retallick C, Franklin SS, Brown MJ, Lloyd RC, Cockcroft JR, Wilkinson IB; ENIGMA Study Investigators. Increased stroke volume and aortic stiffness contribute to isolated systolic hypertension in young adults. Hypertension. 2005 Jul; 46(1):221-6. doi: 10.1161/01.HYP.0000165310.84801.e0. PMID: 15867140
- Citoni B, Figliuzzi I, Presta V, Cesario V, Miceli F, Bianchi F, Ferrucci A, Volpe M, Tocci G. Prevalence and clinical characteristics of isolated systolic hypertension in young: analysis of 24 h ambulatory blood pressure monitoring database. J Hum Hypertens. 2022 Jan;36(1):40-50. doi: 10.1038/s41371-021-00493-9. Epub 2021 Feb 15. PMID: 33589761.
- Scott H, Barton MJ, Johnston ANB. Isolated systolic hypertension in young males: a scoping review. Clin Hypertens. 2021 Jun 15;27(1):12. doi: 10.1186/s40885-021-00169-z. PMID: 34127066; PMCID: PMC8204426.
- Salazar MR, Espeche WG, Balbín E, Leiva Sisnieguez CE, Minetto J, Leiva Sisnieguez BC, Maciel PM, Stavile RN, Carbajal HA. Prevalence of isolated nocturnal hypertension according to 2018 European Society of Cardiology and European Society of Hypertension office blood pressure categories. J Hypertens. 2020 Mar;38(3):434-440. doi: 10.1097/HJH.0000000000002278. PMID: 31584523.
- Atasoy S, Middeke M, Johar H, Peters A, Heier M, Ladwig KH. Cardiovascular mortality risk in young adults with isolated systolic hypertension: findings from population-based MONICA/KORA cohort study. J Hum Hypertens. 2022 Dec;36(12):1059-1065. doi: 10.1038/s41371-021-00619-z. Epub 2021 Oct 14. Erratum in: J Hum Hypertens. 2023 Apr;37(4):330. PMID: 34650215; PMCID: PMC9734041.
- Saladini F, Santonastaso M, Mos L, Benetti E, Zanatta N, Maraglino G, Palatini P; HARVEST Study Group. Isolated systolic hypertension of young-to-middle-age individuals implies a relatively low risk of developing hypertension needing treatment when central blood pressure is low. J Hypertens. 2011 Jul;29(7):1311-9. doi: 10.1097/HJH.0b013e3283481a32. PMID: 21659824.
- Fan HQ, Li Y, Thijs L, Hansen TW, Boggia J, Kikuya M, Björklund-Bodegård K, Richart T, Ohkubo T, Jeppesen J, Torp-Pedersen C, Dolan E, Kuznetsova T, Stolarz-Skrzypek K, Tikhonoff V, Malyutina S, Casiglia E, Nikitin Y, Lind L, Sandoya E, Kawecka-Jaszcz K, Imai Y, Ibsen H, O'Brien E, Wang J, Staessen JA; International Database on Ambulatory Blood Pressure In Relation to Cardiovascular Outcomes Investigators. Prognostic value of isolated nocturnal hypertension on ambulatory measurement in 8711 individuals from 10 populations. J Hypertens. 2010 Oct;28(10):2036-45. doi: 10.1097/HJH.0b013e32833b49fe. PMID: 20520575.
- Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013 May 1;177(9):1006-14. doi: 10.1093/aje/kws342. Epub 2013 Apr 14. PMID: 23589584; PMCID: PMC3639722.
- Thomas Q, Crespy V, Duloquin G, Ndiaye M, Sauvant M, Béjot Y, Giroud M. Stroke in women: When gender matters. Rev Neurol (Paris). 2021 Oct;177(8):881-889. doi: 10.1016/j.neurol.2021.01.012. Epub 2021 Jun 22. PMID: 34172293.
- Poorthuis MH, Algra AM, Algra A, Kappelle LJ, Klijn CJ. Female- and Male-Specific Risk Factors for Stroke: A Systematic Review and Meta-analysis. JAMA Neurol. 2017 Jan 1;74(1):75-81. doi: 10.1001/jamaneurol.2016.3482. PMID: 27842176.
- Ji H, Kim A, Ebinger JE, Niiranen TJ, Claggett BL, Bairey Merz CN, Cheng S. Sex Differences in Blood Pressure Trajectories Over the Life Course. JAMA Cardiol. 2020 Mar 1;5(3):19-26. doi: 10.1001/jamacardio.2019.5306. Erratum in: JAMA Cardiol. 2020 Mar 1;5(3):364. PMID: 31940010; PMCID: PMC6990675.
- Ji H, Niiranen TJ, Rader F, Henglin M, Kim A, Ebinger JE, Claggett B, Merz CNB, Cheng S. Sex Differences in Blood Pressure Associations With Cardiovascular Outcomes. Circulation. 2021 Feb 16;143(7):761-763. doi: 10.1161/CIRCULATIONAHA.120.049360. Epub 2021 Feb 15. PMID: 33587655; PMCID: PMC7884079.
- Cohen JB, Lotito MJ, Trivedi UK, Denker MG, Cohen DL, Townsend RR. Cardiovascular Events and Mortality in White Coat Hypertension: A Systematic Review and Meta-analysis. Ann Intern Med. 2019 Jun 18;170(12):853-862. doi: 10.7326/M19-0223. Epub 2019 Jun 11. PMID: 31181575; PMCID: PMC6736754.
- Li Y, Staessen JA, Lu L, Li LH, Wang GL, Wang JG. Is isolated nocturnal hypertension a novel clinical entity? Findings from a Chinese population study. Hypertension. 2007 Aug;50(2):333-9. doi: 10.1161/HYPERTENSIONAHA.107.087767. Epub 2007 Jun 18. PMID: 17576859.
- Palatini P, Saladini F, Mos L, Fania C, Mazzer A, Casiglia E. Clinical characteristics and risk of hypertension needing treatment in young patients with systolic hypertension identified with ambulatory monitoring. J Hypertens. 2018 Sep;36(9):1810-1815. doi: 10.1097/HJH.0000000000001754. PMID: 30005026.
- Palatini P. The HARVEST: looking for optimal management of young people with stage 1 hypertension. Panminerva Med. 2021 Dec;63(4):436-450. doi: 10.23736/S0031-0808.21.04350-0. Epub 2021 Mar 12. PMID: 33709681.
- Probstfield JL, Applegate WB, Borhani NO, Curb JD, Cutler JA, Davis BR, Furberg CD, Hawkins CM, Lakatos E, Page LB, et al. The Systolic Hypertension in the Elderly Program (SHEP): an intervention trial on isolated systolic hypertension. SHEP Cooperative Research Group. Clin Exp Hypertens A. 1989;11(5-6):973-89. doi: 10.3109/10641968909035386. PMID: 2676266.
- Amery A, Birkenhäger W, Bulpitt CJ, Clément D, De Leeuw P, Dollery CT, Fagard R, Fletcher A, Forette F, Leonetti G, et al. Syst-Eur. A multicentre trial on the treatment of isolated systolic hypertension in the elderly: objectives, protocol, and organization. Aging (Milano). 1991 Sep;3(3):287-302. doi: 10.1007/BF03324024. PMID: 1764497.
- Bourdillon MT, Song RJ, Musa Yola I, Xanthakis V, Vasan RS. Prevalence, Predictors, Progression, and Prognosis of Hypertension Subtypes in the Framingham Heart Study. J Am Heart Assoc. 2022 Mar 15;11(6):e024202. doi: 10.1161/JAHA.121.024202. Epub 2022 Mar 9. PMID: 35261291; PMCID: PMC9075287.
- Lurbe E, Torro MI, Alvarez-Pitti J, Redon P, Redon J. Central blood pressure and pulse wave amplification across the spectrum of peripheral blood pressure in overweight and obese youth. J Hypertens. 2016 Jul;34(7):1389-95. doi: 10.1097/HJH.0000000000000933. PMID: 27088634.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
